 Q: I frequently send patients for treatment of wet AMD. Some get Lucentis, some Avastin, some Eyelea—what’s the difference, and why does every retina specialist seem to have a different protocol?
Q: I frequently send patients for treatment of wet AMD. Some get Lucentis, some Avastin, some Eyelea—what’s the difference, and why does every retina specialist seem to have a different protocol?
A: “Most distinctions in practice patterns involving these agents have to do with patient affordability, practice overhead and patient demographics, as well as the indicated conditions,” says Mohammad Rafieetary, O.D., of the Charles Retina Institute in Memphis.
Lucentis (ranibizumab, Genen-tech/Roche), Avastin (bevacizumab, Genentech/Roche) and Eylea (aflibercept, Regeneron) are all anti-vascular endothelial growth factor (VEGF) agents that have shown efficacy in the treatment of CNV associated with wet AMD, he says.
So how are they different? Pharmacologically, Lucentis has a greater affinity for VEGF (in vitro) than Avastin, but Avastin improves visual acuity as well as Lucentis in clinical studies. Eylea is longer lasting than both Lucentis and Avastin, and is possibly more efficacious because it binds to both VEGF-A and placental growth factor (PGIF). “These factors, plus the physiologic differences between diseases, play a significant role in the selection of a specific agent,” he says.
Retina specialty practices that treat these conditions must have Avastin available for off-label use, because the other agents have limited FDA approval and therefore restricted third-party coverage, he says. “Practically speaking, availability of the drastically cheaper Avastin (as low as $50) allows a segment of patients to be treated who otherwise might not have access. This consideration, combined with the apparent equivalence of Avastin and Lucentis in clinical efficacy, have led some vitreoretinal practitioners to use only Avastin due to the significant overhead cost incurred by Lucentis (about $2,000 per injection),” Dr. Rafieetary explains. “However, most have Lucentis and Eylea available for approved diseases, and use Avastin for all others.”
The recent Comparison of Age-Related Macular Degeneration Treatment Trials (CATT) provided insight on the similarities and differences between Avastin and Lucentis.1 After one year of treatment, vision scores were equivalent for the monthly injection groups between Lucentis and Avastin, but the Avastin group revealed more patients with subretinal fluid still present on time-domain OCT, as well as more patients with leakage on angiography. The two-year results demonstrated similar findings, but used spectral-domain OCT, and noted a higher incidence of geographic atrophy in patients undergoing Lucentis therapy who did not have this finding at study initiation.
“These results suggest that while both Lucentis and Avastin are efficacious, Lucentis is associated with improved anatomical findings as revealed by OCT and FA,” Dr. Rafieetary says. “Only long-term experience will demonstrate if there is any true difference in efficacy between these two medications, although the cautious observer would likely argue that both are reasonable options for AMD, and both offer significant improvements over previous treatments.”
In November 2011, the FDA approved Eylea for wet AMD. Its chief advantage is its reduced number of doses: It is dosed monthly for the first three months, then—unlike Lucentis or Avastin—every other month thereafter. Each dose of Eylea costs about $1,850.
“Anecdotally, our practice, which uses a morphology-based approach to treat AMD, has found that many patients are able to extend the time between injections with Eylea to six weeks,” Dr. Rafieetary says. “Another observation is that pigment epithelial detachments often flatten quicker with Eylea, giving the false appearance of increased subretinal fluid after the first administration. Only time will tell if Eylea is truly a superior or equivalent drug to Lucentis and Avastin, and if it is as clinically effective for decreasing the treatment burden of intravitreal injections.”
Overall, Lucentis, Avastin and Eylea are all good choices for AMD, he says. There is no clear difference in visual acuity outcomes to date between these three medications.
Q: What is my role in comanaging these patients?
A: “The optometrist plays a critical role in the management of AMD patients,” Dr. Rafieetary says. In patients with atrophic disease, counseling, education and periodic examination are essential, he explains. Patients with more severe cases require early detection of conversion from dry to wet AMD, along with prompt referrals to retina specialists.
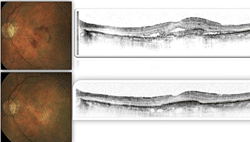
Fundus photo and OCT scan of AMD with CNV and subretinal hemorrhage (top), which is significantly improved (bottom) following a single intravitreal anti-VEGF injection.
“As with any referral, be sure to at least suggest a diagnosis prior to referral. Make the appointment for the patient, and document that you did so clearly in the chart,” he says.
In the early stage of treatment, when most patients require monthly injections by the retina specialist, there may be a gap in patients’ visits to their referring optometrist. “In remote and rural areas, patients may have difficulty returning to the specialist for every follow-up exam,” Dr. Rafieetary says. “So, AMD patients are often comanaged in alternating visits between the specialist and the local optometrist. In this scenario, OCT examinations can detect subtle areas of increased fluid, which is currently the most common re-treatment criterion. When applicable, images can be electronically shared between the providers, which can speed communication.”
The doctor of optometry is also an essential resource in cases where the patient might have co-existing conditions and/or unusual or unexpected symptoms that might require immediate care. Finally, he adds, refractive exams––and particularly low vision aids––remain an integral aspect of care for many AMD patients.
1. Comparison of Age-related Macular Degeneration Treatments Trials (CATT) Research Group. Martin DF, Maguire MG, Fine SL, et al. Ranibizumab and bevacizumab for treatment of neovascular age-related macular degeneration: Two-year results. Ophthalmology. 2012 Jul;119(7):1388-98.

