Q. I have a patient with significant ocular cicatrical pemphigoid (OCP) who uses immunosuppressants, has excessive dry eye and is beginning to form symblepharon. Which contact lenses might provide comfort and improved vision for this patient?

A. Have the immunosupressants caused the OCP, or more specifically the inflammation process, to go into remission? If so, a non-ventilated gas permeable scleral lens may be the best option. It provides protection from the action of the diseased lids and lashes and creates a reservoir of fluid to bathe the corneal surface, says optometrist Janis Cotter of New England College of Optometry in Boston.
Perry Rosenthal, M.D., of the Boston Foundation for Sight in Chestnut Hill, Mass., agrees. Scleral lens wear does not affect the course of the disease, including the development of symblepharon, but it offers other advantages. The liquid bandage created by these devices can offer significant relief from the pain and photophobia that result from ocular surface dryness and the irritation associated with trichiasis and distichiasis, he says. Moreover, vision that is compromised by irregular astigmatism will be improved.
When inserted, the scleral lens should be filled with sterile saline to retain a precorneal fluid reservoir, provided that the scleral zone can be fit with adequate alignment. Corneal hydration is thus improved, even though the natural tears are abnormal or even virtually absent, says optometrist Ken Pullum of Moorfields Eye Hospital in London. A larger lens allows extension of the reservoir further beyond the limbus. On the other hand, the fitting process may be rendered more difficult if the scleral topography is too irregular or asymmetric, in which case an eye impression may be required prior to fitting.
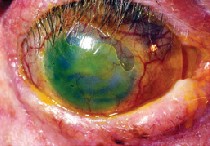
Scleral contact lens in situ in a case of advanced ocular cicatrical pemphigoid. Courtesy: Ken Pullum, O.D.
Keep in mind that the location of the symblepharon dictates the diameter of the scleral lens, Dr. Pullum says. In some cases, it may rule out a scleral lens completely.
If the symblepharon is located way out in the edge of the conjunctiva, fitting a regular-size scleral lens is no problem, Dr. Cotter adds. But as it gets closer and closer to the cornea, you have to make the lens smaller and smaller. And, if the symblepharon occurs between the lid and the cornea, you really wont be able to get a lens on there.
Q. What can I do if the patient is unable to wear any contact lenses? For example, can a surgeon cut the symblepharon so that I can fit a scleral lens?
A. Because OCP is a progressive disease, we are limited. Generally speaking, symblepharon should not be disturbed surgically, as the inflammatory effects of such a procedure can cause the process of the OCP to progress and extend the scarring, says Stephen E. Pascucci, M.D., of Scranton, Pa. This scarring can lead to further goblet cell loss and progression of dry eye and cicatrical changes.
Conjunctival grafting might seem a possible alternative when a non-ventilated gas permeable lens is contraindicated. However, because OCP is usually bilateral, useful conjunctival tissue cannot easily be obtained. So, an autograft is rarely possible, Dr. Pascucci says.
While mucous membrane grafting might seem to be another alternative, it is not applicable here. Traditionally, the fornix needs to be healthy, and this is not the case with OCP, Dr. Pascucci says.
Amniotic membrane grafting may offer some hope, however. This procedure provides useful tissue to reconstruct resected abnormal tissue, Dr. Pascucci says. Its advantages: Amniotic membrane is readily obtainable, easy to handle and ideal for grafting onto the eye.

