
|

|
Topical medications have been a mainstay of post-op cataract care for many years. At the 2012 Optometric Council for Refractive Technology annual symposium, I presented data on a novel drug delivery model associated with cataract surgery to a room full of experts in the field of corneal and lenticular procedures.
In the lecture, I detailed five years of experience comanaging thousands of uneventful surgical cases in which topical antibiotics and anti-inflammatories were neither prescribed nor required. My practice was one of the first in the US to adopt “dropless cataract surgery” back in the late 2000s, and we’ve enjoyed tremendous success with the procedure ever since.
Here’s How It’s Done
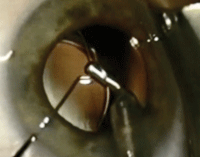
The transzonular technique (seen in the accompanying video) allows the surgeon to deliver formulated medication to the anterior vitreous at the conclusion of uncomplicated cataract surgery. By placing medication directly into the posterior chamber, drug clearance is delayed. This, in turn, provides sustained therapeutic protection against endophthalmitis and postoperative cystoid macular edema.
The medications used in dropless cataract surgery are formulated by a compounding pharmacy. Some surgeons prefer a blend of triamcinolone/moxifloxacin, while others use a triamcinolone/moxifloxacin/vancomycin combination.
Reasons to Drop the Drops
So, why all the buzz about going dropless? From anecdotal experience, this approach to cataract surgery has proven to be a safe, effective procedure for most patients. Here are a few significant advantages:
• Better postoperative drug compliance. When dealing with the typical cataract patient, we know that many individuals have to clear a number of potential physical, mental and situational hurdles to maintain good drop adherence. If patients do not use their medication in a timely fashion, the risk of infection increases. By placing the drug in the eye at the time of surgery, compliance-related concerns are effectively eliminated.
| |
|
For a video of transzonular drug delivery during cataract surgery,
click here. Photo and video courtesy of Kevinn Scripture, MD
|
• Convenience. In my experience, one of the biggest reasons patients defer cataract surgery is the dread of having to administer eye drops. For some, it’s the inconvenience of having to do it themselves. For others, it is a concern for friends or family members who likely would have to alter their schedules to assist with drop instillation.
• Less confusion. Despite multiple patient education sessions both before and after surgery, confusion over the postoperative drop regimen continues to be an issue for most practices. Staff members spend a significant amount of time fielding phone calls regarding proper administration technique and frequency. When eye drops are eliminated from the equation, so is the associated dosing confusion.
Postoperatively, dropless cataract patients are seen one day, one week and one month after the procedure. If significant inflammation is present at the postoperative visits, additional anti-inflammatory medications may be used. Although it is not a mainstream technique, optometrists should be aware of the procedure and understand why some surgeons are either actively performing or strongly considering dropless cataract surgery.
Dr. Mangan is a consultative optometrist at Bennett & Bloom Eye Centers in Louisville, Ky.

