 |
An important element of the review of systems (ROS) specific to the gastrointestinal system is to investigate for jaundice—a yellowish staining of the skin, conjunctiva/episclera/sclera (termed icterus), other mucous membranes and excretions.1
While not a disease itself, jaundice is a sign of a number of underlying conditions that cause the bile ducts, gallbladder, liver or pancreas to malfunction. The color is caused by subsequent hyperbilirubinemia, an excess amount of bilirubin in the blood. Jaundice is often reported in infants and newborns, as well as in children and adults with medical complications (Table 1).1,2
Jaundice is a clinical sign optometrists should be on the lookout for, as it is usually first noticeable in the eyes.1 However, its onset may be so gradual that even those in frequent contact with the affected person may not notice it.1 In addition to its ocular features for diagnostics, jaundice may result from conditions that have significant ocular complications, such as sarcoidosis, sickle cell disease and various infections.1
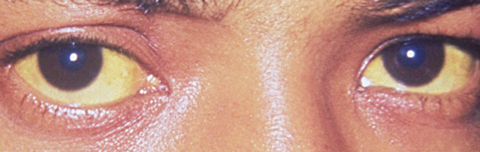 |
| Hepatitis A may manifest as jaundice of the conjunctiva and facial skin. Photo: CDC/Dr. Thomas F. Sellers |
How and Why
Bile is produced and released by the liver and stored in the gallbladder. Eventually delivered directly to the intestinal lumen, it helps with digestion by breaking down fats into fatty acids to be taken into the body by the digestive tract. The primary constituents in bile are cholesterol, acids (also called bile salts) and bilirubin. It also contains water, potassium, sodium, copper and other metals.3
Bilirubin is a yellow/brownish chemical in bile, formed by the breakdown of heme rings, usually from metabolized red blood cells. Bilirubin is normally excreted in bile, giving feces the normal yellow-brown coloration. As senescent hemoglobin-containing erythrocytes break down, the body builds new cells to replace them, and the liver processes the old red blood cells. If the liver cannot handle the blood cells as they break down, bilirubin builds up in the body and jaundice results. Jaundice is detected clinically once the serum bilirubin level rises above 2.5 mg/dL to 3mg/dL.1,3
The amount of bilirubin manufactured (0.5 to 2.0 grams per day) relates directly to the quantity of red blood cells destroyed. Bilirubin has no known function and can be toxic in the fetal brain. Bilirubin in the bloodstream is usually in an unconjugated (free) state. Once transported to the liver, it is attached to the protein albumin and becomes conjugated with glucuronic acid. Bilirubin is then concentrated to about 1,000 times the strength found in blood and transferred to the gallbladder, where it mixes with other bile components.1,3
Jaundice may result from an overproduction of bile or from an inability of the liver to remove bile pigments from the blood due to hepatic disease, regurgitation of bilirubin back into the bloodstream or obstruction of the bile ducts.1-3
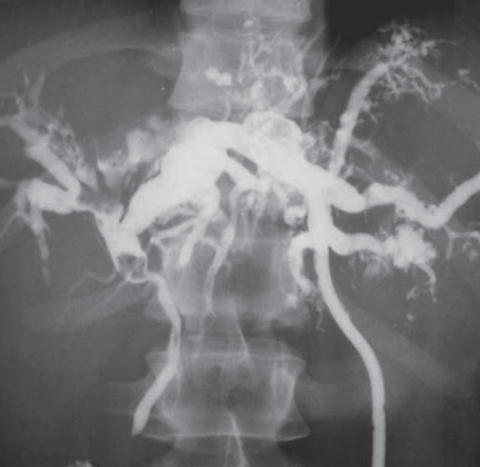 |
| Cholangiography shows dilated bile ducts with extensive abscesses and stones. |
Classification
Clinicians generally describe three types of jaundice, classified according to what is disrupting the normal removal of bilirubin from the body:1
Prehepatic (hemolytic) jaundice. Here, the disruption happens before bilirubin has been transported from the blood to the liver. It is caused by conditions such as sickle cell anemia and hemolytic anemia. Hemolysis is an accelerated breakdown of red blood cells, leading to an increase in bilirubin production.1
Intrahepatic (hepatocellular) jaundice. The disruption happens inside the liver and is caused by conditions such cirrhosis or other liver damage, including injury.1
Post-hepatic (obstructive) jaundice. With this form, the disruption prevents bile (and thus bilirubin) from draining out of the gallbladder and into the digestive system. This can be caused by conditions such as gallstones, biliary tract infection, pancreatitis or neoplastic disease.1
Jaundice in InfantsA healthy newborn may acquire jaundice because the liver has not fully matured.2 Unconjugated hyperbilirubinemia is a normal physiologic event that occurs in approximately 60% of normal full-term infants and in 80% of preterm infants.2,3 The bilirubin level normally increases after two to three days and peaks by five to seven days, reaching as high as 12mg/dL in normal full-term babies and up to 14mg/dL in normal premature infants by the end of the first week of life.2 Breast-fed babies may normally have an elevated bilirubin level until the end of the second week of life. In infants two weeks of age or older, however, the onset of jaundice within the first 24 hours of life, rate of rise of serum bilirubin levels greater than 5mg/dL in 24 hours, direct bilirubin level greater than 1mg/dL at any time, or the persistence or new onset of jaundice may no longer be physiologic.2,3 |
Gallstones are solid particles that form from bile cholesterol and bilirubin in the gallbladder. They are known as bile duct stones or choledocholithiasis when located in the bile duct. Certain bacteria can infect the gallbladder and change the conjugated bilirubin back to free bilirubin and acid. The calcium from the freed bilirubin can settle out as pigment stones, which may eventually block the common bile duct between the liver, gallbladder and small intestine. When blockage occurs, conjugated bilirubin is absorbed into the bloodstream and becomes clinically evident as jaundice and icterus.
Investigating the Cause
Organizing the differential diagnosis of jaundice by prehepatic, intrahepatic and post-hepatic helps make the workup straightforward. Lab work should begin with a urine test for bilirubin, which indicates that conjugated hyperbilirubinemia is present. If the complete blood count and initial tests for liver function and hepatitis are unrevealing, the workup typically proceeds to abdominal imaging by CT or ultrasonography.1,3 More invasive procedures such as cholangiography or liver biopsy may occasionally be necessary to arrive at a diagnosis.
Table 1. Common Causes of Jaundice by Age1,2 | |
| Age | Conditions |
| Neonates younger than 2 weeks | Neonatal jaundice (physiologic) |
| Neonates older than 2 weeks | Hepatitis, biliary atresia, choledochalcyst, obstructive congenital anomalies of the biliary tract, total parenteral nutrition, furosemide treatment, phototherapy, dehydration, infection, hemolytic anemia and short-gut syndrome |
| Infants and young children (two months to four years of age) | Cirrhosis, benign strictures and neoplastic disease |
| Children and adolescents (four to 18 years of age) | Sickle cell disease, bowel resection, hemolytic anemia and choledochal cyst |
| Adults | Viral infections (hepatitis A, B and C), chronic alcohol use, autoimmune disorders, drugs, pregnancy, parenteral nutrition, sarcoidosis, primary biliary cirrhosis, primary sclerosing cholangitis, gallstones, surgical strictures, infection (e.g., cytomegalovirus and Cryptosporidium infection in patients with acquired immunodeficiency syndrome), intrahepatic malignancy, cholangiocarcinoma, extrahepatic malignancy (pancreas, lymphoma) and pancreatitis |
Jaundice in Your Chair
One of the first things an optometrist should do during a patient encounter is to take a step back and observe the patient. Whether it is a shuffling gait as a result of advanced glaucomatous field loss, a head tilt indicating a high vertical phoria or changes in coloration such as flushing or jaundice, the optometrist must be keenly aware of these signs and the potential underlying causes.
A thorough review of systems and comprehensive history are key, as they may point to a specific cause, such as cirrhosis or pancreatitis. In addition to icterus, your ophthalmic workup may uncover such signs as uveitis or metastatic choroidal carcinoma. These ocular complications can guide your lab workup as you rule out various causes of jaundice. As always, the patient’s primary care physician should be promptly made aware of your findings.
Timely and appropriate testing, as well as comanagement with and referral to the appropriate subspecialist (e.g., pediatrics, gastroenterology, infectious disease) are typically required. Physicians do not treat jaundice; they treat the condition that causes this telltale sign.
1. Roche SP, Kobos R. Jaundice in the adult patient. Am Fam Physician. 2004;69(2):299-304. |

