History
A 32-year-old black male presented for a follow-up eye examination after an emergency room visit.
His chief complaint was a red, swollen left eye, without pain, which he had for the past two days.
He said he had splashed an automotive cleaning solution in the eye. He explained the ER had given him a course of I.V. antibiotics when he presented there about 30 hours before.
His systemic history was noncontributory.
Diagnostic Data
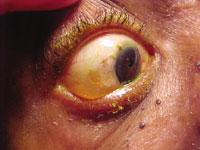
The patient"s right eye upon presentation.
His best-corrected acuity was 20/25 O.D. and 20/50 O.S. at distance and near. External examination findings were positive for periorbital edema and limited abduction O.S. There was no evidence of afferent pupillary defect.
The pertinent anterior segment findings are illustrated in the photograph.
Goldmann intraocular pressures measured 14mm Hg O.D. and 24mm Hg O.S. Dilated fundoscopy was within normal limits in both eyes.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests?
What is your diagnosis? How would you manage this patient? What is the likely prognosis
Diagnosis
Additional testing may include checking the cornea and conjunctiva for staining, checking for symblepharon formation, and ruling out iritis. Additional procedures may include swabbing and lavaging the lids to remove debris.
The diagnosis in this case is contact dermatitis, presumably secondary to the chemical splash. The patient was treated O.S. with atropine 1% for cycloplegia, diphenhydramine 50mgs. p.o. b.i.d. for the medications antihistamine effects, polysporin ointment for prophylaxis of infection and copious artificial tears and frequent cold compresses for palliative purposes.
Two days later, the patient returned for follow up, and his symptoms were much improved. Visual acuity O.S. improved to 20/30. At this point, the left eye demonstrated a 95% return of ocular motility, grade 1 periorbital edema with normal eyelid position, noticeable reduction in palpebral and bulbar conjunctival edema, and markedly reduced corneal epitheliopathy. The intraocular pressures at this point measured 15mm Hg O.U.
The current medical regimen was continued. A topical steroid medication (prednisolone acetate 1% q.i.d. O.S.) was added for its anti-inflammatory effects.
When the patient returned in five days, the condition was completely resolved. The patient was dismissed with instructions to call or return immediately if the condition returned. He was scheduled a follow-up appointment in six months. There were no complications.
Discussion
The thinness of the eyelid skin and conjunctiva makes them particularly delicate. The absence of firm adherences and the presence of loose subcutaneous tissues permits the accumulation of blood resulting from trauma and/or fluid resulting from an allergenic response.
Inflammation represents the bodys attempt to wall off areas of compromised tissue from healthy tissue, via the accumulation of fluid. The result is various levels of dolor (pain), rubor (redness), calor (heat), and tumor (swelling).1,2 Inflammation involves a complex sequence of events within tissues following initial exposure to an irritant.1,2 An inflammatory response is considered to be toxic when there is no previous record of exposure.1
Type IV hypersensitivity reactions, sometimes referred to as cell mediated hypersensitivity reactions, involve the T lymphocytes and lymphokines. Unlike the type I reaction, this reaction is classically delayed until sufficient antigens stimulate the chemical immune cascade. There is no direct IgE mediation to mast cell degranulation. That is why the reaction is not immediately observed.
Typically, patients with contact dermatitis present with a history of using or starting a new cosmetic, perfume, nail polish, clothing detergent, contact lens solution, ocular medication etc.1-23 The term medicamentosa keratoconjunctivitis is used to describe ocular reactions to ocular solutions and medications that produce a more substantial keratitis.24
The management of ocular contact dermatitis is primarily aimed at reducing symptomatology. 4,8,9,13,14,18-25 The easiest and most effective treatment for allergic conjunctivitis/contact dermatitis is elimination or avoidance of the offending allergen. The use of a cold compress, artificial tears, loose clothing ( if a covered area may be irritated by the vestments ) and ointments, cool, soothe and lubricate on an as-needed basis. Topical decongestants produce vasoconstriction, which reduces hyperemia, chemosis and other symptoms by retarding the release of the chemical mediators into the tissues from the blood stream. Topical antihistamines and oral antihistamines are also excellent therapies for acute signs and symptoms. Topical mast cell stabilizers should be used in seasonal or chronic cases involving the conjunctiva. The non-steroidal anti-inflammatory drugs may offer relief in moderate ocular cases with topical steroidal suspensions/solutions reserved for the most severe ocular presentations.
1. Silbert JA. The Role of Inflammation in Contact Lens Wear. In: Silbert JA. Anterior Segment Complications of Contact Lens Wear. New York: Churchill Livingston, 1994: 123-141.
2. Caffery BE, Josephson JE. Complications of Lens Care Solutions. In: Silbert JA. Anterior Segment Complications of Contact Lens Wear. New York: Churchill Livingston, 1994: 143-192.
3. Bloomfield SE. Clinical Allergy and Immunology of the External Eye. In: Duane TD, Jaeger EA. Clinical Ophthalmology. Philadelphia: Harper and Row, 1986; 4(2): 1-25.
4. Friedman NJ, Pineda R, Kaiser PK. Lids/Lashes/Lacrimal. In: Friedman NJ, Pineda R, Kaiser PK. The Massachusetts Eye and Ear Infirmary Illustrated Manual of Ophthalmology. Philadelphia: W.B. Saunders Co., 1998: 45-88.
5. Benjamini E, Sunshine G, Leskowitz S. Biology of the T-Cell lymphocyte. In: Benjamini E, Sunshine G, Leskowitz S. Immunology: A Short Course. New York: Wiley-Liss, 1996: 155-174.
6. Benjamini E, Sunshine G, Leskowitz S. Hypersensitivity Reaction: T-Cell Mediated Type IV-Delayed Hypersensitivity. In: Benjamini E, Sunshine G, Leskowitz S. Immunology: A Short Course. New York: Wiley-Liss, 1996: 299-314.
7. Groos EB. Complications of Contact Lenses. In: Duane TD, Tasman W, Jaeger EA, Eds. Clinical Ophthalmology, Rev. Ed. for 1997. Philadelphia: Lippincott-Raven, 1997; 4(27): 1-21.
8. Dawson CR, Sheppard JD. Follicular Conjunctivitis. In: Duane TD, Tasman W, Jaeger EA, Eds. Clinical Ophthalmology, Rev. Ed. for 1997. Philadelphia: Lippincott-Raven, 1997; 4(7): 1-26.
9. Fountain TR, Michon JJ. Cornea/External Disease: Toxic Conjunctivitis. In: Varma R. Essentials of Eye Care The Johns Hopkins Wilmer Handbook. Philadelphia: Lippincott-Raven, 1997: 168-169.
10. Kairys DJ, Smith MB. General Principles of Antibacterial Agents. In: Onofrey BE, Ed. Clinical Optometric Pharmacology and Therapeutics. Philadelphia: J.B. Lippincott Co., 1994:(22): 1-25.
11. Friel JP. Eczema. In: Friel JP, Ed. Dorlands Medical Dictionary, 26th ed. Philadelphia: W.B. Saunders Co., 1985: 420.
12. Jackson WB. Differentiating conjunctivitis of diverse origins. Surv Ophthalmol 1993 Jul-Aug;38 Suppl:91-104. Review.
13. Onofrey BE. Soothing the Symptoms of Ocular Allergy. Rev Optometry 1994; 131(9) Suppl.: 6a-9a.
14. Jennings B. Mechanisms, diagnosis, and management of common ocular allergies. J Am Optom Assoc. 1990 Jun;61(6 Suppl):S32-41. Review.
15. Onofrey BE. Principles of Immunology and The Immune Response. In: Onofrey BE, Ed. Clinical Optometric Pharmacology and Therapeutics. Philadelphia: J.B. Lippincott Co., 1994: (68): 1-13.
16. Kanski JJ. Disorders of The Conjunctiva. In: Kanski JJ. Clinical OphthalmologyA Systemic Approach, 3rd ed. Boston: Butterworth-Heinemann, 1995: 72-97.
17. Cullom RD, Chang B. Conjunctiva/Sclera /External Disease: Allergic Conjunctivitis. In: Cullom RD, Chang B. The Wills Eye Manual: Office and Emergency Room Diagnosis and Treatment of Eye Disease. Philadelphia: J.B. Lippincott Co., 1994: 112.
18. Pavan-Langston D, Dunkel EC. Anti-Allergy Agents and Ocular Decongestants. In: Pavan-Langston D, Dunkel EC. Handbook of Ocular Drug Therapy and Ocular Side Effects of Systemic Drugs. Boston: Little, Brown and Co., 1991: 7-21.
19. Burden G, Bryant SA. Conjunctivitis. In: Burden G, Bryant SA. Laboratory and Radiologic Tests for Primary Eye Care. Boston: Butterworth-Heinemann, 1997: 36-37.
20. Friel JP. Histamine. In: Friel JP, Ed. Dorlands Medical Dictionary 26th ed. Philadelphia: W.B. Saunders Co., 1985: 610.
21. Johnson KJ, Chensue SW, Kunkle SL, Ward PA. Immunopathology. In: Rubin E, Farber JL. Eds. Pathology 2nd ed. Philadelphia: Lippincott and Co., 1988: 97-141.
22. Friel JP. Tularemia. In: Friel JP, Ed. Dorlands Medical Dictionary, 26th ed. Philadelphia: W.B. Saunders Co., 1985: 1410.
23. Gurwood AS, Altenderfer DS. Contact dermatitis. Optometry 2001;72 (1): 36-44.
24. Aquavella JV, Shovlin JP, DePaolis MD. Protozoan and Fungal Keratitis in Contact Lens Wear. In: Silbert JA. Anterior Segment Complications of Contact Lens Wear. New York: Churchill Livingstone, 1994: 271-287.
25. Rhee DJ, Pyfer MF. Allergic Conjunctivitis. In: Rhee DJ, Pyfer MF. The Wills Eye Manual; Office and Emergency Room Diagnosis and Treatment of Eye Disease, 3rd ed. Philadelphia: Lippincott Williams and Wilkins, 1999: 122-123.

