 History
History
A 45-year-old white male presented with a chief complaint of worsening diplopia and general “eye discomfort.” While it was not officially documented in his ocular history, the patient explained that he underwent orbital decompression surgery twice to relieve congestion in his left eye secondary to thyroid-related, infiltrative disease of the muscles.
At this visit, he also wanted his spectacle prescription (which contained prism to alleviate double vision) checked and updated.
Additionally, his medical status was being followed closely by an endocrinologist, who determined that his thyroid function was within normal parameters. Nonetheless, the patient explained that his orbital disease seemed to be progressing, despite proper medical management.
Diagnostic Data
Best-corrected visual acuity through +2.25DS spectacles measured 20/40 O.D. and 20/50 O.S., which had decreased from 20/30 O.U. at his last visit. External examination uncovered limited ocular motilities throughout all directions of gaze, with full confrontational fields and no evidence of afferent pupillary defect O.U.
We were unable to significantly increase his visual acuity via refraction. Biomicroscopy revealed inferior sodium fluorescein dye uptake located inferiorly on the both the bulbar conjunctiva and cornea (O.S. > O.D.). The anterior chambers, irides and lenses were clear. His intraocular pressure measured 16mm Hg O.U.
Because the patient’s visual acuity was reduced, we performed a dilated fundus examination. The pertinent findings are illustrated in the photographs.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? What’s the likely prognosis?
Discussion
Given the patient’s history of systemic thyroid disease, additional testing included exophthalmometry; a measurement of the marginal reflex distance; and an evaluation of tear prism, quality and volume to determine ocular surface status.
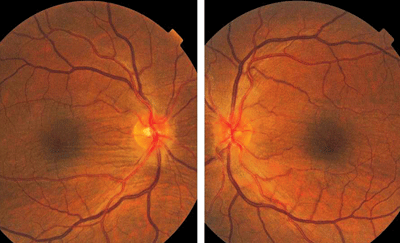
Fundus images (O.D. left, O.S. right) of our 45-year-old patient who presented with worsening diplopia and discomfort. His medical history was significant for thyroid disease. What is the likely diagnosis in this case?
The diagnosis in this case is choroidal folds secondary to orbital complications of systemic thyroid disease.
Graves’ disease, Graves’ orbitopathy, thyroid eye disease and thyroid ophthalmopathy (TO) are all synonymous terms for an autoimmune disorder that is characterized by multiple systemic manifestations.1-12 The associated ocular condition that is characteristically found in patients with TO may exist in the absence of clinical or biochemical evidence of thyroid dysfunction.2
When both the systemic and ocular manifestations coexist, the conditions may follow completely different clinical courses.2-4 The hallmark sign of TO is bilateral, non-pulsatile proptosis.1,2 Other important findings include impaired ocular motility, variable diplopia, eye lid retraction, and variably impaired visual acuity or sight loss secondary to corneal exposure-related keratopathy and/or compressive optic neuropathy.5
The etiology of TO is multifactorial and secondary to newly discovered heritable abnormalities that interfere with immune regulation.1,13 Not all of the mechanisms responsible for the systemic and/or ocular manifestations are understood.2,13 Research regarding the clinical manifestations of TO traditionally point to a combination of increased orbital fat and extraocular muscle volume within the orbital space.1,2,6-9,13 Other important causes of ocular complications include toxic nodular hyperthyroidism (which is caused by the presence of one or more autonomously functioning thyroid nodules) and thyroiditis. In these cases, antithyroid drugs, such as carbimazole or methimazole, are the initial treatment of choice.12
Additionally, radioiodine has been increasingly used as a first-line therapy, and is considered the preferred treatment choice for individuals with relapsed Graves’ hyperthyroidism.12
Finally, complete throidectomy is an option in selected cases.12
Orbital decompression is established procedure for the management of exophthalmos or other cases that exhibit optic neuropathy.14 Numerous procedures that remove orbital bony wall and/or fatty tissue have been reported in the literature.14 Finally, orbital radiation is a controversial treatment modality for patients with severe TO.10,11
At this time, we have received no clear direction from the surgical expert we consulted regarding a treatment approach.
1. Kim N, Hatton MP. The role of genetics in Graves’ disease and thyroid orbitopathy. Semin Ophthalmol. 2008 Jan-Feb;23(1):67-72.
2. Sergott RC, Glaser JS. Graves’ ophthalmopathy. A clinical and immunologic review. Surv Ophthalmol. 1981 Jul-Aug;26(1):1-21.
3. Fatourechi V, Bartley GB, Eghbali-Fatourechi GZ, et al. Graves’ dermopathy and acropachy are markers of severe Graves’ ophthalmopathy. Thyroid. 2003 Dec;13(12):1141-4.
4. Hasani-Ranjbar S, Mohajeri-Tehrani MR. Localized myxedema of the toe: a rare presentation of graves’ dermopathy. Arch Iran Med. 2008 May;11(3):326-9.
5. Richter DF, Stoff A, Olivari N. Transpalpebral decompression of endocrine ophthalmopathy by intraorbital fat removal (Olivari technique): experience and progression after more than 3000 operations over 20 years. Plast Reconstr Surg. 2007 Jul;120(1):109-23.
6. Khoo TK, Bahn RS. Pathogenesis of Graves’ ophthalmopathy: the role of autoantibodies. Thyroid. 2007 Oct;17(10):1013-8.
7. Garrity JA, Bahn RS. Pathogenesis of graves ophthalmopathy: implications for prediction, prevention, and treatment. Am J Ophthalmol. 2006 Jul;142(1):147-53.
8. Prabhakar BS, Bahn RS, Smith TJ. Current perspective on the pathogenesis of Graves’ disease and ophthalmopathy. Endocr Rev. 2003 Dec;24(6):802-35.
9. Karasek M, Lewinski A. Etiopathogenesis of Graves’ disease. Neuro Endocrinol Lett. 2003 Jun-Aug;24(3-4):161-6.
10. Bradley EA, Gower EW, Bradley DJ, et al. Orbital radiation for graves ophthalmopathy: a report by the American Academy of Ophthalmology. Ophthalmology. 2008 Feb;115(2):398-409.
11. Gorman CA, Garrity JA, Fatourechi V, et al. A prospective, randomized, double-blind, placebo-controlled study of orbital radiotherapy for Graves’ ophthalmopathy. Ophthalmology. 2001 Sep;108(9):1523-34.
12. Franklyn JA, Boelaert K. Thyrotoxicosis. Lancet. 2012 Mar 24;379(9821):1155-66.
13. Zhang L, Grennan-Jones F, Lane C, et al. Adipose tissue depot-specific differences in the regulation of hyaluronan production of relevance to Graves’ orbitopathy. J Clin Endocrinol Metab. 2012 Feb;97(2):653-62.
14. Boboridis KG, Bunce C. Surgical orbital decompression for thyroid eye disease. Cochrane Database Syst Rev. 2011 Dec 7;(12):CD007630.

