
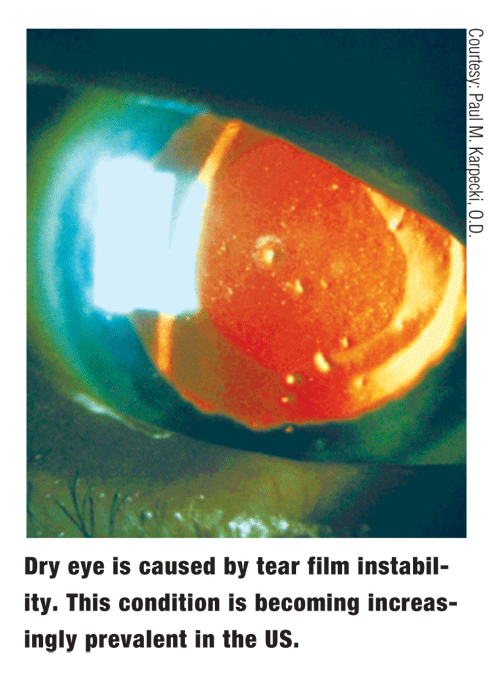
Dry eye is characterized by insufficiencies or instabilities in the tear film that can alter natural tear film break-up, resulting in unsatisfactory ocular surface protection. Depending on the population studied, estimates of the prevalence of dry eye range from 7.8% to 14.4%.1,2 Dry eye is often most prevalent in both female and elderly populations; however, ultimately, the condition can affect just about anyone.1,2
Dry eye is unique; it can present either as a component of a disease or as an acutely exacerbated condition. It seems to be an increasingly common complaint of patients who visit both optometry and ophthalmology practices.
This is likely attributable to the increasing prevalence of various aggravating factors: visual tasks, such as computer use, television watching or driving; environmental pollutants; contact lens wear; LASIK and other refractive surgeries; and the general aging of the baby boomer population.
Although subjective symptoms and surface keratitis are often cited as leading indicators of dry eye, further investigation of the problem must include a thorough examination of the tear film.
 Tear Film
Tear Film
In years past, optometrists believed the human tear film was comprised of three distinct entities: the aqueous, mucin and lipid layers.
Although these components are present in the tear film, the current view suggests that intermingling occurs among each of them.
At the ocular surface, membrane-bound mucins help adhere the bulk of the tear film to the ocular epithelium. They are components in a primarily mucin meshwork known as the glycocalyx.
Other mucins float freely in the large aqueous phase. Common ocular mucinsincluding Muc1, Muc4 and Muc5ACare generated by either goblet or conjunctival epithelial cells. The aqueous, which accounts for more than 90% of the total tear film volume, is the product of both the primary and accessory lacrimal glands.
Resting above the aqueous is the thin lipid layer, which is responsible for both retarding tear evaporation and lubricating the lid during blinking. Some lipids can also be found suspended in the aqueous.
Each component may be prone to reductions in quantity or quality, which can lead to destabilization of the entire tear film.
Each blink spreads the tear film and its components across the surface of the eye. Both tear drainage and evaporation slowly occur until the subsequent blink can replenish the tear film.

Tear Film Break-up Time
A patients tear film stability can be estimated by a tear film break-up time (TFBUT) measurement.
TFBUT is the interval between the last complete blink and the first dispersion of the tear film that exposes the ocular surface. Break-up usually occurs more rapidly in a dry eye patient with a destabilized or insufficient tear film than in a normal patient with a relatively healthy and well-balanced tear film.
Many factors may contribute to either decreases or increases in TFBUT. Both contact lens wear and lid margin disorders, such as meibomian gland dysfunction (MGD) and blepharitis, are often responsible for decreases in TFBUT. Contact lenses can affect the corneal surface or tear film structure, while lid margin changes can destabilize the lipid component of the tear film by stimulating insufficient or unhealthy meibum secretion.
Artificial tears are designed to extend TFBUT. In addition to improving ocular surface protection, increases in TFBUT may require less frequent dosing with a tear substitute.
Another important test, the ocular protection index (OPI) evaluation, compares TFBUT with inter-blink interval (IBI), the average number of seconds between blinks. To calculate IBI, a patients average blink rate must first be measured, either with an eye tracking camera and software or through manual observation and tally (the latter method is less accurate).
To generate an OPI score, divide TFBUT by IBI. A value greater than or equal to 1 implies that the ocular surface is protected, while a value less than 1 suggests that the ocular surface is not protected.6
Put another way, if the tear film breaks up before the eye can replenish it with a complete blink, there will be, on average, some period of time during which the ocular surface is exposedindicating insufficient protection. If a blink occurs before the tear film has a chance to disperse and expose the epithelium, however, the eye has sufficient ocular surface protection.
Tear Film Break-up Patterns
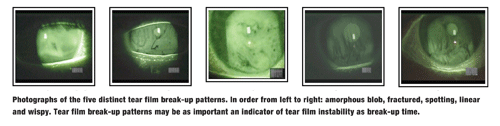
Recent research has shown that the pattern of tear film break-up may be as important as the actual break-up time. To date, five distinct tear film break-up patterns (TFBUPs) have been identified: linear, fractured, amorphous blob, spotting or wispy. These patterns were found to be generally reproducible in a given eye.
This discovery raises two questions: Is the composition of the tear film responsible for the break-up time and pattern? Or, does the nature of a particular patients dry eye determine how quickly the tear film breaks up and the way in which it breaks up?
Preliminary studies have investigated the distribution of TFBUPs in various patient populations, such as groups of both Ashkenazi and non-Ashkenazi Jews.7
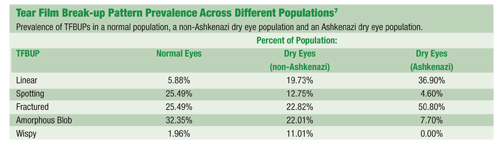
Where most (32.35%) non-dry eye patients demonstrated an amorphous blob break-up pattern, only 22.01% of a dry eye population showed such a pattern. But, while only 1.96% of the non-dry eye population showed a wispy break-up pattern, 11.01% of dry eye patients demonstrated wispy break-up.
Also, far fewer patients exhibited the spotting pattern in the dry eye population than the normal population. The prevalence of linear break-ups increased from 5.88% in non-dry eye patients to 19.73% in dry eye sufferers.
The etiology of the patients dry eye also seems to affect the distribution of patterns. For example, in a unique population of patients with Riley-Day syndrome, 50.8% of subjects demonstrated the fractured pattern, and only 7.7% exhibited an amorphous blob break-up.7
One could infer from the overwhelming prevalence of the fractured pattern that TFBUP may sometimes be attributable to the underlying etiology of a patients dry eye (in this case, Riley-Day syndrome). The progression of a patients dry eye, as determined by duration of diagnosis, seems linked with a different pattern distribution of TFBUPs.
In a study of 374 dry eye patients, 27.4% of patients with a dry eye diagnosis within zero to three years exhibited the linear pattern, while only 10.96% had a wispy break-up pattern. Conversely, in patients with a dry eye diagnosis within seven or more years, prevalence of the linear pattern dropped to 5.10%, while prevalence of the wispy pattern rose to 38.78%.
Additionally, the prevalence of the amorphous blob pattern dropped from 28.77% in zero- to three-year diagnosis subjects to 11.22% in subjects with diagnoses within seven years or more.8
Despite the varying distributions over different patient populations, the break-up patterns are acutely reproducible in individual eyes.
Various hypotheses have been formed about the reproducibility of TFBUPs. Could they be related to the location of keratitis on the ocular surface, or are they attributable to upper lid irregularities? The most convincing theories imply a link between quality or quantity of the various tear film components and specific patterns.
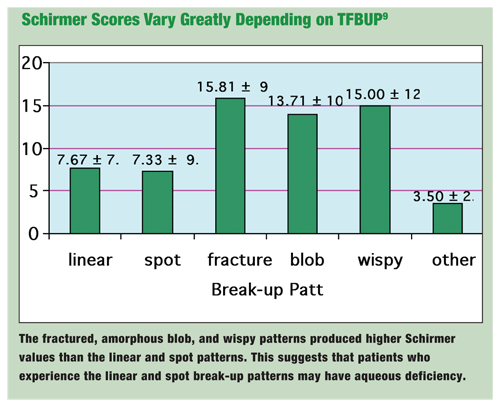
One study looked at break-up patterns in 104 dry eye patients, and found a statistical difference in the average Schirmer values between groups (See Schirmer Scores Vary Greatly Depending on TFBUP).9 Eyes with fractured, amorphous blob or wispy patterns all showed significantly higher Schirmer readings than eyes with the linear break-up pattern.
Since linear TFBUP eyes averaged a mere 7.67mm of tears, one could infer a possible connection between aqueous deficiency and the linear break-up pattern.
Another study of 45 dry eye patients found that meibomian expression yielded increases in the prevalence of the spotting and amorphous blob patterns, and the increased prevalence of these patterns was correlated with an increase in average TFBUT.10
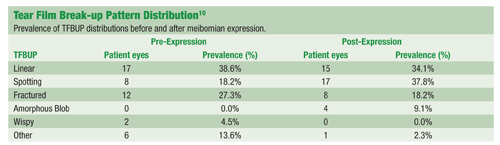
Not only did this suggest the association of these two patterns with better lipid protection, and therefore, more resistance to tear evaporation, but also it demonstrated the potential for acute modification of break-up patterns. There was a significant change in pattern distribution pre- and post-meibomian expression.
The stimulation of reflex tearing may also modify TFBUPs.11 From a clinical standpoint, it is just as important that an artificial tear can change a linear pattern, which is associated with aqueous deficiency and shorter TFBUT, to an amorphous blob pattern, which suggests the existence of a healthier tear film. This evidence implies that TFBUP may well have value as a clinical endpoint, for it is the ultimate goal of artificial tears to improve the integrity of the tear film.
Whether it is through TFBUT, TFBUP, or some other measurement, such as break-up surface area, tear film break-up should continue to provide clues to the nature of dry eye.
Diagnostic tests, such as TFBUT, OPI and TFBUP, will continue to allow both evaluation and comparison of potential dry eye treatments. When tear film instability can be understood and corrected, ocular surface protection can be reestablished. Then, patients suffering from dry eye will be offered something they are unaccustomed to: relief.
John Pietrantonio, O.D., is director of eye services at
1. Schaumberg DA, Sullivan DA, Buring JE, et al. Prevalence of dry eye syndrome among US women. Am J Ophthalmol 2003 Aug;136(2):318-26.
2. Moss SE, Klein R, Klein BE. Prevalence of and risk factors for dry eye syndrome. Arch Ophthalmol 2000 Sep;118(9):
1264-8.
3. Abelson MB, Ousler GW, Nally LA, et al. Alternative reference values for tear film break up time in normals and dry eye populations. In: Sullivan DA, Stern ME, Tsubota K, et al., editors. Lacrimal Gland, Tear Film, and Dry Eye Syndromes.
4. Ousler GW, Gomes PJ, Welch D, et al. Methodologies for the study of Ocular Surface Disease. Ocul Surf 2005 Jul;3(3):143-54.
5. Nally L, Ousler GW,
6. Ousler GW, Emory TB, Welch D, et al. Factors that influence the inter-blink interval (IBI) as measured by the ocular protection index (OPI). (Poster presentation) The Association of Research in Vision and Ophthalmology (ARVO), 2002.
7. Ousler GW, Wilcox-Hagberg K, Casavant JS, et al. Tear film break-up patterns in a population of dry eye patients of Ashkenazi Jewish descent. (Poster Presentation) The 24th Biennial Cornea Research Conference; Sep 30-Oct 1, 2005;
8. Casavant J, Ousler GW, Wilcox-Hagberg K, et al. A correlation between the signs and symptoms of dry eye and the duration of dry eye diagnosis.(Poster presentation) The Association of Research in Vision and Ophthalmology (ARVO), 2005.
9. Marsters E, Ousler GW, Schindelar MR, et al. A correlation between tear film break-up patterns (TFBUP) and the Schirmers test. (Poster presentation) The Association of Research in Vision and Ophthalmology (ARVO), 2006.
10. Schindelar MR, Ousler GW, Oberoi SL, et al. Perturbation of the meibomian glands and the effect on tear film stability and tear film break up patterns (TFBUP) in an Ashkenazi Jewish population. (Poster presentation) The Association of Research in Vision and Ophthalmology (ARVO), 2006.
11. Wilcox KA, Ousler GW, Schindelar MR, et al. Effect of reflex tearing on tear film break up time (TFBUT) and tear film break-up patterns (TFBUP) in a population of Ashkenazi Jewish patients. (Poster presentation) The Association of Research in Vision and Ophthalmology (ARVO), 2006.

