 History
History
A 46-year-old white male presented to the emergency service complaining of flashing lights in his left eye for the last three days. The phenomenon occurred in the temporal portion of the visual field of his left eye every five minutes.
He denied perceiving any floating spots or changes in visual acuity, and reported no pain or injury to the eye or head.
His ocular history was remarkable for lattice degeneration O.U. His systemic history was unremarkable. He denied any history of previous illness or use of medications.
Diagnostic Data
His best-corrected visual acuity was 20/20 O.U. at distance and near. External examination was normal, and there was no evidence of an afferent pupillary defect.
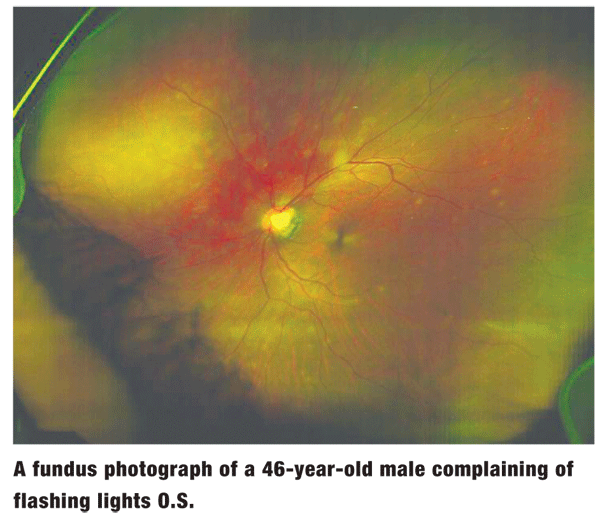
Anterior segment examination was unremarkable O.U. Intraocular pressure measured 15mm Hg O.U. The pertinent posterior segment findings in the left eye are illustrated in the photograph.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests?
What is your diagnosis? How would you manage this patient? What is the likely prognosis?
Thanks to Kim Deugwillo, O.D.,
The Diagnosis
The diagnosis in this case is multiple evanescent white dot syndrome (MEWDS) O.S. The white dot syndromes are an uncommon, idiopathic group of inflammatory disorders affecting the retina and/or choroid.1-5 Patients usually present with some or all of the following visual complaints: acute or subacute decrease in visual acuity, central or paracentral scotomas, photopsia and floaters. MEWDS is often detected by laterality tests, fluorescein angiography and/or maintaining a thorough patient history.
In this case, treatment consisted of patient education and close monitoring for one month using dilated funduscopic examinations (DFE).
MEWDS normally occurs in otherwise healthy women in the third to fourth decades of life, usually appearing after a viral prodrome.1-5 Case reports have also noted development of the syndrome following both hepatitis A and yellow fever vaccinations.6
The etiology of the disorder remains unknown; but, a genetic predisposition for the disorder has been suggested.6
The DFE often reveals multiple small gray-white dots in the posterior pole at the level of the retinal pigment epithelium, which usually do not develop on the fovea. The dots appear and disappear quickly. Associated findings may include an afferent pupillary defect, foveal granularity, vitritis, anterior chamber reaction, optic disc edema and an enlarged bling spot.1-5
Fluorescein angiography shows early puntate staining hyperfluorescence in a "wreathlike" pattern, and late staining of the dots. The dots spontaneously disappear, and the vision returns to normal in approximately three to 10 weeks.1-4 Recurrence of the syndrome is rare.
The white dot syndromes include acute macular neuroretinopathy, acute posterior multifocal placoid pigment epitheliopathy (APMPPE), acute pigment epithilitis (Krill"s disease), birdshot choroidopathy (vitiliginous chorioretinitis), multifocal choroiditis and panuveitis (MCP), subretinal fibrosis and uveitis syndrome, and punctate inner choroidopathy.1-5
Controversy exists as to whether the white dot syndromes are simply variants of one particular disorder, or if there are actually different etiologies for each condition. Nonetheless, prompt and accurate diagnosis is needed to properly treat and manage each case, as well as develop an appropriate follow-up plan.
1. Gasch AT. The white dot syndromes. Am J Ophthalmol. 2004 Mar;137(3):538-50.
2. Gass JD, Hamed LM. Acute macular neuroretinopathy and multiple evanescent white dot syndrome occurring in the same patients. Arch Ophthalmol. 1989 Feb;107(2):189-93.
3. Gross NE, Yannuzzi LA, Freund KB, et al. Multiple evanescent white dot syndrome. Arch Ophthalmol. 2006 Apr;124(4):493-500.
4. Quillen DA, Davis JB, Gottlieb JL, et al. The white dot syndromes. Am J Ophthalmol. 2004 Mar;137(3):538-50.
5. Polk TD, Goldman EJ: White-dot chorioretinal inflammatory syndromes. Int Ophthalmol Clin 1999 Fall;39(4):33-53.
6. Stangos A, Zaninetti M, Petropoulos I, et al. Multiple evanescent white dot syndrome following simultaneous hepatitis-A and yellow fever vaccination. Occul Immunol Inflamm 2006 Oct;14(5):301-4.

