 A 49-year-old black male presents for initial examination and reports that he sustained blunt trauma to his left eye five years earlier, and subsequently lost all vision in that eye. Recently, though, he claims that his vision in the left eye spontaneously and intermittently becomes brighter and clearer. His ocular and medical history is otherwise unremarkable.
A 49-year-old black male presents for initial examination and reports that he sustained blunt trauma to his left eye five years earlier, and subsequently lost all vision in that eye. Recently, though, he claims that his vision in the left eye spontaneously and intermittently becomes brighter and clearer. His ocular and medical history is otherwise unremarkable.
Examination of the patient reveals leukocoria in the left eye; a dense, white cataract is seen through the pupil. Visual acuity in that eye is hand-motion only. Pupillary responses are normal in both eyes, and there is no afferent defect. But, while testing ocular motility, upon upgaze, the left pupil suddenly turns from white to black (figures 1 and 2)!
Inspection under the slit lamp shows that the lens is loose, moving within the posterior chamber as the patient looks about. What caused this unusual phenomenon, and what can be done about it?
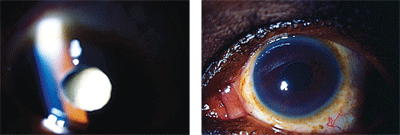
1, 2. Note the changing appearance of the pupil in downgaze (left) and upgaze (right).
Displaced and Distressed
In some cases, lens subluxation is associated with congenital systemic diseases, such as Marfan’s syndrome, homocystinuria, Weill-Marchesani syndrome, aniridia and Ehlers-Danlos syndrome.1-4 Acquired subluxation is typically the result of ocular trauma, and it is more common than lens displacement associated with the aforementioned systemic disorders.4 Blunt trauma causes mechanical stretching of the zonules as the eye is compressed in an anterior-posterior direction; the distention of the globe in the medial-lateral plane causes the zonular fibers to rupture.
In other instances, lens subluxation may occur spontaneously as a result of degenerative and inflammatory stimuli, such as those encountered in long-standing glaucoma, high myopia, hypermature cataract, retinal detachment, pseudoexfoliation syndrome and even anterior uveal tumors, in which zonular support is compromised and lost.5
The displacement of the crystalline lens can result in extreme hyperopic or myopic shifts, atypical astigmatism or acquired aphakia.
Occasionally—and this was the case with our patient—the vision fluctuates dramatically as the patient alternates between phakic and aphakic vision.6 Another common symptom is monocular diplopia, due to light entering the eye via two separate focal systems. While most clinicians immediately think of neurological problems when diplopia is mentioned, monocular diplopia is always attributed to some type of media issue, such as a cataract, corneal opacity or subluxated lens.
The main concern associated with subluxation of the lens is its apposition with the iris and mechanical obstruction of the pupil, because this can lead to pupillary block and secondary angle-closure glaucoma. Features of angle closure include an acute red eye presentation with a steamy cornea, accompanied by blurred vision, photophobia, pain, headache, nausea and vomiting.7,8
Rarely, the lens may completely dislocate into the anterior chamber. The concern with anterior lens displacement (in addition to pupillary block) is physical contact with the cornea; this induces disruption of the endothelial pump mechanism and leads to chronic, potentially irreversible corneal edema and decompensation.9
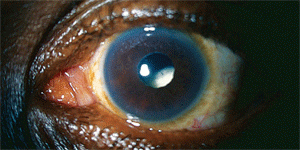
3. The subluxation/dislocation of the left lens is visible.
Diagnosing the Displacement
Subluxation is typically apparent with biomicroscopy (figure 3), but it may be difficult to detect if the pupil is small. Other signs to look for include phacodonesis, which refers to a shaking or jostling of the lens with eye movement. Likewise, patients with subluxation may display iridodonesis, as well as focal deepening of the angle. Pharmacologic dilation makes it easier to identify subluxation, but if there is any suspicion of complete lens dislocation in the posterior chamber, dilating the pupil is ill-advised.9
Managing patients with lens subluxation can be complicated; therefore, lens removal is really only indicated for patients with reduced vision or other visual or ocular symptoms. Coincidental subluxation, whether due to trauma or congenital disease, does not warrant intervention if the patient is asymptomatic. Monocular diplopia can often be overcome simply by using opaque cosmetic contact lenses.10 Alternatively, patients can be initiated on pilocarpine therapy—e.g., 0.5% or 1% q.i.d., or 4% Pilopine HS (pilocarpine hydrochloride, Alcon) at bedtime. Patients on a chronic regimen, however, should undergo concurrent prophylactic peripheral laser iridotomy because the risk associated with pupil block remains high and is increased by the use of pharmacologic miosis.11
Lens dislocation into the anterior chamber will ultimately lead to inflammation and, quite often, pupillary block. In such cases, try to reposition the lens into the posterior chamber. Recline the patient, dilate the pupil, and carefully manipulate the head and eye until the lens resituates. Miose the pupil with pilocarpine or dapiprazole immediately and obtain a surgical consult.
Extracting a Subluxated Lens
Surgical extraction of a subluxated lens can prove complex and difficult, so this course of management should only be considered if:12
• The patient suffers repeated or chronic dislocations of the lens, seriously impacting visual function.
• The crystalline lens is hypermature, and prone to phacolysis and inflammation.
• The lens dislocates into the anterior chamber and cannot be repositioned behind the iris.
Surgery for a completely dislocated lens necessitates intracapsular extraction via limbal (in the case of anterior lens displacement) or pars plana (in the case of posterior lens displacement) lensectomy/vitrectomy. Visual correction can be addressed with a sclerally-fixated posterior chamber implant, anterior chamber implant, contact lens or aphakic spectacles.13,14
Historically, moderately or severely subluxated lenses required the same type of therapy. But, the advent of capsular support devices—e.g., modified capsular tension rings (CTR), capsule anchors and other implantable devices—has allowed for better outcomes using modern techniques.15 A CTR is inserted into the capsular bag during surgery to help expand and stabilize the capsule following phacoemulsification. It helps redistribute support from intact zonules to the entire capsule. Modified CTRs are intended for cases of more severe zonular disruption; they are sutured to the scleral wall to fix the capsular bag in place and further maintain its integrity.15 Capsule anchors, a more recent development, are smaller PMMA implants that saddle the capsular bag and facilitate suture fixation to the scleral wall.16
While not a common occurrence, patients sometimes present with a “lens on the loose.” In such situations, don’t panic! Assess the severity of the condition, manage the optical complications, and obtain a surgical consultation if indicated. Modern technology permits these patients to enjoy restored ocular health and vision.
1. Sachdev N, Wakefield D, Coroneo MT. Lens dislocation in Marfan syndrome and UV-B light exposure. Arch Ophthalmol. 2003 Apr;121(4):585.
2. Cheng KH, Hung MC, Chen SJ, et al. Lenticular subluxation in a patient with homocystinuria undetected by neonatal screening. J Chin Med Assoc. 2007 Dec;70(12):562-4.
3. Chu BS. Weill-Marchesani syndrome and secondary glaucoma associated with ectopia lentis. Clin Exp Optom. 2006 Mar;89(2):95-9.
4. González-Castaño C, Castro J, Alvarez-Sánchez M. Subluxation of the lens: etiology and results of treatment. Arch Soc Esp Oftalmol. 2006 Aug;81(8):471-8.
5. Gutteridge IF. ‘My pupil has gone black!’ Subluxation of a total cataractous lens. Clin Exp Optom. 2008 Nov;91(6):557-60.
6. Loo AV, Lai JS, Tham CC, et al. Traumatic subluxation causing variable position of the crystalline lens. J Cataract Refract Surg. 2002 Jun;28(6):1077-9.
7. Dagi LR, Walton DS. Anterior axial lens subluxation, progressive myopia, and angle-closure glaucoma: recognition and treatment of atypical presentation of ectopia lentis. J AAPOS. 2006 Aug;10(4):345-50.
8. Inatani M, Tanihara H, Honjo M, et al. Secondary glaucoma associated with crystalline lens subluxation. J Cataract Refract Surg. 2000 Oct;26(10):1533-6.
9. Kawashima M, Kawakita T, Shimazaki J. Complete spontaneous crystalline lens dislocation into the anterior chamber with severe corneal endothelial cell loss. Cornea. 2007 May;26(4):487-9.
10. Crews J, Gordon A, Nowakowski R. Management of monocular polyopia using an artificial iris contact lens. J Am Optom Assoc. 1988 Feb;59(2):140-2.
11. Madill SA, Bain KE, Patton N, et al. Emergency use of pilocarpine and pupil block glaucoma in ectopia lentis. Eye (Lond). 2005 Jan;19(1):105-7.
12. Pelit A, Akova YA. Spontaneous posterior dislocation of both lenses in a patient with Marfan’s syndrome: 17 years without complications. Int Ophthalmol. 2005 Feb-Apr;26(1-2):49-51.
13. Choi DY, Kim JG, Song BJ. Surgical management of crystalline lens dislocation into the anterior chamber with corneal touch and secondary glaucoma. J Cataract Refract Surg. 2004 Mar;30(3):718-21.
14. Hoffman RS, Fine IH, Packer M. Primary anterior chamber intraocular lens for the treatment of severe crystalline lens subluxation. J Cataract Refract Surg. 2009 Oct;35(10):1821-5.
15. Blecher MH, Kirk MR. Surgical strategies for the management of zonular compromise. Curr Opin Ophthalmol. 2008 Jan;19(1):31-5.
16. Assia EI, Ton Y, Michaeli A. Capsule anchor to manage subluxated lenses: initial clinical experience. J Cataract Refract Surg. 2009 Aug;35(8):1372-9.

