 Q: I work with an excellent cataract surgeon, but occasionally I see one-day post-op patients who come in with pretty beat-up corneas. This catches me by surprise, and I dont know what to tell the patient. Any suggestions?
Q: I work with an excellent cataract surgeon, but occasionally I see one-day post-op patients who come in with pretty beat-up corneas. This catches me by surprise, and I dont know what to tell the patient. Any suggestions?
A: Nobody likes to be caught off guard. And no optometrist likes to appear surprised and unaware of the details of the patients surgery, especially when that patient is sitting right in front of you.
Cataract comanagement is a two-way street. You send the patient to the surgeon and communicate important details that may affect the outcome. Likewise, you should expect to be notified of anything unusual that happened during the case.
In our center, we send a fax or an e-mail on the day of surgery that tells the referring O.D. if it was a routine case, says optometrist Alex Ward, a resident in ocular disease at Omni Eye Services in
If your cataract surgeon is not communicating this information to you, simply ask him or her to do so. At the very least, ask your surgeon to notify you about the difficult cases. Reasonable surgeons will respond to this reasonable request.
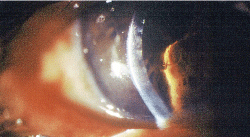
Knowing what happened during surgery can prepare the you to handle post-op complications, such as corneal edema.
Q: Is there a way to predict corneal edema before cataract surgery? What causes it?
A: Most of the time, post-op corneal edema can be predicted before cataract surgery, Dr. Ward says. Some things to look for:
Dense cataracts. Very dense cataracts require more phacoemulsification energy. The more energy used and the longer the phaco time, the more likely the endothelium will take a beating, causing corneal edema. While all phaco instruments provide the phaco time, some of the newer ones also measure the amount of energy used over time (cumulative dissipated energy, or CDE). In the post-op letter, your cataract surgeon should provide this information to you, if available.
Shallow anterior chamber. A patient who presents with a shallow anterior chamber before surgery can return with a lot of corneal edema after surgery. The reason is that the surgeon has to phacoemulsify so close to the cornea that it can cause some shock to the endothelium, which results in corneal swelling at the one day post-op visit and beyond.
Pre-existing corneal disease. A patient with an endothelial dystrophy (such as guttata on the endothelium or Fuchs endothelial dystrophy) is at greater risk for developing post-op corneal edema.
High intraocular pressure. When you see unexplained post-op corneal edema, the first thing to do is get an accurate pressure reading. A likely cause: Viscoelastic from the surgery may be lodged in the angle, which prevents proper drainage and increases the intraocular pressure.
If the patients IOP is between 25mm Hg and 35mm Hg, put the patient on a hypotensive agent, such as brimonidine or a beta-blocker. If the IOP is above 35mm Hg, then you or the surgeon needs to burp the wound to relieve the pressure immediately. (This entails applying pressure with a sterile cotton swab or a 30-gauge needle adjacent to the parecentesis site, which temporarily opens up the wound to allow excess aqueous to escape.)
Regardless of the cause of the corneal edema, reassure the patient that it will usually resolve within a week. In cases of elevated IOP, have the patient return in a two to three days to make sure the pressure is under control.

