 |
A 54-year-old female presented to the emergency room with a new onset of painless vision loss in her left eye. She stated that she noticed a shadow in the upper left quadrant of her left eye about one week ago. She has a history of an overactive bladder and three months prior was started on Myrbetriq (mirbegron, Astellas Pharma); however, she was then switched to Vesicare (solifenacin succinate, Stellas Pharma) as the Myrbetriq caused headaches.
Her initial blood pressure at triage was elevated at 155/70mm Hg; however, this normalized shortly after and stayed less than 120/80mm Hg for the remainder of her hospitalization. She attributed the blood pressure elevation to stress upon arrival at the emergency department. She was afebrile with normal respiratory rate and pule oxygen.
The patient’s visual acuity was 20/20 OD and 20/40 OS. There was a trace afferent pupillary defect in the left eye. Extraocular motilities were full and smooth. Intraocular pressures were 18mm Hg OD and 17mm Hg OS. She reported about 10% decreased brightness and red desaturation in the left eye. Anterior segment exam was unremarkable. Dilated retinal exam revealed significant optic nerve edema in the left eye (Figure 1).
Differentials for her disc edema included non-arteritic ischemic optic neuropathy (NAION), arteritic ischemic optic neuropathy (AION), optic neuritis, a compressive lesion and neuroretinitis. After the patient was admitted, I (Dr. Trottini) ordered an MRI of her brain and orbits, as well as a complete blood count and other blood tests, including antinuclear antibody and lipid profile. I also recommended blood pressure monitoring.
At the follow-up 24 hours later, her clinical exam was stable. MRI was unremarkable, most serology testing was normal and her blood pressure was monitored and normal. She was discharged with a likely diagnosis of NAION and was instructed to see me in the office the following day for a visual field examination.
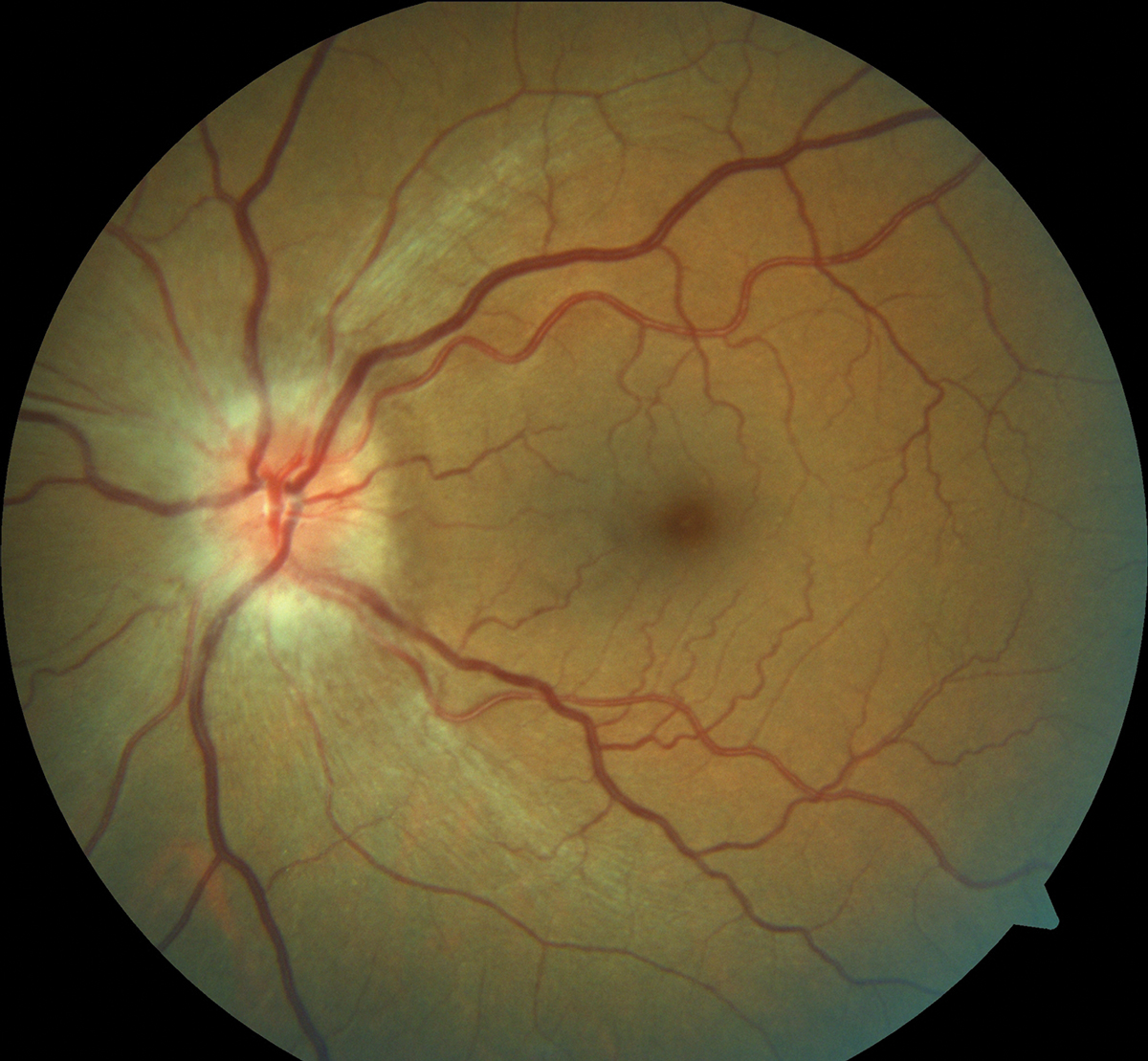 |
This NAION patient presented with significant optic nerve edema. Click image to enlarge. |
Constant Monitoring
The patient’s visual field tests showed a minimal superior temporal defect. No treatment was indicated and, given her normal work-up thus far, I recommended to follow-up again in a month to repeat the visual field. I also asked to her to follow-up with her medical doctor to continue monitoring for any possible microvascular issues as well as a hypercoagulopathy work up.
On follow-up one month later, her visual field did show some progression. Her visual acuity was stable at 20/40, her disc edema was resolved and the optic disc was diffusely pale. Her serology testing from her hospitalization was now finalized and normal.
Although the field did look slightly worse from baseline, given her clinical picture, normal testing, stable visual acuity and resolved disc edema, I continued to follow her without any treatment recommendations. She did see her internist for a coagulopathy work-up which was unremarkable.
I recommended she start a daily 81mg aspirin and continue to see her medical doctor as directed. As of our last visit, approximately four months from the onset of her NAION, her visual field showed spontaneous recovery of most of her defect. She had also noticed this improvement subjectively and was pleased to regain most of her vision.
Discussion
NAION is caused by an infarction of the short posterior ciliary arteries, which supplies the anterior portion of the optic nerve.1 Vision loss is sudden, painless and usually presents upon awakening as some authors contribute NAION to nocturnal hypotension.1
NAION is typically seen in individuals older than 50 and in patients with a small cup-to-disc ratio “disc at risk.”1,2 Clinical findings include unilateral disc edema, decreased vision and visual field loss. NAION patients often present with visual field defects, most commonly inferior nasal and inferior altitudinal defects.3
Major risk factors include microvascular disease such as diabetes, hypertension and hypercholesterolemia. Additional risk factors include optic disc drusen, smoking, anemia, hypercoagulopathies and obstructive sleep apnea.1,2
NAION, AION and optic neuritis can share similar symptoms and clinical findings; however, they are all different entities. So, it’s important to differentiate between each one.
AION is ischemia to the short posterior ciliary arteries and optic nerve secondary to inflammation. This is commonly seen in patients older than 65, with unilateral disc edema, significantly greater visual acuity and field defects. Symptoms of giant cell arteritis such as headache, fatigue and scalp tenderness are typical in AION. Elevated erythrocyte sedimentation rate (ESR), C-reactive protein (CRP) and platelets levels also raise additional suspicion for AION. If not diagnosed and treated, the fellow eye can become affected and vision loss is typically permanent.
Optic neuritis is typically seen in younger individuals (between the ages of 20 and 40), can occur as unilateral vision loss with or without pain and will most commonly affect the retrobulbar portion of the optic nerve. The disc is usually normal in appearance or mildly edematous in a third of cases.4 High T2 signal and contrast enhancement of the optic nerve is generally seen on MRI.
Optic neuritis can present idiopathically or as a result of disorders such as multiple sclerosis, lyme, syphilis or sarcoidosis.
Treatment
Serial visual field testing helps determine improvement or progression of the field defects. Repeated clinical examination should show resolution of the disc edema, with optic nerve pallor forming shortly after. NAION treatment from an optometric standpoint is largely observational. There is no generally accepted, definitive treatment for NAION presently.2
Data on treating NAION with anticoagulation, steroids, pressor agents, vasodilators or optic nerve decompression have not shown significant advantages.2 Some studies show that steroids can help improve visual function; however, the design of these studies as well as the side effects of higher doses of steroids in older patients with vascular disease weaken those findings.1,5
While aspirin hasn’t been confirmed to be beneficial for treating acute NAION or prevention of NAION in the fellow eye, I recommend patients take an 81mg daily aspirin if they aren’t already taking any anticoagulation. This will possibly reduce the risk of stroke or myocardial infarction.2
NAION will generally stabilize after two to three months with a guarded visual prognosis, and acuity can improve up to three lines in 43% of patients. There is a less than 5% chance of recurrence in the same eye and a 15% chance of the fellow eye’s involvement at five years.1,2
Issues such as diabetes, hypertension, hypercholesterolemia and sleep apnea as well as possible nocturnal hypotension need to be tightly controlled by the internist. Identifying and controlling these underlying causes takes careful communication between specialties. Discuss with the patient’s primary doctor over the phone instead of just e-mail correspondence to ensure the appropriate management plan.
This patient was interesting because she didn’t have any risk factors associated with NAION. She was taking Myrbetriq and discontinued it a few weeks prior to onset of her NAION. Myrbetriq can cause hypertension, but our patient’s internist discontinued the medication for her because she was reporting headache but did not check her blood pressure prior to discontinuation. Her medical history was unremarkable otherwise, and her work up was extensive and unrevealing.
Additionally, her visual field defect was not one most commonly seen with NAION. Although not the classical presentation of NAION, her marked disc edema, painless vision loss, relatively good visual acuity, mild visual field defect and normal imaging/work-up made it the most likely diagnosis.
Although no universally accepted treatment for NAION exists, a thorough work-up is necessary to identify any underlying causes and ensure those issues are managed appropriately. It is also of the utmost importance to rule out AION, optic neuritis and other etiologies, as they each require a much different treatment.
1. Berry S, Lin WV, Sadaka A, Lee AG. Nonarteritic anterior ischemic optic neuropathy: cause, effect and management Eye Brain. 2017;9:23-8. 2. Atkins EJ, Bruce BB, Newman NJ, Biousse V. Treatment of nonarteritic anterior ischemic optic neuropathy. Surv Ophthalmol. 2010 55(1):47-63. 3. Hayreh SS, Zimmerman B. Visual field abnormalities in nonarteritic anterior ischemic optic neuropathy: their pattern and prevalence at initial examination. Arch Ophthalmol. 2005;123(11):1554-62. 4. Wilhelm H, Schabet M. The diagnosis and treatment of optic neuritis. Dtsch Arztebl Int. 2015;112(37):616-26. 5. Hayreh SS, Zimmerman MB. Non-arteritic anterior ischemic optic neuropathy: role of systemic corticosteroid therapy. Graefes Arch Clin Exp Ophthalmol. 2008;246(7):1029-46. |

