Diabetes is one of the most common, chronic conditions in the world. It is the leading cause of new cases of blindness in working-age adults. Nearly 24 million people are now affected by diabetes in the United States (8% of the American population). In fact, this number has risen by three million in the last two years alone. Another 57 million individuals are estimated to have pre-diabetes, a condition that puts them at risk for diabetes. And, approximately 25% of those with diabetes don’t know they have it—on a positive note, that’s a 5% decrease from two years ago.
According to the Centers for Disease Control and Prevention, someone with diabetes loses visual function every 15 minutes.1 Diabetes can also cause serious health complications, including heart disease, kidney failure and lower-extremity amputations. Even more alarming, diabetes is the seventh leading cause of death in the United States.1
Although the statistics indicate that more people are developing diabetes, the numbers also show that there is increasing awareness about the condition’s causes and overall prevalence. The good news is that with increased awareness and appropriate care, many complications from diabetes can be delayed or avoided. The Diabetes Control and Complication Trial (DCCT), for instance, found that intensive blood glucose control reduced the risk of eye disease by 76%, kidney disease by 50% and nerve disease by 60%.2 According to the Early Treatment of Diabetic Retinopathy Study (ETDRS), 50% of blindness caused by DR could have been prevented with the early diagnosis of diabetes and early detection of retinal complications.3
As essential health care providers for patients with diabetes, optometrists have both the capacity and responsibility to increase patient awareness about the condition, facilitate early detection, and assist in disease management and treatment. This article provides insight on how optometrists can better educate their patients about diabetes management, and offers several useful resources to help improve patient care—including a road map on how to become a Certified Diabetes Educator.
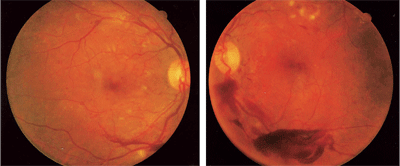
This patient presented with bilateral proliferative diabetic retinopathy (O.D. left, O.S. right). Note the presentation of cotton wool spots, disc neovascularization and preretinal hemorrhage (O.S.>O.D.). We educated this patient about her condition and convinced her that she had a significant problem that would eventually compromise her eyesight. The retinal specialist followed her closely and asked her to return to my office for additional education, because the patient remained reluctant to pursue care.
Certified Diabetes Educators
Diabetes educators provide specialized training and care for people with diabetes. They give general information about diabetes and its causes, create individual self-management plans, and make sure that a patient is comfortable testing and recording blood glucose levels. Diabetes educators are also trained to manage psychological issues and various complications related to hypo- and hyperglycemia. They can assemble a team of health care professionals, as well as gather support from a network of family and friends.
As optometrists, we already do a lot of this in day-to-day practice. Therefore, optometrists are eligible to become certified diabetes educators (C.D.E.).
A C.D.E. has reached a high level of clinical and technical knowledge, passed a national exam and is up-to-date regarding diabetes care (C.D.E.s must apply for recertification every five years). Eligibility requirements include:
• A minimum of two years of professional practice experience.
Diabetes may be diagnosed by one of the following tests: 1. Fasting plasma glucose (FPG). FPG measures blood glucose in someone who has not eaten in at least eight hours. Fasting plasma glucose equal to or greater than 126mg/dL is indicative of diabetes. 2. Oral glucose tolerance (OGTT). OGTT measures blood glucose after a person fasts for at least eight hours, and then drinks a specialized high-glucose beverage. Two hours after ingestion, a blood glucose level is taken again. 3. Random plasma glucose testing (RPG). RPG measures blood glucose without regard to when the person last ate or drank. A doctor can diagnose diabetes (but not pre-diabetes) with a RPG of 200mg/dL or greater and obvious symptoms (e.g., polyuria, polydipsia and polyphagia). Test results should be confirmed with a second test on a different day.
• A minimum of 1,000 hours of diabetes self-management experience (at least 400 of those hours must be accrued in the most recent year preceding the exam).
• A minimum of 15 clock hours of continuing education activities that are applicable to diabetes within two years of initial application.
Here, Dr. MacDonald educates a patient about the potential impact of diabetes on his vision.
Optometrists as Diabetes Educators
Essential Testing Strategies for Diabetes
Increasing patient awareness through education is an area where optometrists must be key players and active participants within a diabetes health care team. Optometrists also are in a unique position in that we understand the complications and serious nature of the disease. However, we are not often perceived as traditional health care providers who are involved in diabetes education and management.
On subsequent visits, many patients have told me that they realized the importance of good diabetes care after learning the particulars of their condition. They mentioned that receiving education about diabetes from a person whom they had initially considered an unexpected source was very helpful.
“Being a C.D.E. has enhanced my practice, but not all O.D.s will want to pursue C.D.E. certification,” says Roger Phelps, O.D., C.D.E., of Ojai, Calif. “I would recommend, however, that most O.D.s (especially those working with a lot of patients with diabetes) join the American Association of Diabetes Educators (AADE). As a member of AADE, the O.D. can network with other professional providers of diabetes care and establish a relationship in their local community that can benefit their patients with diabetes.”
Use every opportunity to educate not only patients, but also other health care providers regarding optometry’s role on the diabetes care team. Additionally, you must emphasize that comprehensive dilated eye exams are a necessity. In her annual address, Ann Albright, Ph.D., R.D., director of the CDC’s Diabetes Translation Section, mentioned that the numbers of documented dilated eye exams are down. “We need to do a better job of sustaining a multidisciplinary team approach to our patients’ care by communicating all findings of dilated eye exams,” said Dr. Albright.
The Importance of Communication
Effective communication and collaboration with the rest of the diabetes care team results in optimum patient care and decreased overall costs. Such efforts also can increase your referral base.
I have many referral sources from as far as 30 miles away, even though I know that there are closer eye doctors. I believe that other diabetes care providers truly value the information I share with them and their patients.
Members of a diabetes management team often includes: the patient, the primary care doctor, an endocrinologist, a dietician, a nurse educator, an eye care provider, a podiatrist and a dentist. In addition, an exercise consultant, a pharmacist, and other necessary professionals may be included.
A study conducted by the Center for the Partially Sighted showed that regular input and guidance from such diabetes management groups had a positive impact on patients’ HbA1c levels, even in visually impaired individuals.5 Furthermore, an Australian study documented results that showed patients in multidisciplinary care have improved metabolic control and decreased cardiovascular risk factors.6
• Type 1. Type 1 diabetes is an autoimmune disease that destroys the insulin-producing beta cells of the pancreas. It generally occurs during childhood or the young-adult years. Between 5% and 10% of Americans with diabetes have type 1. • Type 2. In type 2 diabetes, the pancreas still produces insulin; however, it is not used well by the body’s tissues (insulin resistance). Eventually, insulin production is diminished. The sweeping majority of Americans with diabetes have type 2. • Gestational. Gestational diabetes typically occurs between the 24th and 28th week of pregnancy. It is a form of glucose intolerance. Five percent to 10% of women with gestational diabetes are found to already have one form of diabetes (usually type 2). Additionally, women who develop gestational diabetes have a 25% to 50% chance of being diagnosed with diabetes five to 10 years after pregnancy. • Pre-diabetes. Pre-diabetes is a condition where blood glucose levels are higher than normal, but not yet high enough to be diagnosed as diabetes. “Impaired glucose tolerance” is defined as two-hour glucose levels of 140mg/dL to 199mg/dL (7.8mmol/L to 11.0mmol/L) on the 75g oral glucose tolerance test, and “impaired fasting glucose” is defined as glucose levels of 100mg/dL to 125mg/dL (5.6mmol/L to 6.9mmol/L) in fasting patients. The Diabetes Prevention Program reported that DR has been found in nearly 8% of individuals with pre-diabetes.4
Coordinating care can be a challenge when there are multiple providers. This consideration becomes even more difficult when these health care professionals are
scattered over a variety of locations. Establishing solid relationships and utilizing available channels of communication is essential.
Primary Forms of Diabetes
The best way to establish good working relationships is through personal contact. Start by sending a letter of introduction and requesting a face-to-face meeting. Mention that you’ll be following up with a phone call. This can prevent awkwardness, because the other health care provider will already be somewhat familiar with you.
During the meeting, be sure to ask how the provider best receives information. Many busy professionals ask staff members to file report letters that come in the mail, and may never read them until the patient comes in for a visit. A “to the point” e-mail or voicemail may be equally or even more effective. Additionally, professionals are now requesting e-mail referrals, where photos or other pertinent information can be attached.
The American Optometric Association (AOA) has excellent diabetes report forms that you may purchase from its catalog if you do not want design your own report letter. The AOA’s “Healthy Eyes Healthy People” program also has health record cards that patients can carry in their wallets to each visit.
Regardless of your approach, just be sure to communicate actively with everyone on the diabetes health care team. You should also establish a referral system for routine preventative care as well as for urgent needs. Don’t simply tell the patient with a potentially serious problem to consult a specialist right away. Contact primary care and specialty providers to discuss specific criteria and ensure that procedures are in place for seeing a patient who is referred for preventive or urgent care.
Along those lines, specific messages sent directly from a specialized health care provider are much more effective than generalized requests (e.g., “I notice that your foot looks ulcerated; I recommend that you need to see a podiatrist. Let me give you a referral list”).
We already take detailed patient histories and are trained to identify both primary and secondary problems. You don’t need to be an expert or take much time to identify problems that require attention from a specialist in another discipline.
Make a list of providers, case managers, phone numbers, and other contact information and keep it handy for quick reference. Consider designing handouts with referral information, or calling clinics directly for urgent referrals. Many assisted living communities, hospitals and health agencies, and Veteran’s Administration facilities also have diabetes care programs.
The bottom line––you must communicate openly and effectively with your patient. The manner in which you deliver information is essential. You must also encourage and support self-management techniques.
Traditionally, medical information has been given in a “top-down” fashion. That outdated approach often hits patients with an unsavory feeling of condescension––“I am the expert, you are the patient.” Such methods generally don’t work well. Commanding someone who has a chronic condition to comply with a certain behavior rarely motivates him or her to actually exhibit the desired behavior. The “fear tactic” is a short-term motivator at best, and it certainly doesn’t treat the patient as a member of the care team.
Communication based on the motivational interviewing technique has been shown to help patients who have chronic conditions (such as diabetes) modify lifestyle behaviors to maintain optimum health. When speaking with diabetes patients, don’t forget to address the following:
1. Establish a rapport by trying to understand the patient’s perspective.
2. Do not be judgmental, especially if the patient shows resistance to change.
3. Help the patient appreciate the value of healthy change.
4. Help the patient identify nescessary areas of change, and elicit a commitment to a change in their behavior.
5. Motivate patients by acknowledging and complimenting them when they have changed their behavior.
Items to discuss include: general diabetes education, smoking cessation, diet and exercise, medications, self-monitoring of blood glucose, and any problems or potential problems identified during your history and exam (e.g., stress or suspected sleep apnea). Be sure to explain the complications of uncontrolled diabetes and the benefits of regular exams.
You also can refer the patient to a pharmacist for a blood glucose monitor.
Important Discussion Points, Questions and Resources for Diabetes Patients
Resources for Educators
Promote the ABCs—A1C, Blood Pressure and Cholesterol:
Ask about Health Examinations:
• Controlling the ABCs can prevent complications and reduce the risk of stroke and heart attack.
• Foot exams
• Ask, “Do you know your ABC goals and how to reach them?”
• Dilated Eye exams
• Explain that poor ABC control can also lead to problems in foot, eye and oral health.
• Oral health exams
• ABC monitoring and control
Promote a Healthy Lifestyle:
• Weight control
• Healthy food choices
• Daily physical activity
• Daily foot care
• Support self-management
• Eye care
• No tobacco use (Call 1-800-QUITNOW)
• Daily oral care
• Monthly oral self-exam
Explain the Risks and Benefits of Comprehensive Diabetes Control:
• Selection and use of a blood glucose monitor
• Know your ABC goals and how to reach them
• Foot health
• Eye health
• Medication management
• Oral health
• Drug therapy management
Assess Symptoms that Require Referral:
• Foot symptoms
• Eye symptoms
• Oral symptoms
• Medication-related symptoms• National Certification Board of Diabetes Educators
1-847-228-8469
www.ncbde.org
• American Association of Diabetes Educators
1-800-338-3633
www.aadenet.org
• American Optometric Association
243 North Lindbergh Boulevard
St. Louis, MO 63141
1-800-365-2219
www.aoa.org
AOA catalog/order department
1-800-262-2210
www.aoa.org/documents/Order-DeptCatalog.pdf
Final Suggestions
• The ABCs of diabetes. Reinforce the importance of good metabolic control by emphasizing the ABCs of diabetes––A1C, blood pressure and cholesterol.
• One step at a time. Don’t address everything at one exam. Have a list of items that you can check off, and concentrate on the most pertinent concerns at any one visit. Representatives from the National Diabetes Education Program created a table that can help you generate several important questions (see “Important Discussion Points and Questions for Diabetes Patients, left).7 This table outlines concepts that you should discuss with patients who have diabetes, including ocular and oral health considerations as well as drug therapy management. Always communicate the need for prudent metabolic control.
• AADE 7. Another useful approach is to inform your patients about the AADE’s Seven Self Care Behaviors (AADE 7): 1. Healthy eating; 2. Being active; 3. Monitoring (blood glucose); 4. Taking medications; 5. Problem solving; 6. Reducing risk; 7. Healthy coping. “The prevalence of diabetes is so huge, one person cannot do it all alone,” says Deborah Fillman, M.S., R.D., L.D., C.D.E., president of the AADE. “Diabetes education is not in a vacuum. The AADE is looking at other professionals to get the message out.”
• Prepare your patients. Finally, prepare your patient for visits to your practice as well as visits to other professionals’ offices. Inform your patients that it’s a good idea to write down specific concerns/questions prior to their visits. This goes for family members as well. Discuss the importance of keeping accurate and complete records. Review your patients’ questions, goals and plans. Also, ask your patients to have their other care providers send their clinical information to your office. (They may not think of it unless you ask them.)
We have an important place in the care of our patients with diabetes. Because we understand the effects of diabetes, are good at educating our patients, and have a different relationship with these patients than other members of their health care team, we can not only save vision, but save lives.
Dr. MacDonald has served as the Los Angeles Unified School District’s low vision specialist and has been involved in low vision rehabilitation at the Center for the Partially Sighted since 1991. She is also an adjunct professor at the Southern California College of Optometry.
1. The Centers for Disease Control and Prevention. National Diabetes Fact Sheet, 2007. Available at: www.cdc.gov/diabetes/pubs/pdf/ndfs_2007.pdf (Accessed August 27, 2010).
2. The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med. 1993 Sep 30;329(14):977-86.
3. Early Treatment Diabetic Retinopathy Study Research Group. Photocoagulation for diabetic macular edema. Early Treatment Diabetic Retinopathy Study report number 1. Arch Ophthalmol. 1985 Dec;103(12):1796-806.
4. Knowler WC, Barrett-Connor E, Fowler SE, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med. 2002 Feb 7;346(6):393-403.
5. Thompson P. Pyschological Counciling and Support Groups. Available at: http://low-vision.org/en/Our_Services_Psychological_Counseling_And_Support_Groups (Accessed August 27, 2010).
6. Zwar NA, Hermiz O, Comino EJ, et al. Do multidisciplinary care plans result in better care for patients with type 2 diabetes? Aust Fam Physician. 2007 Jan-Feb;36(1-2):85-9.
7. Aung B, Ball WL Jr, Caporusso JM, et al. Working together to manage diabetes. The National Diabetes Education Program. Available at: http://ndep.nih.gov (Accessed September 1, 2010).

