The optometrically comanaged LASIK patient will have only limited contact with the surgeon; therefore, the responsibility for pre- and post-surgical management and potential complications falls mainly on your shoulders. You are the manager of the team, both clinically and in terms of medicolegal liability.
Here, Ill present a broad overview of pre- and postoperative drug therapy, including some tips on how to prevent the three most common LASIK complications: inflammation, infection and dry eye.
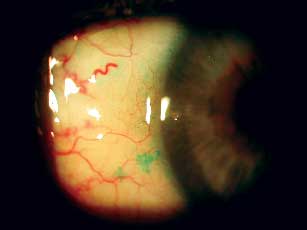
Lissamine green staining shows dry eye preoperatively in this patient. Any patient with even a hint of dry eye needs to be stabilized before surgery.
Education
Avoiding postoperative complications starts preoperatively with an emphasis on proper patient education. The aim at this stage is to present the positive and negative aspects to the patient. I like to tell them a story of a LASIK patient who came down with a cold one day after surgery. He started to take several OTC remedies and stayed in bed for the better part of a week, mostly sleeping. When he awoke, his eyes were very dry (induced by the OTC medications), and his flap became partially lifted at the inferior edge. He had followed his postoperative medication instructions, but the excess dryness and sleeping created the problem. His vision fluctuated from 20/20 to 20/30 and was distorted. The flap had to be re-floated, and a bandage contact lens had to be placed on the eye to allow the flap to properly settle.
As I tell the story, I tell my patients that this was not a catastrophe but an inconvenience that simply delayed an optimal outcome. Above all, this story illustrates the importance of complying with post-op meds. It also illustrates the value of the educational process. The patient in the story was informed that flap complication was a possibility, so he was not completely surprised when it occurred.
Day of Surgery
Before surgery, patients have the option to take Valium (diazepam, Roche) to counteract anxiety and fidgeting. But, I instruct them not to take this or any similar anti-anxiety drugs prior to arriving for surgery. These drugs can dry the surface of the eye if taken too early preoperatively, and they may over-sedate the patient. I ask that the patient refrain from ingesting food or drink high in carbohydrates, sugar or caffeine on the day of the surgery, as they will interfere with the Valium.
The anesthetic used during the surgery will probably be tetracaine hydrochloride. The effect of the drug lasts 15 to 30 minutes, but I tell patients they may continue to feel the effect of the drug for up to three hours. After that, they will feel an awareness of their eyes, possibly an itching and/or gritty sensation, but they should not experience severe pain.
Severe pain is usually a sign that something has gone wrong, and the patient should return to the office or call me as soon as possible. Many patients nonetheless ask about painkillers. We do not encourage nor do we prescribe any kind of narcotic-based medications for postoperative LASIK. It simply is not necessary. If the patient insists on a painkiller, I suggest OTC Tylenol (acetaminophen, McNeil) or Advil (ibuprofen, Wyeth) b.i.d. to q.i.d.
When surgery is complete, patients are given a take-home packet of important medications. These include:
A topical corticosteroid. Most patients can get by with a fluorometholone such as FML (Allergan), Flarex (Alcon) or eFlone (Novartis). These agents are designed to treat mild to moderate surface inflammation with minimal ocular absorption. I only prescribe maximum- efficacy steroids such as Pred Forte (prednisolone acetate, Allergan) if the patient develops a serious inflammatory condition, such as diffuse lamellar keratitis (DLK).
An antibiotic. Many physicians pre-treat with antibiotics, but I think this might err on the side of overkill. Ive been very satisfied with the postoperative performance of the fourth-generation fluoroquinolones Vigamox (moxifloxacin, Alcon) and Zymar (gatifloxacin, Allergan). Also, we know that most cases of bacterial keratitis are caused by Gram-positive organisms, and fourth-generation fluoroquinolones specifically target these pathogens.
However, do not disregard the effectiveness of the third-generation fluoroquinolonessuch as Ocuflox (ofloxacin, Allergan), Ciloxan (ciprofloxacin, Alcon) or Quixin (levofloxacin, Santen)which are still extremely effective. Because opinions vary so widely, you should discuss the choice of antibiotic with your surgeon. One school of thought views fourth-generation fluoroquinolones as overkill, while others will never go back to third-generation drugs. Still, some surgeons may suggest using a steroid- antibiotic combination drug such as TobraDex (dexamethasone/tobramycin, Alcon).
The onset of acute infection and subsequent symptoms most often occurs within 24 to 72 hours of surgery. Suspect infection in a post-op red eye that is not caused by a hemorrhage (see How to Handle Acute Infection, page 56).
Artificial tears. I prefer a single-ampule, non-preserved solution such as Refresh Endura (Allergan), Refresh Plus (Allergan) or GenTeal (Novartis Ophthalmic). Other preparationsantioxidant drops such as Viva-Drops (Vision Pharmaceuticals) or electrolyte-balanced drops, such as Bion Tears (Alcon Labs) or TheraTears (Advanced Vision Research)are also good choices. If the patient has dry eye or suspected dry eye, you might need to choose drops with more clinical impact (as discussed on the next page).
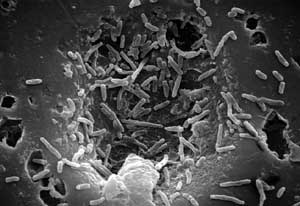
Scanning electron micrograph of Mycobacterium chelonae, one type of infection that may occur post-LASIK. The onset of acute infection and subsequent symptoms most often occurs within 24 to 72 hours of surgery.
Patient Management
Each take-home medication should be dosed at q.i.d., leaving about five minutes between administering each medication.
However, if I can get the patient to agree to it, I prefer dosing one medication every waking hour of the day, starting with the FML and ending with the artificial tear. In other words, patients dose the FML at 9 a.m., the antibiotic at 10 a.m., etc. This not only ensures the medicine reaches the ocular surface, but also enhances lubrication because each drop acts as a lubricant. I tell my patients that as the mantra of a successful retail business is location, location, location, so the mantra of successful refractive surgery is lubrication, lubrication, lubrication. (However, if the patient is non-compliant on this more aggressive schedule, I recommend the original q.i.d. schedule.)
We highly encourage the patient to refrigerate the drops. Refrigeration adds viscosity to the drops to achieve a longer ocular surface contact time, provides a higher level of comfort upon instillation and the cold has an anti-inflammatory, vasoconstrictive effect.
We also maintain the use of lubricants q.i.d. for 30 days postoperatively in conjunction with punctal occlusion.
I try to be present during surgery, and if not, I always call the patient that evening. Your phone call says that you are the manager and will resume control of the care in cooperation with the surgeon. Make these calls before 6:30 p.m., because if there is a problem, you will not want to be seeing patients at midnight. In the same vein, schedule one-day post-op exams as early in the day as possible. In the rare event of a complication that cannot be handled by the comanaging O.D., you will want to avoid finding the surgeon at 4 p.m. when he or she is getting ready to end the work day.
How to Handle Acute Post-LASIK Infection
In cases of acute infection, we always evaluate the anterior segmentinitially without stain, and then after instilling sodium fluoresceinand view the ocular surface with cobalt and a Wratten filter. The Wratten filter will help you to differentiate epithelial anomalies and intra-flap concerns.
In many cases, red eyes observed one-day postoperatively are due to mechanical chafing of the epithelium. They are easily treated by incorporating FML (fluorometholone, Allergan) ointment rather than drops. If the condition appears to be infiltrative, then an increase of steroid potency may be required (i.e., prednisolone), complemented with an increased frequency of antibiosis (approximately every two to three hours) and more frequent follow-up at 24-hour intervals until resolution.
If the red eye persists after 48 hours without resolution, consider an infiltrative or keratopathy response to be a surgical concern. If ulcerative in nature (i.e., Pseudomonas, Streptococcus, Mycobacterium, etc.), corneal melting from proteases can quickly ensue. In this case, the surgeon may want to re-float the flap, cleanse the stromal interface and instill antibiosis, possibly fortified.K.D.
Dry Eye
All refractive surgery patients should be screened for keratoconjunctivitis sicca. This should be done in the usual fashion, including tear break-up time, Schirmer testing (with and without anesthetic) and staining. Sequential staining is also valuable if you detect subtle conjunctival changes.
Borderline dry eyes are best diagnosed by a unilateral punctal plug trial if the etiology is tear volume deficiency. If you suspect mucous-membrane causes, try unilateral lubricant therapy using Systane (Alcon), Refresh Endura (Allergan), and/or electrolyte/oil-based supplements to help in the diagnosis. Any patient with even a hint of dry eye needs to be stabilized before surgery.
I tend to classify dry eye into two groups: red eyes, in which variable tear spreading with symptoms implies inflamed ocular surfaces; and white eyes, in which decreased tear volume production and symptoms imply inflamed lacrimal glands. The difference in presentation will define the specific therapy.
Red dry eye. I usually start red dry eye patients on Lotemax (loteprednol 0.5%, Bausch & Lomb) four times a day for two to four weeks, then reduce the drug to Alrex (loteprednol 0.2%, Bausch & Lomb) four times a day, and finally reduce that to maintenance once or twice a day. After surgery, long-term maintenance will include converting the patient to antioxidant or electrolyte/oil-based lubricantseither twice a day or four times a dayand an ointment at bedtime.
If the dry eye is severe, I start with Lotemax and incorporate a fluorometholone ointment at bedtime for about two weeks, then re-evaluate the patient. If tear volume remains poor after resolution of injection and discomfort, I initiate Restasis (cyclosporine, Allergan). During this process, the patient should continue using antioxidant- or electrolyte/oil-based drops.
White dry eye. These patients should start their preoperative therapy with Restasis q12h and should continue use for at least 30 days. Sixty days of therapy is preferable, although some patients need up to 90 days and sometimes even as long as six months to stabilize. If the condition is resistant, supplement the Restasis with Lotemax four times a day. Once stabilized, place the patient on Alrex q.i.d. for about a week before surgery.
Punctal plugs are an option for all dry eye patients pre- and postoperatively. In our practice, we insert punctal plugs in the E2/E4 (lower puncta) of all postoperative patients. I acknowledge that this is an aggressive approach, but it has worked well in our hands. Our philosophy is, let your own tears do their jobdefense and healing.
If the patient has dry eye prior to surgery, then well occlude the lower puncta only after the proper medical intervention. In these cases, we will use either a medium-term collagen (60-90 days dissolution rate) or a removable silicone (Freeman style) plug. In general, a short-term (5- to 10-day) plug is sufficient. However, we tend to use the medium term for extra lubrication coverage beyond the 30-day period.
In all cases, I encourage the use of omega-3 and omega-6 fatty acids, fish oils, seed oils and supplements, such as HydroEyes (Science-based Labs), Hydrate Essential (Cynacon) or TheraTears. These oils have a natural anti-inflammatory capability and help add lubrication to the mucous membranes. As a bonus, they are excellent for staving off arthritic and cardiovascular disorders.
Also, realize that there may be overlap between dry eye patients and ocular allergy patients. The symptoms are similar, and both conditions may cause the patient to become contact lens intolerant.
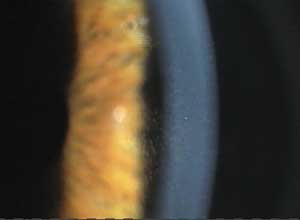
Diffuse lamellar keratitis first appears in the peripheral flap.
Courtesy: James D. Colgain, O.D.
Like dry eye, allergic conjunctivitis must be stabilized before surgery. My preference drug for accomplishing this is Patanol (olopatadine, Alcon), which can be used right up until the day of surgery and beyond without producing an ocular drying effect. Other options include Acular LS (ketorolac, Allergan), Livostin (levocabastine, Novartis) and other anti-allergy medications. Every individual will have a different response to the medicinal effectiveness.
Advise the patient to avoid almost all OTC allergy medications preoperatively, especially H1 antagonists, decongestants and vasoconstrictive agents, because they cause ocular dryness and possibly re-bound hemorrhage.
Blepharitis
Active blepharitis needs to be treated well before surgery takes place. Regular lid scrubs and an antibiotic ointment such as bacitracin or erythromycin are usually all that is needed. If not, the next step up is the combination drug TobraDex. I also recommend a shampoo containing selenium sulfide in case the blepharitis is seborrheic. Last resorts are systemic drugs such as doxycycline or tetracycline.
These patients should be checked for rosacea, which must be treated by a dermatologist prior to surgery.
DLK
Diffuse lamellar keratitis (DLK), also known as the sands of the Sahara, is a rare, non-infectious, diffuse inflammation seen in the first week after surgery. The patient will complain of discomfort, mild to moderate pain, foreign-body sensation, tearing, photophobia or a reduction in vision. Their eyes will be white, and the diffuse presentation will be limited to the flap interface.
Researchers are unsure of what causes this condition. But, they speculate it may be an allergic or a toxic inflammatory reaction, caused by some unknown factor during the surgery, possibly an iatrogenic reaction to latex of the surgeons gloves or lubricants of the microkeratome.
The first step is to rule out other interface opacities, including microbial keratitis, epithelial cells in the interface and non-microbial interface opacities, such as powder from the surgeons gloves or sponge fibers. Prescribe prednisolone acetate 1% one drop every one to two hours for 24 hours, then reduce to one drop every two hours for 48 hours.
If the condition does not resolve within a short period (48 to 72 hours), then you must refer the patient back to the operating surgeon, who will likely re-float the flap, and cleanse the interface.
When patients understand and are made an active part of the process, they are more than willing to follow our advice and the vital therapies of pre- and postoperative care that optimize their visual outcomes.
Dr. Daniels is an adjunct assistant clinical professor (Center for International Studies) and a National Eye Institute clinical investigator (CLEK Study) at the Pennsylvania College of Optometry, where he is also the former Director of Contact Lens Research. He maintains a private practices in Hopewell and Lambertville, N.J.

