 A 62-year-old white female presented to the office as a new patient in July 2007 complaining of significantly blurred vision at both distance and near, as well as moderate irritation in both eyes. She underwent a laser thermal keratoplasty (LTK) procedure O.S. in 2001, with a subsequent touch-up approximately six months later. Her ocular history was significant for the presence of a freckle in her left eye.
A 62-year-old white female presented to the office as a new patient in July 2007 complaining of significantly blurred vision at both distance and near, as well as moderate irritation in both eyes. She underwent a laser thermal keratoplasty (LTK) procedure O.S. in 2001, with a subsequent touch-up approximately six months later. Her ocular history was significant for the presence of a freckle in her left eye.
Her current medications include: Macrobid (nitrofurantoin, Proctor & Gamble Pharmaceuticals), coumadin, omega-3 supplements and red yeast rice. She reported an allergy to sulfonamides.
Slit lamp examination of the anterior segment of the right eye was remarkable for fine superficial punctate keratitis (SPK) over the inferior one-third of the cornea, with a similar appearance in the left eye. The episclera was moderately injected O.U. The left cornea showed 16 LTK sites centered on the visual axis.
Intraocular pressure measured 15mm Hg O.D. and 16mm Hg O.S. Her anterior chamber angles O.U. were measured as grade 4 open by Van Herricks method.
Diagnostic Data
The patients uncorrected visual acuity was 20/25 O.D. and J3 O.S. Pupils were equal, round and reactive to light and accommodation, with no afferent pupillary defect. Extraocular muscles were full in all positions of gaze. Refractive findings revealed +0.50D 0.75D X 090, yielding 20/20 O.D., and -1.75D 0.25D X 105, yielding 20/20 O.S., with a +2.25D add to J1 at 16 inches.
Through dilated pupils, the crystalline lenses were clear O.U. Her cup-to-disc ratios were 0.30 x 0.30 O.D. and 0.15 x 0.15 O.S., with normal-sized discs.
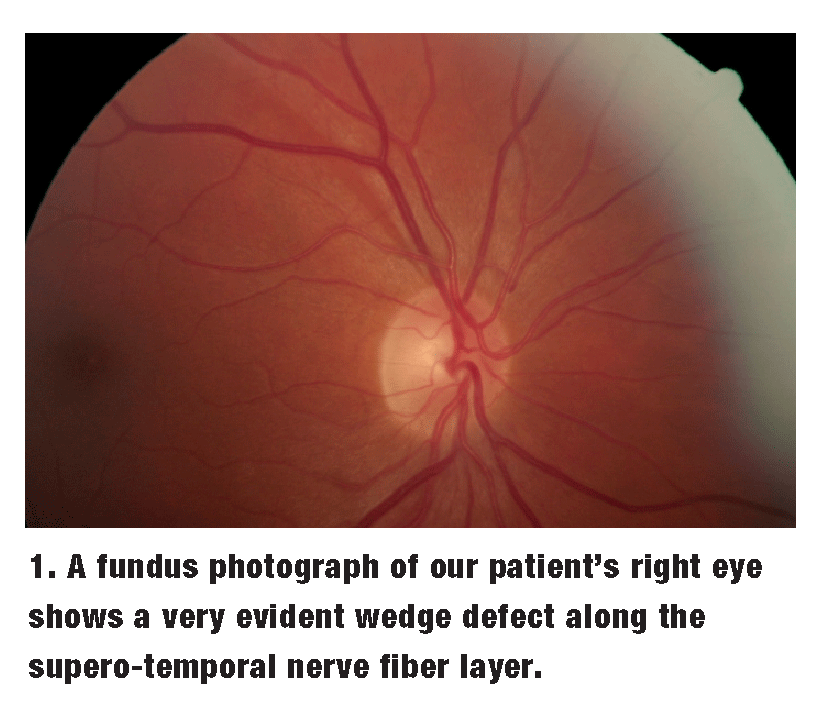 Both neuroretinal rims were plush and well perfused, and followed the ISNT (inferior-superior-nasal-temporal) rule O.U. Adjacent to the right optic nerve, along the supero-temporal nerve fiber layer (NFL), was a rather noticeable wedge defect, as shown in figure 1.
Both neuroretinal rims were plush and well perfused, and followed the ISNT (inferior-superior-nasal-temporal) rule O.U. Adjacent to the right optic nerve, along the supero-temporal nerve fiber layer (NFL), was a rather noticeable wedge defect, as shown in figure 1.
The vasculature in both posterior poles was normal, with no evidence of related systemic disease. Spontaneous venous pulsations were present bilaterally.
Both maculae were healthy, with a foveal reflex absent O.D. and present O.S. Above the superior arcades O.S. were two choroidal nevi, which measured approximately two disc diameters (DD) and 1DD in size, respectively. Both were flat with no overlying drusen. The peripheral retinal examination was normal.
I diagnosed her with inflammatory dry eye O.U., in addition to choroidal nevi O.S. Additionally, I suspected the patient may also have glaucoma, due to the NFL defect O.D. I prescribed FML (fluorometholone alcohol 0.1%, Allergan) O.U. t.i.d. for one week, b.i.d. for a second week, and q.d. for a final week. I discussed the NFL wedge defect with the patient, and she reported that this finding had never previously been brought to her attention.
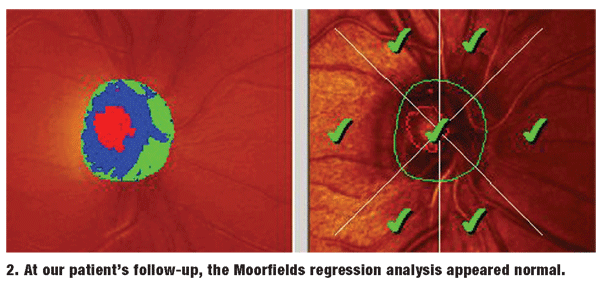
She returned in three weeks for a follow-up examination of her corneas and for additional investigation of the possible glaucoma O.D. She reported that both eyes felt markedly more comfortable and that her vision was crisper. At this visit, IOP measured 18mm Hg O.D. and 16mm Hg O.S. Pachymetry readings were 548m O.D. and 531m O.S. Threshold visual fields were reliable and demonstrated no abnormalities O.U.
Heidelberg Retina Tomograph-3 (HRT-3) imaging of both optic nerves demonstrated a symmetric double-hump TSNIT (temporal-superior-nasal-inferior-temporal) graph of the NFLs, and a normal Moorfields regression analysis of the neuroretinal rim characteristics (figure 2).
I asked her to continue tapering the FML for another week and to supplement corneal hydration with preservative tears over the long term. Some questions now arise: How would you handle her in terms of the wedge defect? Does she have glaucoma? When does she need to be seen again?
Discussion
Loss of the retinal NFL is a classic sign of glaucomatous optic nerve disease. In years past, before we had the currently available optic nerve imaging devices, NFL defects were difficult to visualize, even under the best circumstances.
Previously, we would occasionally be able to identify existing NFL defects in diagnosed glaucoma patients after our attention was already focused on critically evaluating the nerve fiber layer.
Photodocumenting NFL defects remains difficult even with clear media. Such defects are best seen under red-free light.
What is interesting in this case is the presence of a very obvious NFL wedge defect in one eye, while all other parameters pertaining to glaucoma are considered normal O.U. However, on close examination of the patients NFL wedge defect, it is clear that the defect narrows to an endpoint, just at the edge of the optic canal. Typically, NFL defects that are truly related to the glaucomatous optic neuropathy extend onto the neuroretinal rim. This commonly occurs in areas with the greatest neuroretinal rim thinning. Still, not all NFL defects are glaucomatous in origin.
With current technology available to assist us in differentiating healthy from glaucomatous optic nerves, the structural changes that occur at the optic nerve and the perioptic NFL are more readily detected. Bear in mind, however, that there are competing technologies in this area, and one imaging system may be more sensitive and specific to a particular parameter than another.
Some optometrists have regular access to more than one of the devices, and find that the collective information from each of the technologies is additive to the overall diagnostic process. Other clinicians, like myself, have access to only one technology, as it is prohibitively costly to have several of them in a private practice.
In this particular patient, both her TSNIT NFL thickness maps and Moorfields regression analysis were normal in both eyesparticularly in the area of the wedge defect O.D. Interestingly, a recent study looked at just such a patient population, in which localized NFL defects were present in the absence of visual field defects, and found that the optical coherence tomographys sensitivity was relatively poor at detecting such pre-perimetric NFL defects.1
However, another recent analysis of OHTS data looking at predictors for the development of glaucomatous optic neuropathy showed that scanning laser ophthalmoscopy and Moorfields regression analysis of the superior and inferior temporal nerve was able to predict change up to eight years before actual visual field loss.2
Concerning our patient, the entire glaucomatous landscape is normal except for an isolated wedge defect in the right eye, which is probably entirely unrelated to glaucoma. Therefore, I chose to simply monitor this patient.
Now, what if I had used a different technology that flagged the wedge defect as abnormal? Would that have changed the treatment plan? Being in private practice with limited funding, I do not have on-site access to multiple technologies. I believe that the HRT-3 provides me with extremely useful information on a day-to-day basis.
Even if one or more of the other technologies did show a different endpoint than the HRT-3, I still would have elected to monitor this patient simply because the entire glaucomatous picture is otherwise normal.
Use the technology available to you. But, do not abdicate clinical judgment in the process, as none of the available technologies replace our clinical acumen.
1. Kim TW, Park UC, Park KH, Kim DM. Ability of Stratus OCT to identify localized retinal nerve fiber layer defects in patients with normal standard automated perimetry results. Invest Ophthalmol Vis Sci 2007 Apr;48(4):1635-41.

