Q: I recently had a Parkinson’s patient taking Symmetrel (amantadine hydrochloride, Endo Pharmaceuticals) present with bilateral corneal edema. A local corneal specialist suggested that we stop the medication, and the corneal edema disappeared over a few weeks. What is the mechanism for this reaction and is it always reversible?
A: Amantadine is an organic compound originally used as an antiviral for influenza A, but today it’s used to treat Parkinson’s disease because it reduces extrapyramidal symptoms and akathisia.1 Amantadine has been linked to several central nervous system side effects related to its dopaminergic, adrenergic and anti-cholinergic properties. Ocular side effects include vision loss, mydriasis, oculogyric crises, punctate subepithelial opacities and superficial punctate keratitis.2,3 The first case of a corneal edema associated with the use of amantadine was published in 1990.4
J. James Thimons, O.D., of Fairfield, Conn., explains that while the mechanism of action of the corneal edema is still unknown, the result is the loss of the endothelial cell count, which is dose- and duration-related.
Research to pinpoint the exact cause of the toxicity is ongoing. In 2007, a Veterans Health Administration survey showed a high level of correlation between the use of amantadine and clinical findings of corneal edemas.5 Subsequent studies have documented case reports of endothelial damage associated with amantadine.6,7 A 2010 study found that patients taking amantadine had lower endothelial cell counts and lower hexagonality of endothelial cells. In addition, the investigators found that longer duration of amantadine therapy and higher cumulative doses were associated with lower endothelial cell counts.8
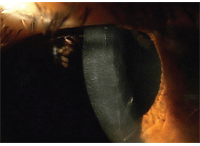
Amantadine therapy has been associated with decreased endothelial cell counts. Notice the obvious striae in this corneal edema patient.
“While the exact mechanism is unknown, the current theories revolve around the role the drug has in dopamine activation in the brain,” says Dr. Thimons. “I believe that there may be a relationship to the fact that the endothelium is neuronectodermal in origin and may have an enhanced receptiveness to the drug through that mechanism.”
Once a link between the drug and the corneal edema has been established, Dr. Thimons says, the correct course of action is to immediately remove the drug from the system.
However, the response is not always consistent nor is it always successful. The longer the drug has been in the system, the less likely it is that the response will be successful, he says.
Dr. Thimons diagnosed a similar case in a postoperative patient who was initially thought to be developing Fuchs’ dystrophy. Although the patient’s eye resolved nicely when Dr. Thimons identified the link to amantadine and the drug was removed from the patient’s system, he cautions that patients who do not see immediate relief will likely need penetrating keratoplasty or Descemet’s stripping endothelial keratoplasty (DSEK).
“It is reasonable, from several of the studies, to assume that once the effect has been identified, the risk of progression is a concern,” he said.
Be sure to first consult the prescribing physician, usually the neurologist, about discontinuing or suspending the drug.
1. Physician’s Desk Reference. Amantadine. Thompson Healthcare, Montvale, N.J.; 2003:1213-5.
2. Fraunfelder FT, Meyer SM. Amantadine and corneal deposits. Am J Ophthalmol. 1990 Jul;110(1):96-7.
3. Fraunfelder FT, Fraunfelder FW. Drug-Induced Ocular Side Effects. Butterworth-Heinemann, Boston; 2001:421-2.
4. Blanchard DL. Amantadine caused corneal edema. Cornea. 1990 Apr;9(2):181.
5. French DD, Margo CE. Postmarketing surveillance of corneal edema, Fuchs dystrophy, and amantadine use in the Veterans Health Administration. Cornea. 2007 Oct;26(9):1087-9.
6. Chang KC, Kim MK, Wee WR, Lee JH. Corneal endothelial dysfunction associated with amantadine toxicity. Cornea. 2008 Dec;27(10):1182-5.
7. Pond A, Lee MS, Hardten DR, et al. Toxic corneal oedema associated with amantadine use. Br J Ophthalmol. 2009 Mar;93(3):281.
8. Chang KC, Jeong JH, Kim MK, et al. The effect of amantadine on corneal endothelium in subjects with Parkinson’s disease. Ophthalmology. 2010 Jun;117(6):1214-9.

