 Keratoconus, pellucid marginal degeneration (PMD) and post-LASIK ectasia are difficult conditions to manage and treat. These progressive ocular diseases have frustrated patients because of the need for multiple changes to spectacles and contact lenses, and eventually the need for full-thickness penetrating keratoplasty.
Keratoconus, pellucid marginal degeneration (PMD) and post-LASIK ectasia are difficult conditions to manage and treat. These progressive ocular diseases have frustrated patients because of the need for multiple changes to spectacles and contact lenses, and eventually the need for full-thickness penetrating keratoplasty.
Fortunately, researchers continue to uncover new ways to manage and treat such ectatic diseases. One such option: collagen cross-linking with riboflavin and ultraviolet-A (UVA) light.
Collagen Cross-Linking
The cornea is a lamellar structure and has multiple layers of collagen that cross-link to create stability and uniformity. Throughout an individuals lifetime, researchers have observed that exposure to ultraviolet radiation and increased intake of riboflavin may contribute to improved cross-linking and greater corneal rigidity.1,2 This explains why older patients demonstrate tighter collagen cross-linking of the corneas and skin than younger patients.3
Enzymes, such as collagenase, proteinase and matrix metalloproteinase (MMP), may play a crucial role in corneal breakdown associated with keratoconus.4-6 Research has demonstrated, however, that eyes treated with collagen cross-linking are more resistant to corneal degeneration caused by these enzymes.7
For example, one study showed that rabbit corneas treated with collagen cross-linking using riboflavin and UVA demonstrated a significant increase in corneal collagen diameter and biomechanical stability.8 Another study revealed an impressive increase of 329% in corneal rigidity in human corneas after collagen cross-linking.9
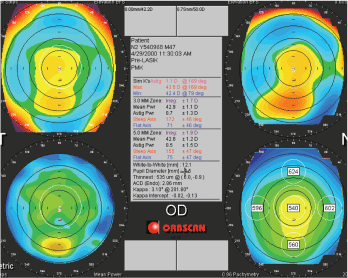
On Orbscan (Bausch & Lomb), this patient demonstrated forme frust keratoconus O.D. If progression continues, he may be a candidate for collagen cross-linking.
The Procedure
The procedure involves removal of the epithelium to expose the cornea to UVA radiation at a rate of 3mW/cm2, while administering riboflavin drops for 30 minutes. Although research has shown no thermal injury to corneal collagen, there is a risk of endothelial cytotoxicity from riboflavin/UVA exposure.10 Thus, the treatment depth with the UVA laser should not exceed 400m.11
Patients whose corneas are thinner than 400m should not undergo collagen cross-linking. Since there is significant corneal thinning associated with keratoconus or post-LASIK ectasia, an accurate pachymetry assessment is always essential.
The preliminary results of collagen cross-linking have been successful. At the 2007 European Society of Cataract and Refractive Surgeons meeting in
He also showed that patients best-corrected visual acuity improved following surgery. At two years, uncorrected visual acuity improved from 20/100 to 20/40, and best-corrected visual acuity improved by more than one Snellen line.12 Dr. Seiler noted that keratometry values decreased substantially, and the symmetry index improved significantly within 10 months following treatment.
The complication rate was extremely low. The most common complications were corneal haze, delayed epithelial healing and small corneal scars.12 Additionally, with the use of corticosteroids, all cases of corneal haze resolved within two to three weeks.
Also, a study of 44 eyes at the
More Research Required
Despite its early success, there is much to learn about collagen cross-linking for keratoconus patients. We are not certain if the procedure is as effective for patients in an advanced stage of keratoconus, nor are we sure if the procedure works as effectively on other types of ecstatic disease, such as PMD or post-LASIK ectasia. Additionally, while the procedure may halt disease progression, there are other important factors to address. For instance, you must consider if the patient may still require contact lenses, intracorneal ring implants or photorefractive keratectomy to correct residual refractive error following collagen cross-linking.
Collagen cross-linking is a potential treatment for patients who have progressive ectatic diseases, such as keratoconus. As with any new technology, additional research will continue to improve the final productwhich ultimately translates into improved care for your patients.
1. Menter JM, Patta AM, Sayre RM, et al. Effect of UV irradiation on type I collagen fibril formation in neutral collagen solutions. Photodermatol Photoimmunol Photomed 2001 Jun;17(3):114-20.
2. Laksshmi AV. Riboflavin metabolismrelevance to human nutrition. Indian J Med Res 1998 Nov;108:182-90.
3. Dalle Carbonare M, Pathak MA. Skin photosensitizing agents and the role of reactive oxygen species in photoaging. J Photochem and Photobiol B 1992 Jun 30;14(1-2):105-24.
4. Mackiewicz Z, Maatta M, Stenman M, et al. Collagenolytic proteinases in keratoconus. Cornea 2006 Jun;25(5):603-10
5. Zhou L, Sawaguchi S, Twining SS, et al. Expression of degradative enzymes and protease inhibitors in corneas with keratoconus. Invest Ophthalmol Vis Sci 1998 Jun;39(7):1117-24.
6. Collier SA. Is the corneal degradation in keratoconus caused by matrix-mealloproteinases? Clin Experiment Ophthalmol 2001 Dec;29(6):340-4.
7. Spoerl E, Wollensak G, Seiler T. Increased resistance of crosslinked cornea against enzymatic digestion. Curr Eye Res 2004 Jul;29(1):35-40.
8. Wollensak G, Wilsch M, Spoerl E, Seiler T. Collagen fiber diameter in the rabbit cornea after collagen crosslinking by riboflavin/UVA. Cornea 2004 Jul;23(5):503-7.
9. Wollensak G. Crosslinking treatment of progressive keratoconus: new hope. Curr Opin Ophthalmol 2006 Aug;17(4):356-60.
10. Menucci R, Mazzotta C, Rossi F, et al. Riboflavin and ultraviolet A collagen crosslinking: in vivo thermographic analysis of the corneal surface. J Refract Surg 2007 Jun;33(6):1005-8.
11. Wollensak G, Spoerl E, Reber F, Seiler T. Keratocyte cytotoxicity of riboflavin/UVA-treatment in vitro. Eye 2004 Jul;18(7):718-22.
12. Seiler T. Crosslinking of the cornea. Congress of the European Society of Cataract and Refractive Surgery.
13. Caporossi A, Baiocchi S, Mazzotta C, et al. Parasurgical therapy for keratoconus by riboflavin-ultraviolet type A rays induced cross-linking of corneal collagen: preliminary refractive results in an Italian study. J Cataract Refract Surg 2006 May;32(5):837-45.

