 History
History
A 47-year-old white male presented for an eye examination complaining of blur in his left eye lasting one months duration.
His systemic and ocular histories were noncontributory. He reported no previous trauma and denied having any allergies or taking medications of any kind.
Diagnostic Data
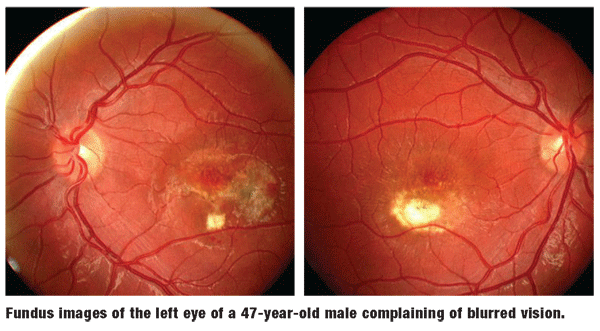
His best-corrected visual acuity was 20/25 O.D. and 20/100 O.S. at distance and near. External examination was normal, and there was no evidence of afferent pupillary defect. Anterior segment findings were normal. Intraocular pressure measured 18mm Hg O.U. The pertinent findings are illustrated in the photographs.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? What is the likely prognosis?
Discussion
The diagnosis in this case is Bests disease. We referred the patient to a retinologist for a fluorescein angiogram, which detected a treatable, subretinal neovascular membrane. The patient underwent laser photocoagulation, and visual acuity has remained stable.
Bests disease is a rare, dominantly inherited disease. It has been mapped to chromosome 11q13; however, the genetic abnormality responsible for this condition remains unknown.1
Bests disease can manifest itself in an individual at any age. In most cases, its onset occurs in childhood. Occasionally, however, Bests disease may initially appear during adulthood. Affected individuals show a range of yellow, bilateral, symmetric, foveal deposits that resemble a small egg yolk. These deposits are composed of fine, cuticular drusen (lipofuscin-like deposits in the retinal pigment epithelium, or RPE) in or near the fovea; although, recent theories have suggested the yellowish material may represent shed photoreceptor outer segments in association with subretinal fluid.2
These vitelliform lesions usually first appear during childhood, with a diameter ranging from 1mm to 5mm. Later in life, the lesions may break down resulting in chorioretinal scarring and atrophy. Late lesions are diagnosed by the constellation of signs, symptoms and history. Ironically, any decrease in vision is a result of atrophy and scarring of the paramacular and macular RPE and photoreceptors.
Choroidal neovascularization is rare, but can arise adjacent to old vitelliform scars. In fact, Bests disease is one of the causes of choroidal neovascularization in younger patients.3 In most instances, the visual acuity is unimpaired when the lesion remains off of the visual axis. If the lesion expands and disrupts macular integrity, vision will suffer. Visual disabilities usually occur during the scarring and neovascularization stages.1-3
Optical coherence tomography (OCT) has demonstrated that lipofuscin accumulates in the cystic spaces underneath the retinal pigment epithelium in the "pseudo-hypopyon stage." It also demonstrated that these lesions produce disruption of the photoreceptors in the "scrambled egg" stage. These new OCT findings could explain why visual acuity is preserved during the "pseudo-hypopyon stage," but is lost as the disease progresses through the "scrambled egg" stage of Best"s disease.4
Reduced electro-oculogram (EOG) distinguishes Bests disease from other forms of maculopathy. The full-field electroretinogram (ERG) is normal.
There is no treatment for this disease until chroidal neovascularization occurs. Then, it is treatable with focal laser photocoagulation, as in this patients case. Treatments of the future may include photodynamic therapy and intravitreal injection with anti-vascular-endothelial-growth-factor preparations. Patients should receive both education and consultation regarding this condition. When appropriate, they should be referred for low vision rehabilitation evaluation.
1. Parnell JR, Small KW. Macular Dystrophies. In: Yanoff M, Duker JS. Ophthalmology.
2. Spaide RF, Noble K, Morgan A, et al. Vitelliform macular dystrophy. Ophthalmology 2006 Aug;113(8):1392-400.
3. Miller DG, Singerman LJ. Vision loss in younger patients: a review of choroidal neovascularization. Optom Vis Sci 2006 May;83(5):316-25.
4. Vedantham V, Ramasamy K. Optical coherence tomography in Best"s disease: an observational case report. Am J Ophthalmol 2005 Feb;139(2):351-3.

