 A 28-year-old white male presented with complaints of acute vision alteration. He reported that “something just wasn’t right” in his left eye, and that there appeared to be a blurry spot in his peripheral vision. His ocular history was unremarkable for prior disease, surgery or trauma. He reported being very healthy, eating well and remaining physically fit. In fact, he mentioned that he first noticed these symptoms two days earlier, after returning home from the gym.
A 28-year-old white male presented with complaints of acute vision alteration. He reported that “something just wasn’t right” in his left eye, and that there appeared to be a blurry spot in his peripheral vision. His ocular history was unremarkable for prior disease, surgery or trauma. He reported being very healthy, eating well and remaining physically fit. In fact, he mentioned that he first noticed these symptoms two days earlier, after returning home from the gym.
Best-corrected visual acuity measured 20/20 O.D. and O.S. His pupils were equally round and reactive, and his motilities were normal. Upon confrontation fields and Amsler grid testing, the patient consistently displayed a large temporal scotoma in the left eye. Dilation revealed a well-circumscribed pre-retinal hemorrhage located nasally to the left optic nerve (figure 1). His history, clinical appearance and lack of associated retinal findings, such as exudates, cotton-wool spots or retinal tears, suggested a diagnosis of Valsalva retinopathy. So, how should we manage this patient?
The Valsalva Maneuver
The term “Valsalva maneuver” is well known in medicine. It is defined as “expiratory effort against a closed glottis, which increases pressure within the thoracic cavity and thereby impedes venous return of blood to the heart.”1 Valsalva maneuvers can be attained through a variety of circumstances, such as vigorous coughing, sneezing, vomiting, straining through constipation, trying to lift a heavy object, or any such effort that involves straining and holding one’s breath.
In our patient, his trip to the gym entailed running on the treadmill and lifting weights––both of which could induce a Valsalva event.
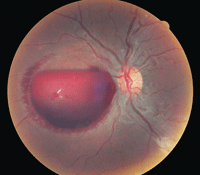
1. Appearance of our patient’s left fundus is indicative of Valsalva retinopathy.
In a clinical setting, the Valsalva maneuver might be employed to arrest episodes of supraventricular tachycardia, or diagnostically to help identify certain cardiac abnormalities.2,3 Complications may be seen when the maneuver is performed either too forcefully or for too long. This is a consequence of the exaggerated physiological changes that occur––particularly elevation of intravascular, intrathoracic (pulmonary) and intra-abdominal pressure and associated vascular reflexes.4 Specific systemic complications that have been associated with random or deliberate Valsalva events include syncope, alveolar rupture, inner- or middle-ear damage, migraine headache, cerebral hemorrhage and infarct, and even priapism.4-8
Ocular complications typically result from the rupture of small blood vessels in various tissues. Most commonly, this is seen as a non-traumatic subconjunctival hemorrhage. Valsalva retinopathy is another distinct and well-documented ocular manifestation of this phenomenon. All of these complications may be seen with increased frequency in patients who use systemic blood thinners (i.e., warfarin).9
The Clinical Appearance
The ophthalmoscopic picture of Valsalva retinopathy can be quite striking (figures 2 and 3). Often, the hemorrhage is fairly large, extending across several disc diameters. It is well demarcated and typically round in appearance. Most commonly, the presentation is unilateral, but bilateral cases have been documented.10
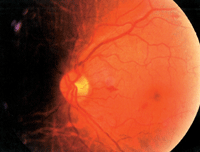
2. This patient exhibited small, superficial hemorrhages following a Valsalva maneuver. Photo: Andrew S. Gurwood.
The pre-retinal blood typically is bright red––in stark contrast to deeper retinal hemorrhages encountered in diabetic retinopathy or neovascular membranes associated with macular degeneration––and obscures underlying retinal and choroidal detail. In our experience, most cases seem to involve the macula, explaining why patients often present with decreased acuity.
Fortunately, our patient’s hemorrhage was situated in the nasal retina and therefore did not directly interfere with his acuity.
Management Strategies
Management of Valsalva retinopathy begins with a proper diagnosis. The patient history typically is the deciding factor in this regard. However, in cases with confounding elements, associated systemic disease or trauma, you must first rule out such conditions as proliferative diabetic retinopathy, hypertensive retinopathy, Purtscher’s retinopathy, Terson’s syndrome, retinal vein occlusion, retinal macroaneurysm and hemorrhagic vitreous detachment.11
Once a diagnosis is confirmed, the management approach for Valsalva retinopathy generally is conservative. Advise patients to avoid anticoagulant medications and strenuous activities that could potentially induce a re-bleed. Additionally, instruct them to sleep in a seated or elevated position to promote blood settling, which could potentially improve visual acuity in cases that involve the macula. If appropriate,
antiemetics or stool softeners may be employed.12
The typical recovery time for Valsalva retinopathy is six weeks to six months, although larger hemorrhages may take longer to reabsorb.13 In more severe or protracted cases, there is always concern that prolonged retinal exposure to hemoglobin and iron may induce cellular toxicity, leading to irreversible visual impairment. In these instances, surgical intervention via Nd:YAG laser is most appropriate. Several case series have been published that describe the utility of laser hyaloidotomy (e.g., puncture of the posterior hyaloid face) to allow drainage of preretinal hemorrhages into the vitreous cavity, thereby expediting resolution.11,13-16
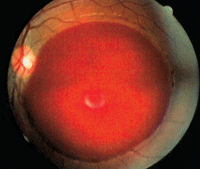
3. Another patient developed a massive preretinal hemorrhage secondary to a Valsalva maneuver. Photo: Andrew S. Gurwood.
Because our patient’s macula was not involved and his vision was only mildly impaired, we didn’t initiate therapeutic intervention. We advised the patient to restrict his physical activity for several weeks and avoid use of any blood-thinning agents. We also suggested a comprehensive health examination (which revealed no hematological or serological abnormalities).
“How soon will this annoying spot in my vision go away, Doc?” our patient asked. “Well… don’t hold your breath!” we responded. Fortunately, the hemorrhage, and his vision, resolved fully over the next four months.
1. The American Heritage Medical Dictionary. Boston: Houghton Mifflin Harcourt Publishing Company. 2008:569.
2. Smith G. Management of supraventricular tachycardia using the Valsalva manoeuvre: a historical review and summary of published evidence. Eur J Emerg Med. 2011 Dec 18. [Epub ahead of print]
3. Rolandi M, Remmelink M, Nolte F, et al. Effect of the Valsalva maneuver on cardiac-coronary interaction assessed by wave intensity analysis. Conf Proc IEEE Eng Med Biol Soc. 2010;2010:3776-9.
4. Taylor D. The valsalva manoeuvre: A critical review. J South Pacific Underwater Med Soc. 1996 Mar;26(1):8-13.
5. McGeeney BE. Valsalva-induced cluster headache. J Headache Pain. 2006 Dec;7(6):416-8. Epub 2006 Dec 10.
6. Carlson AP, Pappu S, Keep MF, Turner P. Large cerebellar hemorrhage during trumpet playing: importance of blood pressure elevation during the valsalva maneuver: case report. Neurosurgery. 2008 Jun;62(6):E1377; discussion E1377.
7. Uber-Zak LD, Venkatesh YS. Neurologic complications of sit-ups associated with the Valsalva maneuver: 2 case reports. Arch Phys Med Rehabil. 2002 Feb;83(2):278-82.
8. Chen WL, Tsai WC, Tsao YT. Valsalva maneuver-induced priapism: a hidden culprit. J Sex Med. 2009 Apr;6(4):1181-4.
9. Biyik I, Mercan I, Ergene O, Oto O. Ocular bleeding related to warfarin anticoagulation in patients with mechanical heart valve and atrial fibrillation. J Int Med Res. 2007 Jan-Feb;35(1):143-9.
10. Kim DK, Lee WJ, Cho MS, Kim JS. A case of atypical valsalva retinopathy after strenuous exercise. J Korean Ophthalmol Soc. 2005 May;46(5):915-20.
11. Puthalath S, Chirayath A, Shermila MV, et al. Frequency-doubled Nd:YAG laser treatment for premacular hemorrhage. Ophthalmic Surg Lasers Imaging. 2003 Jul-Aug;34(4):284-90.
12. Chapman-Davies A, Lazarevic A. Valsalva maculopathy. Clin Exp Optom. 2002 Jan;85(1):42-5.
13. Khan MT, Saeed MU, Shehzad MS, Qazi ZA. Nd:YAG laser treatment for Valsalva premacular hemorrhages: 6 month follow up: alternative management options for preretinal premacular hemorrhages in Valsalva retinopathy. Int Ophthalmol. 2008 Oct;28(5):325-7.
14. Durukan AH, Kerimoglu H, Erdurman C, et al. Long-term results of Nd:YAG laser treatment for premacular subhyaloid haemorrhage owing to Valsalva retinopathy. Eye (Lond). 2008 Feb;22(2):214-8. Epub 2006 Sep 1.
15. Mumcuoglu T, Durukan AH, Erdurman C, et al. Outcomes of Nd:YAG laser treatment for Valsalva retinopathy due to intense military exercise. Ophthalmic Surg Lasers Imaging. 2009 Jan-Feb;40(1):19-24.
16. Kirwan RP, Cahill MT. Nd:YAG laser hyaloidotomy for valsalva pre-macular haemorrhage. Ir J Med Sci. 2011 Sep;180(3):749-52. Epub 2009 Jun 3.

