A 77-year-old Hispanic female presented complaining of painless, bilateral vision loss that had persisted for the past year. Additionally, she reported that the vision in her right eye became dramatically worse two weeks ago. Her medical history was significant for hypertension, which was controlled with medications.

On examination, her visual acuity measured 3/200 O.D. and 20/50 O.S. Confrontation fields were full to careful finger counting O.U., and Amsler grid was significant for central metamorphopsia O.D.
The patient’s pupils were equally round and reactive, without afferent defect. Extraocular motility testing was normal. The anterior segment examination was unremarkable, except for 2+ nuclear sclerosis O.U. Her IOP measured 12mm Hg O.U.
On dilated fundus exam, we noted a posterior vitreous detachment O.U. Her optic nerves were normal O.U. The posterior poles and maculae can be seen in figures 1 and 2. Her peripheral retinae were normal O.U. We also obtained an optical coherence tomography scan of her right eye (figure 3).
Take the Retina Quiz
1. What do the changes seen temporal to the right macula likely represent?
a. Choroidal neovascular membrane (CNV).
b. Cystoid macular edema (CME).
c. Neurosensory retinal detachment.
d. Retinal pigment epithelial (RPE) detachment.
2. What does the OCT show?
a. Large RPE detachment with neurosensory retinal detachment.
b. Cystic spaces of fluid in the intraretinal layers.
c. Macular retinoschisis.
d. RPE tear.
3. What is the diagnosis for the patient’s right eye?
a. Exudative age-related macular degeneration.
b. Macular telangiectasia.
c. Idiopathic central serous choroidopathy (ICSC).
d. Harada’s syndrome.
4. How should this patient be managed?
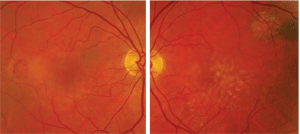
1, 2. The right and left eye of our patient (O.D. left, O.S. right). Note the fundus
changes seen in the right eye. How do you account for her vision being 3/200 O.D.?
a. Anti-VEGF therapy.
b. Observation.
c. AREDS-formulated multivitamins and home Amsler monitoring.
d. Photodynamic therapy.
5. What is the prognosis for visual recovery O.D.?
a. Good, with treatment.
b. Too early to tell.
c. Not very good, despite treatment.
d. Uncertain. Patient must first be referred to a retinal specialist.
Retina Quiz Answers: 1) a; 2) d; 3) a; 4) b; 5) c.
Discussion
The clinical appearance of this patient and the OCT scan confirmed the diagnosis of RPE tear in the setting of exudative age-related macular degeneration. There was an area of subretinal hemorrhage secondary to a CNV located temporal to the macula. CNV leakage subsequently resulted in an RPE detachment as well as an overlying serous detachment. The detachment became more bullous and taut, causing the RPE to
eventually tear. This occurred at the time when the patient noticed her sudden vision loss.
The RPE tear was difficult to discern on clinical exam; however, the OCT scan provided excellent anatomic detail and helped to confirm the diagnosis. The OCT showed the large pigment epithelial detachment (PED) with an obvious break and disruption of the RPE temporally. In addition, the overlying serous detachment can be seen temporal and nasal on the OCT.
RPE tears have a classic clinical presentation. Patients typically present with severe vision loss that is sudden in nature.1 These tears characteristically appear as an atrophic break of exposed choroid adjacent to an area of darkly-pigmented RPE. Fundoscopy correlates with fluorescein appearance of an area of hypofluorescence due to blockage from scrolled RPE that is located next to an area of hyperfluorescence, secondary to exposed choroid. Significant leakage, which is often expected with the loss of the outer blood-retinal barrier at the exposed choroid, typically is not seen on fluorescein angiography unless the entity occurs in the setting of a choroidal neovascular membrane (CNVM).1
Optical coherence tomography imaging is helpful in confirming the diagnosis, often illustrating focal disruption along with frank loss of the RPE. Scrolled or rolled edges of the RPE may appear as irregular, hyperreflective areas. In the setting of AMD, OCT may help distinguish between geographic atrophy and a chronic RPE tear.1
J. Donald M. Gass, M.D., described the pathogenesis of RPE tears in which new vessel growth through Bruch’s membrane combined with the formation of occult lesions and increased permeability of the vessels.2 Because the RPE remains attached to one side of this lesion and a pressure gradient is formed, the RPE detaches from the other side of the lesion. The force of the pressure causes a tear at the junction of the attached and detached tissue. Additional hypotheses have described the pathogenesis of RPE tears, including weakened RPE cells, hydrostatic pressure buildup from PEDs, CNVM contracture and vitreoretinal traction.2
The setting of a vascularized PED in exudative AMD is the most common setting for these tears.1 However, spontaneous RPE tears have been described in the clinical picture of central serous retinopathy, angioid streaks and trauma as well as secondary to various treatments for AMD.1
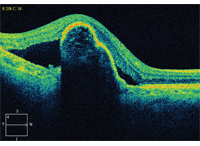
3. The OCT scan through the patient’s right macula. How would you interpret this image?
In connection with the increasing popularity of anti-VEGF therapy––particularly for exudative AMD––numerous reports have been published regarding the incidence (2% to 17%) of RPE tears following intravitreal injection.3 Consequently, additional studies have proposed certain risk factors for PEDs following anti-VEGF therapy, including larger RPE detachment size and occult CNVM.2
Interestingly, our patient had a prior diagnosis of CNV associated with AMD and received at least two injections of Avastin (bevacizumab, Genentech). She received the most recent injection approximately 10 weeks prior to the development of her RPE tear. She has not received a subsequent injection since developing the RPE tear. We will continue to monitor her closely, but, because of her widespread RPE loss, her visual prognosis is quite poor.
This case was written and submitted by Jennifer Sinclair, O.D., optometry resident at the Bascom Palmer Eye Institute in Miami.
1. Chang LK, Sarraf D. Tears of the retinal pigment epithelium: an old problem in a new era. Retina. 2007 Jun;27(5):523-34.
2. Gass DJ. Pathogenesis of tears of the retinal pigment epithelium. Br J Ophthalmol. 1984 Aug;68(8):513-9.
3. Yeh B, Ferruci S. Retinal pigment epithelial tears after bevacizumab injections. Optometry. 2011 Mar;82(3):152-7.

