 A 37-year-old black man presented for a routine eye examination. He complained of difficulty while reading with his current near vision prescription.
A 37-year-old black man presented for a routine eye examination. He complained of difficulty while reading with his current near vision prescription.
His systemic history and previous ocular history were noncontributory. He denied using any medications. He does both carpentry and general construction for a living.
Diagnostic Data
His best-corrected visual acuity was 20/20 O.U. at distance and near. External examination was normal, with no evidence of afferent pupillary defect.
Intraocular pressure measured 19mm Hg O.U. The dilated fundus findings were normal O.U. Refraction suggested a benefit from a slight increase in add. The pertinent anterior segment findings O.S. are illustrated in the photograph.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? Whats the likely prognosis?
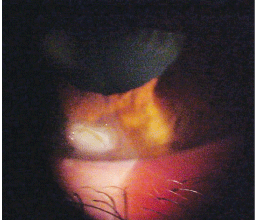
The left eye of our 37-year-old patient. What do you notice?
Discussion
The diagnosis is superficial corneal laceration with significant subepithelial infiltration (a mechanical etiology is presumed).
Additional testing included corneal sensitivity to determine if desensitization had occurred (a possible clue to how much time has passed since injury); Seidel testing; and close inspection of the iris, anterior chamber contents and lens tissue to establish the area of the injury and rule out the presence of full thickness penetration.
Corneal abrasion and superficial corneal laceration are two of the most common clinical entities that you will see in clinic. Patients usually present with some or all of these symptoms: acute pain, photophobia, pain upon extraocular muscle movement, lacrimation, blepharospasm, foreign body sensation and blurred vision.1-5 Be certain to document any history of contact lens wear or blunt trauma to the eye. In this case, despite the severity of the injury, our patient was completely unaware of the corneal laceration.
Primary treatment was administered over three days:
First, we anesthetized the cornea and trimmed the flap, which was completely necrotic and nonviable, with forceps and scissors. Then, we prescribed Acular (ketorolac tromethamine, Allergan) b.i.d and 600mg ibuprofen p.o. t.i.d. with food as needed. Also, we cyclopleged with atropine 1% to combat inflammation and any potential pain, and to stabilize the normal internal blood vasculature O.S. To prevent infection, we prescribed a topical fluoroquinolone antibiotic q2h during the day and tobramycin ointment h.s. We did not patch the patient, nor did we apply a bandage contact lens. We scheduled the patient to return in 24 hours.
The next day, we documented 60% resolution and noted that the patient was completely asymptomatic. So, we tapered the topical antibiotic to q.i.d., prescribed NaCl ointment h.s. and continued all other therapies. Again, we scheduled the patient to return in 24 hours.
On the third day of treatment, we noted almost complete resolution of the abrasion. Also, the residual inflammation was aggressively attacked by the addition of topical Lotemax (loteprednol etabonate, Bausch & Lomb) q.i.d. We discontinued the Acular, but continued all other therapies.
Three days later, our patients laceration was virtually 100% resolved, and his inflammation was approximately 80% resolved. Scarring remained, however. We discontinued the topical antibiotic drops and ointments, tapered the topical steroid, and instructed the patient to continue using the topical hypertonic ointment until the tube was empty. The next follow-up appointment was set at one week.
Within two weeks of treatment initiation, both the abrasion secondary to the laceration and inflammation were 100% resolved O.S. The patient was free of pain and symptoms. He was discharged with instructions to wear safety glasses on the job.
Additional Discussion
The cornea has five distinct layers: the corneal epithelium, Bowmans membrane, the stroma, Descemets membrane and the endothelium. There are two categories of corneal abrasion: superficial (which does not involve Bowmans membrane) and deep (which penetrates Bowmans membrane, but does not rupture Descemets membrane).
Cobalt blue light inspection, with the instillation of sodium fluorescein dye, will illuminate the damaged segment. When compared to the rest of the cornea, the wound will appear as a bright green area.3,5
The cornea has remarkable healing properties. Within 24 to 48 hours, the epithelium adjacent to any insult expands in size to fill in the defect.5 Epithelial lesions often heal quickly and completely without scarring. However, lesions that extend below Bowmans membrane pose an increased risk of permanent scarring.5
Treatment for corneal abrasion begins with patient history. Record the time, place and activity being performed when the injury occurred for both medical and legal purposes. Document visual acuity before initiating any procedures or drops. If the blepharospasm prevents acuity measurement, administer one drop of topical anesthetic. Measure visual acuity immediately thereafter.
During the eye examination, evert the eyelids and scrutinize the fornicies to rule out the presence of foreign material. Instill fluorescein dye (without anesthetic) to identify the corneal defects. Use the Seidel test to uncover full thickness injuries. Inspect the abrasion for size, shape, location and depth. Also, observe and document the anterior chamber. A dilated examination should be completed to rule out posterior effects from the trauma.
Begin medical treatment with adequate cycloplegia, which is often determined on a case-by-case basis. Use atropine 1% for severe cases and tropicamide 1% for mild cases. Also, prescribe topical antibiotics, such as Polytrim (polymyxin B and trimethoprim, Allergan), gentamicin or Tobrex (tobramicin, Alcon). Bed rest, inactivity and over-the-counter analgesics can be used to treat acute pain. In cases of severe pain, use topical nonsteroidal anti-inflammatory drugs (NSAIDs) q.i.d. or a thin, low water content bandage contact lens.1-6 Pressure patching is no longer considered a standard of care.1,2,4-6 Reevaluate patients every 24 hours until the abrasion is reepithelialized.1-5
Prescribe a hypertonic solution or ointment to promote healing, prevent recurrent erosion and reduce corneal edema after reepithelialization has occurred.5 In cases where excess epithelium impairs regrowth, use a cotton-tipped applicator saturated with anesthetic to debride loose tissue.5
If significant iritis is present or if subepitheial infiltration occurs during the reparative process, prescribe a topical steroid, such as Alrex or Lotomax (lotoprednol, B&L), FML (fluorometholone, Allergan), FML Forte (fluorometholone 0.25%, Allergan), Flarex (fluorometholone acetate, Alcon), Vexol (rimexolone, Alcon), Pred Mild (prednisolone, Allergan) or Pred Forte (prednisolone acetate, Allergan) q2h-q.i.d. Worsening subepithelial infiltration may be a sign of infection or impending ulceration. These lesions can be vision threatening and warrant immediate treatment with fluoroquinolone antibiotic drops q2h-q.i.d., depending upon the severity and size of the lesion.3
Lacerations may require suturing and appropriate referral. Cover any penetrating wound with a Fox Eye Shield (Bausch & Lomb Storz) or paper cup, and immediately refer the patient for surgical evaluation. In such cases, do not administer drops or exert any external pressure on the globe.
1. Donnenfeld ED, Selkin BA, Perry HD, et al. Controlled evaluation of a bandage contact lens and a topical nonsteroidal anti-inflammatory drug in treating traumatic corneal abrasions. Ophthalmology 1995 Jun;102(6):979-84.

