 |
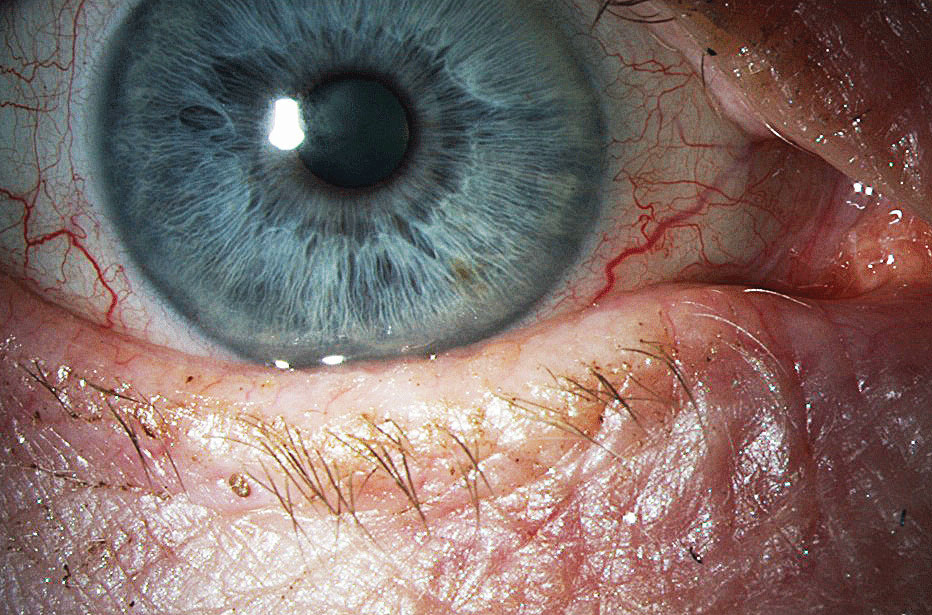
| Excess keratin protein in the meibum can lead to MGD. Photo: Gregory Moore, OD. Click image to enlarge. |
As anyone who’s made an online clothing purchase knows, the color you receive in the mail isn’t always identical to the color you see on your screen. Image appearances can vary widely based on the device and its settings. When it comes to remote diagnostics, many of which rely more and more on smartphones, it’s important to know whether a certain model of phone (i.e., its camera sensor characteristics) or different environmental conditions (e.g., ambient light) will affect the result. That’s the case with traditional methods of smartphone-based cataract detection, such as texture feature analysis, RGB color feature extraction, red reflex method and Gray Level Co-occurrence Matrix method, researchers recently explained in a paper. Their study reported a novel luminance-based eye image analysis technique, which they say, “Copes with different smartphone camera sensors and chroma variations, while operating independently from sensors’ color characteristics and changes in distances and camera angle.”
There are three types of cataract according to the WHO (nuclear sclerotic, cortical spoking and posterior subcapsular) that are defined and graded by examining the opacities. Smartphone applications for detecting cataract rely on lens color and texture features, but as noted before, the color-based methods they use aren’t universally applicable to different devices.
The researchers devised a luminance-based method, which they noted was shown to improve detection accuracy and feature extraction compared with color-based methods in a study comparing the two strategies to detect cancer cells in leukemia. The luminance-based method had 86.67% accuracy and the color-based method had 33.4% accuracy. Overall, the luminance-based method yielded a 17% increase in accuracy over the color-based method.
The researchers wrote in their paper that their novel luminance-based method detects cataract “using pixel brightness transformation to extract luminance values of images acquired with a smartphone camera. To validate the method, we used different iPhone models (iPhone 6, iPhone X and iPhone 11 Pro) to capture images in different light, distance and angle conditions using an eye model. The luminance-based images were then cropped and transformed using the watershed transformation algorithm to extract the region of interest.”
Additionally, they used a Support Vector Machine classifier to distinguish healthy eyes from those with cataract. They used a 10-fold cross validation resampling procedure to evaluate their machine learning model in order to overcome the small data sample size. “As a result, the proposed method detects cataracts from images captured by the smartphone camera,” they explained. “The proposed method only differentiates healthy eyes from diseased eyes, and it doesn’t differentiate between types of cataracts.”
The researchers reported in their paper that their luminance-based method could diagnose diseased eyes with 96.6% accuracy, 93.4% specificity and 93.75% sensitivity. “This method can be used for bedside, clinical and community applications, which are the main pillars of translational medicine,” they wrote. “We’ve implemented our method using different smartphone camera pictures from 100 eye models, of which 50 were cataracts and 50 were healthy. Images were acquired from the eye models emulated to replicate different types of cataract disease and healthy eyes. Our proposed method aimed to find cloudiness and blurriness as signs of cataracts in the eye model.” They tested the model using different distances, ambient light and camera angles. “To improve the performance of our proposed model, a median filter was adopted for pre-processing, and a watershed algorithm was used to enhance luminance features and extract noise and glare.”
Their results showed that “changing environmental factors had a very limited impact (average: 2.8%) on the outcome results. Alternating camera distance, smartphone and camera angle had 3.3%, 3% and 2.2% impact, respectively, on the outcome results, which was negligible.” In addition, they say their method is able to detect the mildest cataracts or lens anomalies because it precisely measures any light reflection. This aids in monitoring progression, they added.
They concluded that their experimental results show that the method can accurately detect cataracts from different distances, smartphones and camera angles. “We can implement our method on any smartphone, including iOS or Android phones, with adequate hardware using a retargetable application platform,” they said.
1. Gupta PK, Periman LM, Lain E, et al. Meibomian gland dysfunction: a dermatological perspective on pathogenesis and treatment outlook. Clin Ophthalmol. 2021;15:4399-404. |


