 The prevalence of obesity among children is rapidly increasing, so much so that statistics quickly become obsolete. Today, the problem has become a true pandemic.1 Consequently, the prevalence of type 2 diabetes mellitus (T2DM) in children is on the rise.
The prevalence of obesity among children is rapidly increasing, so much so that statistics quickly become obsolete. Today, the problem has become a true pandemic.1 Consequently, the prevalence of type 2 diabetes mellitus (T2DM) in children is on the rise.
As many as one in three children born in the year 2000 will develop T2DM as adults.2,3 Prior to 1990, less than 4% of new cases of diabetes in children was type 2.1 But by 1999, T2DM accounted for as much as 46% of new pediatric cases.2,4-6 Alarmigly, such young individuals with diabetes may develop heart disease by age 30.2
Fortunately, the increased diabetes prevalence in children has not yet reached pandemic proportions.6,7 We can intervene and prevent T2DM from affecting more youth primarily by addressing childhood obesity.4 A public health approach would likely be most successful—with health care providers and community organizations promoting active, healthy lifestyles.8,9
Optometrists are uniquely positioned to reach out to a large number of children and families. Not only can we provide our traditional role in screening for retinopathy, but we can also actively identify at-risk youth. Having a thorough understanding of T2DM in children can help us be better educators and community partners in the prevention of this devastating disease.
The Obesity Epidemic
The origin of T2DM in children is widely associated with the worldwide obesity epidemic.9 Obesity is a hallmark predictor and underlying cause of T2DM, with up to 85% of children being overweight at the time of diagnosis.8 While certain people may be hereditarily susceptible, the obesity epidemic evolved too quickly to be solely a genetic problem. Because obesity is a global concern that knows no racial or ethnic boundaries, we know that several environmental factors play a significant role.
No race or gender is immune to obesity. At least 20% of the adult populations in countries ranging from the Pacific Islands to Germany and Bahrain to South Africa are obese or severely overweight.1 Even more alarming, 39% of Native American children, 24% of African- and Mexican-American children and 13% of white children in the United States are overweight; the overall prevalence is highest for Mexican-American boys and African-American girls.2
• Dietary considerations. It is a very simple equation: Obesity develops when caloric intake exceeds metabolic output. Several studies have shown that caloric intake among children has not really changed from the 1970s to 2000. The foods and drinks that children consume have changed dramatically, however. Interestingly, fat content in American children's diets actually has decreased over the last 30 years.10 But, artificial drink (soda, sports drinks, partial juice drinks) consumption has increased by nearly 500% in the last five decades.10 In fact, teenagers get 11% of their daily caloric intake from soda.2 It is inconclusive whether sugary drinks directly promote weight gain (because such soft drinks have largely displaced whole milk consumption), but several studies have shown that for every additional serving of soda, the frequency of obesity rises.2,10
• Physical activity levels. In addition to diet, the other primary contributory factor to the obesity epidemic is decreased physical activity. There is overwhelming evidence that lifestyles have become much more sedentary during the last two decades. Many schools have eliminated physical education (and even recess) in order to meet performance standards. Only one out of five children have gym class each week.10 Driving to school instead of walking, as well as an average of 5.5 hours spent per day sitting in front of a television or computer screen clearly contribute to reduced energy expenditure.1,2,10
Pathophysiology of T2DM in Children
Diabetes develops when there is an imbalance between insulin secretion by the beta cells of the pancreas and insulin action. In patients with T2DM, both insulin action and secretion may be impaired.
Initially, there is insulin resistance by the cells in the body. Then, the beta cells hypersecrete insulin in an effort to restore/maintain normoglycemia. When the beta cells cease the overproduction of insulin, clinical diabetes manifests.8
Puberty has a significant influence on the development of T2DM in children. During puberty, the increase in growth hormone (GH) causes insulin resistance. The body compensates by hypersecreting insulin. As GH declines in a normal patient, so does insulin resistance. It is believed that puberty-induced insulin resistance, along with the obesity-related reduction in glucose metabolism, is what leads to hyperglycemia and eventually T2DM.8
Identify Major Risk Factors
• Obesity is the number one risk factor for the development of T2DM.9 A child is considered overweight by the Centers for Disease Control and Prevention if he or she is above the 95th percentile of body mass index (BMI) for his or her respective age and gender. Further, a child is considered to be at risk for being overweight if he or she is at the 85th percentile of BMI.10 There is no official definition for obesity in children.11
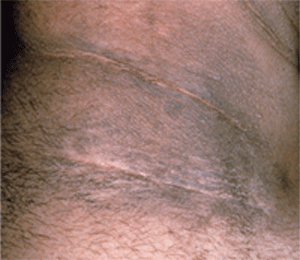
1. Overweight children who exhibit acanthosis nigricans, as seen here, are substantially more likely to develop type 2 diabetes than normal-weight children. (Image courtesy of
www.visualdx.com© Logical Images, Inc.)
• Family history is also strongly associated with T2DM. Statistics show that anywhere between 45% and 80% of children who have been diagnosed with T2DM has at least one parent with diabetes. The association is even stronger with an additional first- or second-degree relative (74% to 100%).8,9 This risk factor may be as much about family lifestyle as it is genetic.
• Race and gender are also risk factors for T2DM in children. Ethnic groups at higher risk for T2DM development include: Native Americans, Alaskan natives, African-Americans, Hispanics and Pacific Islanders.11 Young girls are 1.7 times more likely than young boys to be diagnosed with T2DM, but this gender difference does not hold true for adults.9
•Other conditions are often associated with insulin resistance, including hypertension, dyslipidemia, polycystic ovarian syndrome (PCOS) and acanthosis nigricans (AN). 11 AN is one of the most easily identifiable markers for diabetes risk. The condition is characterized by hyperpigmentation and a thickening of the upper layers of the skin (figure 1). When AN is noted, 93% to 99% of presentations appear on or around the folds of the neck. It also can present on the axilla, elbows and the knees. The prevalence of AN increases with the number of risk factors for T2DM. Just 3% of normal-weight patients have AN. Children with AN are 1.6 to 4.2 times more likely to have hyperinsulinemia and are 1.97 times more likely to be diagnosed with T2DM.12,13
Screening and Diagnosis
It seems that population-based screening would be prudent. However, the World Health Organization has very specific criteria that must be met, and T2DM has not yet satisfied those requirements. The current American Diabetes Association (ADA) screening guidelines mandate that only children who are at risk for being overweight or who are overweight and meet two of the following should be screened:
- Family history of T2DM in first- or second-degree relative.
- Race/ethnicity (Native American, Alaskan, African-American, Hispanic, Asian American, Pacific Islander).
- Presence of a condition associated with insulin resistance, including AN, dyslipidemia, hypertension or polycystic ovarian syndrome.
- Maternal history of diabetes during the child’s gestation.
This protocol is to be implemented at age 10 or when the child enters puberty.9,11,14, 15
In 2010, the ADA expanded its diagnostic testing guidelines to include the hemoglobin A1c (HbA1c). The current standard of medical care in diabetes includes the following diagnostic criteria:
- HbA1c greater than 6.5%.
- Fasting plasma glucose (FPG) greater than or equal to 126 mg/dl (fasting is defined as no caloric intake within eight hours.)
- Oral glucose tolerance test (OGTT) or two-hour plasma glucose greater than or equal to 200mg/dl.
- Random plasma glucose (RPG) greater than or equal to 200mg/dl in a symptomatic patient.
Diabetes is confirmed when there is a repeatable result on any of the diagnostic tests, if two different tests yield abnormal results, or if the clinical presentation is consistent with the diagnostic test results (such as with RPG in a symptomatic patient). If two different tests yield discordant results, the abnormal test is repeated for confirmation.15
Treatment
The short-term treatment goal is to normalize the blood glucose and HbA1c. The long-term goal is to decrease the risk of the complications secondary to diabetes.8 Lifestyle changes continue to be the cornerstone of T2DM management.
The U.S. Diabetes Prevention Program showed that diet and exercise were more effective than metformin in reducing the progression to diabetes in patients who were considered pre-diabetic.11 Those types of lifestyle changes can be very difficult, and it is estimated that just 10% of patients with diabetes can control their disease with diet and exercise alone.9 Treatment guidelines for children begin with lifestyle intervention, but if the glucose levels do not normalize within three months, medical therapy should be initiated.11
Currently, just insulin and metformin are FDA approved for the treatment of diabetes in children.6 In clinical practice in the U.S., treatment appears to be equally divided between insulin and metformin.9 Doctors also may recommend off-label use of other diabetes drugs that are FDA approved for adults.
Ocular Complications
The ocular and systemic complications of diabetes are well known. Although the landmark ophthalmological studies (e.g., the Early Treatment of Diabetic Retinopathy Study and the Epidemiology of Diabetes Interventions and Complications Study) have expressly examined the effects of diabetes on adults, we assume that children with T2DM will manifest similar complications.
Like adults with T2DM, children may have retinopathy present at the time of diagnosis. So, according to the ADA guidelines, children with T2DM should have an initial dilated eye exam at the time of diagnosis and then again on a yearly basis (or sooner, if retinal changes manifest).6,8,11 To date, no large-scale studies have evaluated the prevalence of retinopathy in children with T2DM. But, one small study suggests that it is less than 4%.16
There appears to be some differences in ocular findings between patients with type 1 diabetes mellitus (T1DM) and T2DM. In general, retinopathy occurs more frequently in children with T1DM, but patients with T2DM tend to have a shorter disease duration before the appearance of retinopathy.6 Likewise, autonomic neuropathy tends to occur much sooner in children with T2DM. Autonomic neuropathy, evaluated by pupil size before and after a light stimulus, appears to be the same for both T1DM and T2DM patients. However, more than half of the T2DM patients studied had autonomic neuropathy after a median of 1.3 years of disease onset.16
There appears to be a direct relationship between increased BMI and the risk of retinopathy; however, the pathophysiology of this link remains unknown. It may be that hypertension and hyperlipidemia are merely independent risk factors for both obesity and retinopathy. Or, it may be that obese individuals tend to have hyperleptinemia. Leptin is a cytokine secreted by fat cells. It causes reactive oxygen species to accumulate around cells, causing increased oxidative stress. Both hypertensive and diabetic retinopathy are associated with high levels of plasma leptin.
Interestingly, there is evidence of a more direct relationship between obesity and proliferative retinopathy: Vascular endothelial growth factor (VEGF) tends to be elevated in obese individuals. It is unknown if weight loss would lead to the regression of retinopathy, but it is generally accepted that a decrease in BMI would reduce the risk of retinopathy.17
The O.D.’s Role
Screening for retinopathy is the obvious role for optometrists in caring for children with T2DM. But, we may be able to play a more critical role in identifying children at risk. We see a lot of children who have failed school vision screenings. Many of these children do not receive annual wellness exams. In fact, one survey indicated that 62% of three to six year olds and just 52% of seven to 11 year olds who have a pediatrician actually get an annual wellness check-up.18
Even children who see a pediatrician annually may not be getting screened for diabetes. A 2004 study at a large, high-risk clinic in Chicago showed that just 38% of children who met the criteria for diabetes screening actually had tests ordered.14 Another study conducted in 2006 showed a screening rate of just 45%.5 Electronic medical records can improve this statistic, because BMI can be calculated automatically and the system can flag those who should be tested. More importantly, optometrists can help identify children at risk, even though most do not have the capability of obtaining a BMI. Merely recognizing risk factors—such as ethnicity, family history and AN—is sufficient to make a follow-up recommendation with a pediatrician.
Optometrists should also play a major role in diabetes education. Discussing T2DM with children is very complex. It is well recognized that diabetes education must be team-oriented. For children, the team must include both parents and siblings.6 Adolescents are rarely motivated by long-term health consequences, so discussing the risk of blindness may not be useful.11 Admonishing a patient for not self-monitoring blood glucose is not helpful, because testing generally is conducted as needed, when sick or when symptomatic for hyper- or hypoglycemia.8 Discussing diet is also fraught with complications, because nutritional counseling must be appropriate for the patient’s culture and resources.8
Exercise, however, is the one aspect of T2DM management that optometrists should consider discussing with child-aged patients. Encouraging children to stay away from the television and computer and go outside can be helpful. Thirty minutes of continuous activity per day is all that is recommended.8 Ideally, this discussion should be had with all children in an attempt to prevent obesity and/or the future development of T2DM.9
Ultimately, the most important role for optometrists in the co-management of children with T2DM is to serve as the communication facilitator. Optometrists must communicate with pediatricians regarding the children seen in their offices. Because obesity is a public health problem and so few children receive regular physical exams, we must do our part to help identify children at risk. Simply suggesting that a child receive a routine physical is important and may mean the difference between diabetes prevention and devastating life-long complications. A letter to the pediatrician recommending an exam, including an evaluation of risk factors for diabetes, is a simple way to assist in the early detection and even prevention of future complications.
Optometrists’ traditional role in managing diabetes patients is the identification and appropriate referral of retinopathy. However, the increasing prevalence of T2DM in children shifts our primary role as eye care provider to one of public health advocate. Simple awareness of risk factors, assessing the patient’s family history, observing the patient and a little communication can go a long way in not only reducing the obesity epidemic, but also preventing a massive outbreak of T2DM in children during the next few decades.
Dr. Martin is in private practice in Sedona, Ariz. at Southwestern Eye Center, a state-wide referral center. She thanks Wendy Tuccille, M.D., of Red Rock Pediatrics in Cottonwood, Ariz. for her assistance in obtaining reference materials.
1. Prentice AM. The emerging epidemic of obesity in developing countries. Int J Epidemiol. 2006 Feb;35(1):93-9.
2. Wieting JM. Cause and effect in childhood obesity: solutions for a national epidemic. J Am Osteopath Assoc. 2008 Oct;108(10):545-52.
3. Shah S. Screening for type 2 diabetes in obese youth. Pediatrics. 2009 Aug;124(2):573-9.
4. Kaufman FR. Type 2 diabetes mellitus in children and youth: a new epidemic. J Pediatr Endocrinol Metab. 2002 May;15 Suppl 2:737-44.
5. Shikha GA, Mehta SD, Adams WG. Diabetes mellitus screening in pediatric primary care. Pediatrics. 2006 Nov;118(5):1888-95.
6. Bowen ME, Rothman RL. Multidisciplinary management of type 2 diabetes in children and adolescents. J Multidiscip Healthc. 2010 Jul 28;3:113-24.
7. Gora MI, Davis J, Kelly L, et al. Low prevalence of pediatric type 2 diabetes: where’s the epidemic? J Pediatr. 2008 Jun;152(6):753-5.
8. American Diabetes Association. Type 2 diabetes in children and adolescents. Diabetes Care. 2000 Mar;23(3):381-9.
9. Alberti G, Zimmet P, Shaw J, et al. Type 2 diabetes in the young: the evolving epidemic: the international diabetes federation consensus workshop. Diabetes Care. 2004 Jul;27(7):1798-811.
10. Dehghan M. Childhood obesity, prevalence and prevention. Nutr J. 2005 Sep 2;4:24.
11. Gahagan S, Silverstein J. Prevention and treatment of type 2 diabetes mellitus in children, with special emphasis on American Indian and Alaska Native children. American Academy of Pediatrics Committee on Native American Child Health. Pediatrics. 2003 Oct;112(4):e328.
12. Kong AS, Williams RL, Rhyne R, et al. Acanthosis nigricans: high prevalence and association with diabetes in a practice-based research network consortium—a PRImary care Multi-Ethnic Network (PRIME Net) study. J Am Board Fam Med. 2010 Jul-Aug;23(4):476-85.
13. Kong AS. Acanthosis nigricans and diabetes risk factors: prevalence in young persons seen in southwestern US primary care practices. Ann Fam Med. 2007 May-Jun;5(3):202-8.
14. Drobac S, Brickman W, Smith T, Binns HJ. Evaluation of a type 2 diabetes screening protocol in an urban pediatric clinic. Pediatrics. 2004 Jul;114(1):141-8.
15. American Diabetes Association. Executive summary: standards of medical care in diabetes--2011. Diabetes Care. 2011 Jan;34 Suppl 1:S4-10.
16. Eppens MC, Craig ME, Cusumano J, et al. Prevalence of diabetes complications in adolescents with type 2 compared with type 1 diabetes. Diabetes Care. 2006 Jun;29(6):1300-6.
17. Cheung N. Obesity and eye diseases. Surv Ophthalmol. 2007 Mar-Apr;52(2):180-95.
18. Hart C. Well-Child Check-ups. Practice Management Online 2010; Spring. Available at:
http://practice.aap.org/content.aspx?aid=2927 (accessed July 8, 2011).

