 |
|
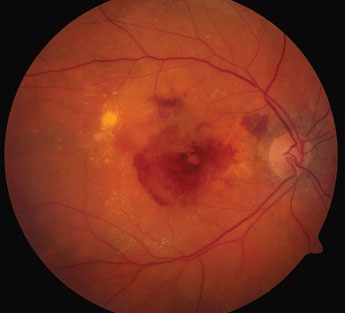
AMD disease activity can be monitored through 3D retinal OCT scans that highlight affected areas. Image courtesy of National Eye Institute/NIH. Click image to enlarge. |
By now, it’s commonplace to hear that artificial intelligence (AI) continues to expand its footprint in healthcare, with studies consistently finding that it provides disease screening capabilities that meet or even exceed traditional human analysis. But when will such efforts strike pay-dirt for clinicians in practice? Looking into its utility in eyecare, an upcoming study currently enrolling patients with wet AMD plans to explore AI’s clinical value in monitoring disease status and influencing personalized treatment decisions by clinicians in real time during the office visit.
The RAZORBILL study will investigate the impact of advanced AI segmentation algorithms on AMD disease activity through “AI-enriched” 3D retinal OCT scans that have automated fluid and layer quantification measurement capabilities. These multidimensional images could show volumes of fluid by highlighting the affected areas within the scans.
“This volumetric information is potentially of high clinical value as it describes precisely and quantitatively the fluid status, which is known to be one of the cornerstones of disease activity evaluation,” the researchers wrote in their paper.
This approach could provide a faster and more sensitive identification of disease activity, which could offer better differentiation and help in decision-making when it comes to treatment, particularly in less specialized centers, the authors suggested.
The study will use Discovery (RetinAI Medical AG), an ophthalmology image management platform embedded with advanced AI technology for analyzing and enriching 3D OCT scans.
“The system will detect, identify, highlight and quantify pathological fluid compartments associated with neovascular lesion activity to the treating physician in real time,” the researchers wrote.
The investigation will enroll 720 patients with wet AMD who are either treatment-naive or are currently using aflibercept, brolucizumab or ranibizumab. Patients will be enrolled in approximately 20 centers across five countries—Canada, Germany, Ireland, Italy and Spain. The observation and data collection period will last 12 months.
The study will be conducted in two phases:
Clinical data collection (Phase I): The observational study design will not enforce strict visit schedules or mandated treatment regimens and was chosen as an appropriate design to collect data in a real-world clinical setting to enable evaluation in the second phase.
OCT enrichment analysis (Phase II): De-identified 3D OCT scans will be evaluated for disease activity. Within this evaluation, the investigators will review the scans once enriched with segmentation results (highlighted and quantified pathological fluid volumes) and once in their original state. This review will be performed using an integrated crossover design, where investigators will act as their own controls, allowing the analysis to account for differences in expertise and individual disease activity definitions.
“With RAZORBILL, we aim to understand and evaluate the added value that AI-based enrichment of OCT images will bring to the task of disease activity assessment,” the researchers wrote. “Additionally, the study will provide essential information on the feasibility and applicability of the AI tool in the clinical practice setting.”
Holz FG, Abreu-Gonzalez R, Bandello F, et al. Does real-time artificial intelligence-based visual pathology enhancement of three-dimensional optical coherence tomography scans optimize treatment decision in patients with nAMD? Rationale and design of the RAZORBILL study. Br J Ophthalmol. August 6, 2021. [Epub ahead of print]. |


