A 48-year-old Hispanic female presented with a chief complaint of blurred vision and distortion in her left eye that had persisted for the last four months. She assumed the condition would simply improve on its own, but instead, her symptoms gradually worsened. Her medical history was unremarkable. She was a smoker and had a positive family history for glaucoma.

On examination, her best-corrected visual acuity measured 20/20 O.D. and 20/70 O.S. Confrontation visual fields were full to careful finger counting O.U.
Her pupils were equally round and reactive, with no afferent defect. Amsler grid testing of the right eye was normal; however, the left eye showed mild central distortion. Extraocular motility testing was normal. The anterior segment examination of both eyes was unremarkable. Her intraocular pressure measured 14mm Hg O.U.
On dilated fundus exam, her vitreous was clear. The optic nerves appeared healthy, with a small cup and good rim coloration and perfusion O.U. The remainder of the fundus exam of her right eye was normal. However, we noted a subtle elevation of the macula in her left eye. The remainder of the fundus examination of her left eye revealed other pertinent findings.
In addition, we ordered an optical coherence tomography scan (figure 1), ultrasound (figure 2) and fluorescein angiogram.

1. Here is a 3D view through the left macula on Spectralis OCT (Heidelberg Engineering). What obvious changes can be seen?
The peripheral retina of the patient’s left eye was unremarkable, exhibiting no open holes, tears, breaks or detachments.
Take the Retina Quiz
1. Based on the OCT and ultrasound, at what level is the lesion primarily located?
a. Choroid.
b. Bruch’s membrane.
c. Retinal pigment epithelium (RPE).
d. Sensory retina.
2. What critical finding does the OCT reveal?
a. Elevated choroidal mass lesion.
b. RPE detachment with cystoid macular edema (CME).
c. Neurosensory detachment.
d. The OCT provides no useful diagnostic information.
3. What is the reflectivity of the lesion?
a. No significant reflectivity.
b. Low internal reflectivity.
c. Medium internal reflectivity.
d. High reflectivity.
4. What is the correct diagnosis?
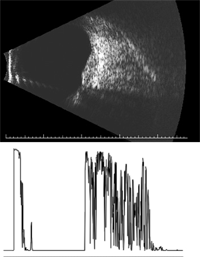
2. B-scan (top) and A-scan through our patient’s lesion. What is the most
significant finding?
a. Amelanotic nevus.
b. Choroidal melanoma.
c. Metastatic lesion.
d. Choroidal hemangioma.
5. How should this patient be managed?
a. Observation.
b. Intravitreal anti-VEGF injection.
c. Plaque radiotherapy.
d. Photodynamic therapy (PDT).
For answers, see below.
Discussion
On clinical examination, it was evident that our patient’s left eye had an elevation of the retina that involved the macula. However, it did not appear that the elevation was due to any type of fluid accumulation. Indeed, the elevation was solid and dome-shaped.
What’s more, upon reduced magnification on 90D slit lamp ophthalmoscopy, a more prominent, reddish hue involving the macula and posterior pole was seen. This was even more noticeable on binocular indirect ophthalmolscopy. In fact, there was a striking contrast between the reddish appearance of the lesion and the “normal” retina that surrounded it. This was very noticeable on the montage fundus photo, but was much less apparent with high magnification at the slit lamp. Although we had a strong suspicion as to what the lesion represented, we ordered an OCT and a standardized ultrasound to help confirm the diagnosis.
The OCT nicely detailed the dome-shaped elevation that we observed on clinical examination; however, what was most remarkable was that the lesion appeared to be at the level of the choroid, pushing up on the RPE and sensory retina. On one of the OCT sections through the fovea, we also noted a subtle neurosensory detachment.
Perhaps, the standardized ultrasound provided the most useful information in this case. As seen in figure 2, there was a dome-shaped elevation on the B-scan. The A-scan showed a lesion at the level of the choroid, with high internal reflectivity. This finding is illustrated by a high initial spike that corresponds to the retina, followed by a space, then another highly reflective spike that corresponds to the anterior surface of the lesion, and then a series of highly reflective spikes that represent the lesion’s high internal reflectivity.
Based on the clinical appearance and coloration of the lesion, we suspected that our patient had a choroidal hemangioma. This was confirmed by the high internal reflectivity on the A-scan.
A choroidal hemangioma is a benign, vascular tumor of the choroid that is chiefly composed of large, dilated, thin-walled vessels, with minimal stroma. These lesions blend almost imperceptibly with the surrounding choroidal tissue. They are usually round or oval, slightly elevated, and have a subtle orange-red coloration.1,2 Often, such tumors have indistinct borders and are more apparent on BIO, as was the case with our patient. They are usually located in the posterior pole, within the paramacular area. Some may be found adjacent to the optic nerve or on the nasal side of the disc.
Most patients are asymptomatic and, as a result, such lesions may be discovered as an incidental finding. Symptoms may develop if the lesion is located directly under the macula, or if the patient develops a neurosensory detachment that spreads from the edge of the lesion into the macular area––which is what occurred in our patient.
Choroidal hemangiomas can also be seen in patients with Sturge-Weber syndrome. In Sturge-Weber syndrome, patients typically present with angiomatous malformations of the face (nevus flammeus), uveal tract and brain.1,2 But our patient did not have Sturge-Weber syndrome, because she presented with an isolated choroidal hemangioma.
Usually, choroidal hemangiomas do not grow much once the patient reaches adulthood. Some minor tumor enlargement may occur later in life, but this is believed to occur secondary to varicosity and congestion of the large vascular channels. Over time, the hemangioma may cause a degenerative breakdown of the overlying RPE, resulting in cystic edema or a serous detachment of the sensory retina.
Fluorescein angiography shows a characteristic pattern of early hyperfluorescence that corresponds to the large vascular channels located within the tumor. Later in the angiogram, widespread fluorescence secondary to diffuse leakage of the dye from the surface of the tumor can be seen. Unfortunately, this similar staining pattern also can be seen in other similar-sized tumors.
Ultrasonography is the most helpful diagnostic examination in differentiating these tumors from more serious conditions, such as choroidal melanoma. A choroidal melanoma will show low to medium reflectivity, whereas a choroidal hemangioma will demonstrate high reflectivity.1
Ultimately, it’s the reddish-orange color of the lesion viewed on BIO that provides the index of suspicion for the correct diagnosis and helps differentiate it from other lightly colored or nonpigmented lesions.
Most patients with choroidal hemangiomas do not need to be treated unless they develop macular edema or a neurosensory detachment that involves the fovea. When this occurs, photocoagulation has been the traditional treatment of choice. But, newer, less invasive treatments, such as PDT and intravitreal anti-VEGF therapy, have also been effective treatment options.2,3
Our patient received an intravitreal injection of Avastin (bevacizumab, Genentech). We scheduled her to return for follow-up within the next few weeks.
Thanks to Jennifer Sinclair, O.D., optometric resident at the Bascom Palmer Eye Institute in Miami, for contributing this case.
Retina Quiz Answers: 1) a; 2) a; 3) d; 4) d; 5) b.
1. Gass JD. Stereoscopic Atlas of Macular Disease: Diagnosis and Treatment. 4th ed. St Louis: Mosby; 1997.
2. Anand R, Tasman WS. Nonrhegmatogenous Retinal Detachment. In: Wilkinson CP (ed.). Retina, vol. III: Surgical Retina. 4th ed. St. Louis: Mosby; 2006:2122-41.
3. Sagong M, Lee J, Chang W. Application of intravitreal bevacizumab for circumscribed choroidal hemangioma. Korean J Ophthalmol. 2009 Jun;23(2):127-31.

