Remember the days before the autorefractor, when optometrists had to project cartoons on a screen in order to achieve accommodative relaxation? How about the era when visual fields were performed on a tangent screen? And, does anyone remember prolonged ocular occlusion?
Review asked some of optometrys most respected veteran O.D.s to take a look back at the evolution of diagnostic testingwhat it was like yesterday and what it has evolved to today. Here are some of their memories.
 The Not-So-Good Old Days
The Not-So-Good Old Days
By Robert M. Cole III, O.D.,
Chief Clinical Editor
When I reflect on my early years of practice and reminisce with colleagues, I cant help but be impressed with the advances weve made in our modes and methods of practice. When I think about a typical comprehensive examination 25 or 30 years ago compared with today, it becomes almost comical at times. One thing is for sure: Its very easy to see how advances in technology have made our lives easier and greatly improved our examination techniques. The quality of information gathered, the capacity to compare it over time, and the speed at which this information is available to us seems nothing short of miraculous.
In the refractive portion of an eye examination, the instrument that has unquestionably enabled me to provide better accuracy, more speed and more confidence, has been the autorefractor. When I think back on examining an uncooperative child without the luxury of cycloplegia, I recall using devices such as remote-controlled animated mechanical stuffed animals or projected cartoon movies to achieve accommodative relaxation while trying to determine an objective refraction using retinoscopy. Today, I really appreciate my autorefractor! Of course the same can be said comparing manual to autokeratometry as well.
I remember doing visual field examinations in a dark room by placing little white pins in a felt wall to determine isopters of vision. The old tangent screen is a far cry from the threshold automated perimeter as we know it today. Just imagine trying to diagnose or treat a glaucoma patient without devices such as this and HRT, GDx, and stereo or digital photography.

The physical retinal examination has been greatly improved as well, with devices such as binocular indirect ophthalmoscopes, aspheric lenses, and even the Optos imager. These were either not available or were not as finely tuned as they are today.
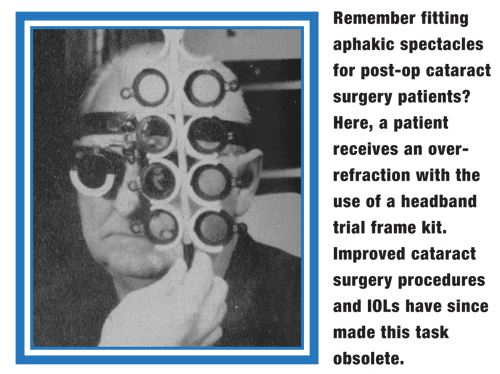
I remember when my cataract post-op visits used to be done in one day in the hospital, but would then linger for almost three months, slowly removing sutures from a 120 incision. This, of course, was followed by the fitting of aphakic glasses, or instructing an 80-year-old patient in the care and handling of a contact lens. Thank heaven for phacoemulsification and IOLs.
Fortunately, technology has not been limited to the exam room. Patient scheduling, recalls, insurance forms, billing and clinical records were either all typed or handwritten! Imagineno computers! There were no fax machines, cell phones, e-mail or electronic billing. Being on call meant hoping you could locate a phone if your beeper went off (assuming, of course, that you had a beeper).
Whats even more astounding is the seamless integration of all of these technologies and the ease and user-friendliness of their applications.
What is equally amazing for an old-timer like me who never learned to type: As I sit here with a cast on my left and dominant hand, I am able to produce this document entirely using voice-recognition software.
Gosh, I wonder whats next?
 What Was, What Is, and What Will Be
What Was, What Is, and What Will Be
By Pamela J. Miller, O.D., J.D.
It was 1973, and I had just graduated from the brand new campus of the Southern California College of Optometry (formerly Los Angeles College of Optometry).
There were no drug laws for optometrists, intraocular pressure testing was reserved for those patients over age 40, and Bausch & Lomb had just released the first soft contact lenses for low levels of simple myopia.
A well-equipped office had a slit lamp/biomicroscope, trial lenses and frame, color and stereo books, a tonometer, retinoscope, ophthalmoscope, keratometer/ophthalmometer, lensometer and a phoropter. Visual fields, when done at all, were usually done on a tangent screen. A few practitioners were even still performing trial frame refractions. 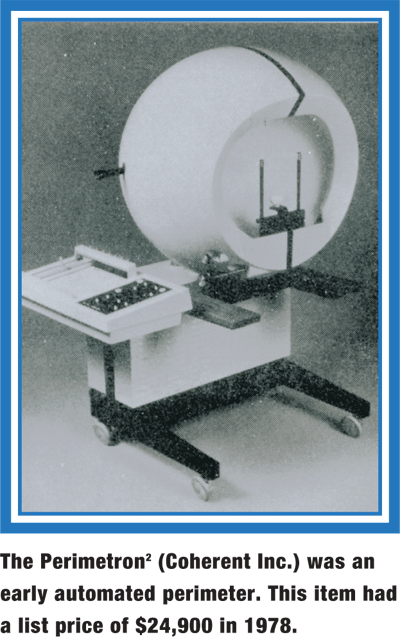 Most contact lenses were made of PMMA, and fluorescein was utilized for fit evaluation, either with a slit lamp and/or a
Most contact lenses were made of PMMA, and fluorescein was utilized for fit evaluation, either with a slit lamp and/or a
Few patients were covered by insurance; most were private pay and retained the concept of the family doctor. It was a time when optometry was changing, as was the entire health care system.
Over the next three decades, optometry gained the right to utilize and prescribe drugs, developed parity with medicine, became an active player in the health-care system, and increased its ranks of both female members and non-white practitioners. The field leveled between professional and commercial practitioners, and we became independent, strong, and respected as our education and scope of practice increased.
Todays doctor of optometry frequently comanages patients with other health-care providers, performs a variety of medical interventions, is an active provider of insurance covered services, and is a dynamic force helping lead the face of health and vision care.
Just as the practitioner has become more knowledgeable and increased his or her scope of practice, the basic optometric practice now includes a variety of computerized testing devices. Automation is routineincluding topographers, autorefractors, tonometers, pachymeters, computerized acuity charts, digital fundus photography, automated billing and coding programs, automated perimeters (that can print out or send the results to the computer), electronic health care records, pupillometers instead of the PD rulerand the list goes on.
The push is to do more and do it quicker, more efficiently and more effectively. As this occurs, more patients are covered by insurance, patient loyalty is diminished and is driven by the insurance carriers, and doctors receive less reimbursement for more work and greater patient testing. Staffing requirements have increased, and most practices are utilizing computers for billing, ordering, and authorization purposes, as well as scheduling, patient notification, and patient contact lens ordering. Some doctors have gone completely paperless for their patient records, and virtually all offices have a full time computer staff person. This is a far cry from when I started with one staff person who could do it all and not feel overly-burdened.
When I look at the scope of practice I enjoy today and the equipment I rely on daily to provide the best patient care possible, it is almost overwhelming. Annual equipment investments are the rule, not the exception. The learning curve for this new equipment continues to challenge, and my office of five years ago is only the skeleton for my office of today.

I fully expect to be practicing for another 25 or 30 years. I eagerly anticipate the improved diagnostic and therapeutic equipment. Within the next few years, I see my patients utilizing a touch screen to provide necessary information, making their appointments through the computer, being able to view themselves with a variety of frames or contact lens colors in free-space.
My exam equipment will become less actual equipment and more open-space testing devices. The phoropter and biomicroscope of my not-so-distant office will actually be a screen projected in front of the patient that I can control remotely. Fundus photography will be routine and enhanced with automated evaluations and comparison capabilities of common diseases like diabetes, glaucoma, macular degeneration, etc. Patient records will be easily transferred between practitioners.
The age of improved computerization and automation are rapidly becoming the norm. Consultation with other practitioners and specialists will be routine and in real-time, with the clinicians practicing in different parts of the country as well as the world. The time may even come when a great deal of vision care can be provided to patients in their own home, in a care facility, or in outer space!
The bottom line is and always has been this: Change or become obsolete. We optometrists have a tremendous resiliency and (no pun intended) vision. We have been aggressive and we can adapt to our changing environment with enthusiasm and eagerness.
I cant wait for tomorrow. How about you?
 Remember Prolonged Ocular Occlusion?
Remember Prolonged Ocular Occlusion?
By Irving Bennett, O.D.
Prolonged ocular occlusion? Ill bet that well over 90% of the readers of this little article never heard the expression, particularly if the readers are optometrists who graduated later than 1980. So, whats the big deal?
In December 1967, Raymond Roy, a well-respected optometrist from
Dr. Roy developed a technique to make the discovery of the condition easy for practitioners to use. He managed to attract numerous O.D. advocates. Periodic reports about patients who magically recovered from years of migraine headaches began to surface. The miracle cure was a simple pair of eyeglasses with an unusually high amount of vertical or horizontal prism, and in some cases, both.

Not too many years after Dr. Roy reported at the Academy meeting, the profession of optometry took a sharp turn toward medical optometry. The definitive diagnosis of ocular medical conditions became much more attractive than the use of prisms in ocular lenses. The art and science of correct ocular dysfunction took a hit, and to this day, it has not made a full recovery.
Optometrys journey over the last 50 years has been nothing less than remarkable. New privileges and new responsibilities have emerged. Unfortunately, some of the older tests and techniques, like the use of prolonged ocular occlusion, were sacrificed to make way for change.
It is this sacrifice that many senior optometrists, retired and not, bemoan.
 Perspectives on the Evolution of Diagnostic Technology
Perspectives on the Evolution of Diagnostic Technology
Linda Casser, O.D.
As is the case with every health care profession, optometry has witnessed and contributed to the development of an explosion of new diagnostic technology in the past 20 to 30 years. This has directly impacted optometric practice in three important ways:
First, doctors of optometry utilize and integrate new technologies into their practices.
Second, as primary eye-care providers, optometrists are knowledgeable about new technologies used to provide care for the patients whom they comanage with other providers.
Last, but not least, the evolution of technology has provided access to new resources and methods of communication.
In my perspective, the introduction of automated threshold visual field testing instruments in the early 1980s was the leading edge of this technological transformation. Doctors of optometry were central to the development of this instrument; they fully integrated the instrument into their practices in caring for their patients, and they have contributed to the literature describing the instruments use, outcomes and efficacy.
This trend has continued in other important areas, such as contact lens care. New contact lens materials have been developed and new diagnostic technology, such as corneal topography, has become integral to delivering care to contact lens patients.
Instruments used to provide the refractive component of comprehensive eye and vision care, such as the phoropter and lensometer, have become automated.
Diagnostic technology available for assessing and managing patients with glaucoma and vitreoretinal disease has increased dramatically, with the incorporation of pachymetry, confocal laser scanning ophthalmoscopy, and optical coherence tomography. Also dating from the early 1980s, diagnostic fundus lenses greatly expanded in availability and optical quality.
In the late 1970s and early 1980s, optometrists patients started undergoing phacoemulsification and intraocular lens implantation when they were comanaged for cataract extraction. This directly impacted the clinical practices of doctors of optometry, and they are expert in providing care for patients who have undergone these procedures.
Similarly, and due to their expertise in optics and anterior segment disease, optometrists counsel and comanage patients for refractive surgical procedures of all types, an area of clinical care that has evolved dramatically since the mid-1990s with regard to the technology available for patient assessment and management.
These are just a few examples of the far-reaching and substantive impact that diagnostic and related technology has had on optometric practice in recent decades. Of course, this trend will continue in ways that are predictable and many that currently are not.
While doctors of optometry have been, and will remain, effective adopters and developers of diagnostic technology, technology will serve to complement the art and science that they dedicate to their patient care responsibilities.

