 |
|
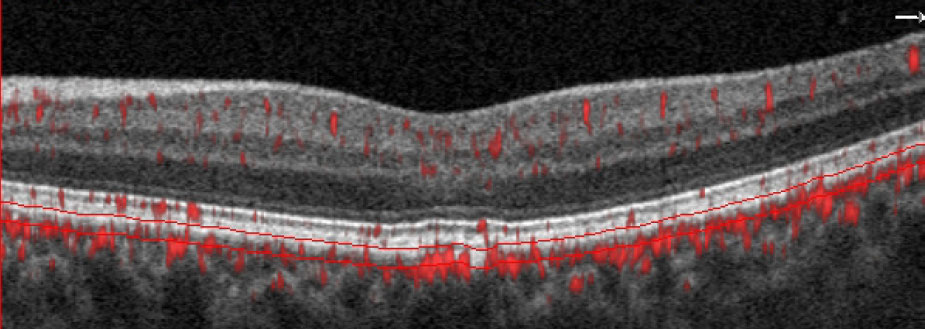
OCT-A imaging is revealing more about choriocapillaris function and its earliest presentations of disease. Shown here is a glaucoma suspect with no visible abnormality on fundus exam. However, B-scan with segmentation lines set at the choriocapillaris depict a non-exudative occult choroidal neovascular membrane. Image courtesy of Julie Rodman, OD. Click image to enlarge. |
Studies have noted that flow deficits in the choriocapillaris—the choroidal layer that nourishes the retinal pigment epithelium and photoreceptors—have been correlated with decreased macular function in age-related macular degeneration (AMD) patients. In addition, rates of geographic atrophy (GA) secondary to AMD have been correlated to the percentage and size of global choriocapillaris flow deficits, leading researchers to conclude that regions of the retina with flow deficits could help predict the likelihood of GA expansion.
One accompanying side effect of flow deficits in eyes with GA is overlying cone photoreceptor loss in the area of the deficit. Cone structure, however, is relatively preserved compared with choriocapillaris flow. “It’s unknown whether the relatively preserved cones in regions of the choriocapillaris flow deficit may have had reduced visual function,” researchers pointed out in a paper published in the American Journal of Ophthalmology. They hypothesized that localized choriocapillaris flow deficits are correlated with retinal sensitivity in GA eyes.
To test this, the researchers launched a cross-sectional, single-center study in which they imaged choriocapillaris flow using 6mm x 6mm swept-source OCT-A and fundus-guided microperimetry to measure retinal sensitivity in the central 20° of their study subjects. They imaged 18 eyes of 12 subjects with GA secondary to non-exudative AMD and seven eyes of four normal subjects and divided their OCT-A scans into a grid. Their microperimetry results were superimposed onto the OCT-A grid using retinal vascular landmarks.
The researchers noted that choriocapillaris flow deficit was significantly greater in the eyes with GA than those without. Retinal sensitivity was significantly lower in GA eyes. They reported that in eyes with GA, choriocapillaris flow deficit decreased and retinal sensitivity increased with distance from the GA margin.
“Choriocapillaris flow deficits inversely correlated with retinal sensitivity,” the investigators stated. “These results suggest decreased choriocapillaris perfusion is associated with photoreceptor dysfunction in eyes with GA. Furthermore, increased flow deficit percentages and reduced retinal sensitivity at the margin of GA suggest that reduced choriocapillaris perfusion and macular dysfunction accompany GA, even outside the border of the individual lesions.”
They noted that further investigation is needed to better understand how the choriocapillaris and photoreceptors affect the development or progression of GA. “Segmentation of structural OCT layers may demonstrate reductions in outer segment or retinal pigment epithelium layer thickness that accompany the abnormalities of retinal sensitivity and choriocapillaris flow we observed beyond the GA margins,” they said.
Additionally, they noted that eyes with nascent GA or incomplete retinal pigment epithelial and outer retinal atrophy are of particular interest because those are areas most likely to develop photoreceptor dysfunction and GA progression. “Studies in these regions could demonstrate whether choriocapillaris flow deficit or retinal sensitivity is affected earliest, and may shed light on the mechanism of disease progression.”
Rinella NT, Zhou H, Wong J, et al. Correlation between localized choriocapillaris perfusion and macular function in eyes with geographic atrophy. Am J Ophthalmol. August 23, 2021. [Epub ahead of print]. |


