
A
weekly e-journal by Art Epstein, OD, FAAO
Off the Cuff: How Managed Care Led to Unmanageable Despair
“Death panels” were a hot topic during the run up to Obamacare. The right warned about them, while the left reassured that death panels didn’t exist and never would. What most of us didn’t notice, hiding behind more palatable names, like claims review and prior authorization, was that death panels do very much exist. If you doubt me, take a moment to listen and read this article from CNN. Call it what you will, but what this poor young woman faced, and likely will continue to face, is very much a death panel.
|
|||||
|
|||
| Optical Coherence Tomography Retinal Nerve Fiber Layer Analysis in Eyes With Long Axial Lengths | ||||
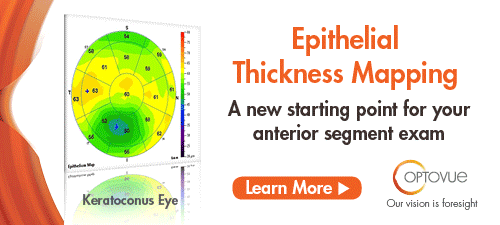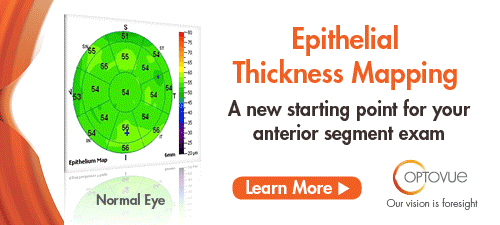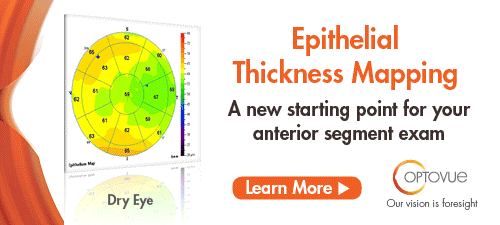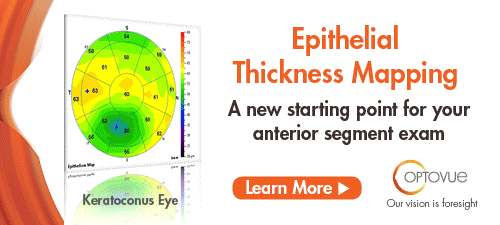
This study evaluated the relationship between axial length (AL) and retinal nerve fiber layer (RNFL) profile and characterized differences in optical coherence tomography RNFL of myopic glaucomatous eyes compared with nonglaucomatous eyes. A retrospective chart review of 170 eyes of 89 subjects with optical biometry and optical coherence tomography RNFL assessment was conducted. Temporal RNFL thickness showed no association with AL in either glaucomatous or nonglaucomatous eyes. Nasal thinning was most strongly associated with glaucoma in myopic eyes. Both myopic glaucomatous and nonglaucomatous eyes had a mean RNFL thickness of 16-22µm thinner than the mean RNFL thickness of normal AL eyes. Researchers concluded that an average of 16 µm to 22µm thinning of RNFL compared with nomogram could be tolerated in patients with long AL. They added that prominent nasal thinning likely represented changes from axial elongation. Temporal RNFL thinning in those with long AL tended to be mild, and, as such, researchers wrote, significant thinning should raise suspicion for glaucoma. |
||||
SOURCE: Patel SB, Reddy N, Lin X, et al. Optical coherence tomography retinal nerve fiber layer analysis in eyes with long axial lengths. Clin Ophthalmol. 2018;12:827-832. |
||||
 |
||
| Evidence for an Association between Macular Degeneration and Thyroid Cancer in the Aged Population | ||||
Investigators wrote that direct evidence of whether thyroid cancer patients have a higher risk of age-related macular degeneration (AMD) has yet to be investigated. Patients older than 50 years-old and newly diagnosed with thyroid cancer between 2000 and 2008 were identified from the national health insurance research database (NHIRD). Investigators applied time-varying Cox proportional hazard models to assess the association between thyroid cancer and AMD. The multivariable models included conventional cardiovascular risk factors, myopia, vitreous floaters, hypothyroidism, hyperthyroidism and treatment modality of thyroid cancer. The analysis process was stratified by age, gender and comorbidity.
In this study, 5,253 patients were included in a thyroid cancer cohort (men 24.5%; median age 59.1 years (53.7 to 67.4 years), and 21,012 matched controls were included in a non-thyroid cancer cohort. The AMD incidence was 40.7 per 10,000 person/years in the thyroid cancer cohort. The thyroid cancer cohort had a higher risk (adjusted hazard ratio (aHR)=1.38, 95% confidence interval, CI=1.09 to 1.75) of AMD than the non-thyroid cohort. Thyroid cancer patients had a higher risk of AMD, especially the male patients (aHR=1.92, 95% CI=1.38 to 3.14) and the patients with comorbidities (aHR=1.38, 95% CI=1.09 to 1.74). Investigators found that thyroid cancer patients older than 50 years-old had an increased risk of AMD. |
||||
SOURCE: Lin SY, Hsu WH, Lin CL, et al. Evidence for an association between macular degeneration and thyroid cancer in the aged population. Int J Environ Res Public Health. 2018;15(5). |
||||
| Risk of Glaucoma Surgery after Corneal Transplant Surgery in Medicare Patients | ||||
Glaucoma is a well-documented complication of corneal transplants, contributing significantly to ultimate visual loss. Authors wrote that reported incidence of glaucoma following corneal transplants is highly variable, and definitions of post-transplant glaucoma are inconsistent. Here, they used glaucoma surgery as a more rigid and specific endpoint to compare rates following different corneal transplant surgeries.
They used a 5% random sample of Medicare beneficiaries from 2010 to 2013. Patients were identified by Current Procedural Terminology (CPT) codes for penetrating keratoplasty (PK), endothelial keratoplasty (EK), anterior lamellar keratoplasty (ALK) and keratoprosthesis (KPro). Rates of glaucoma surgery within the same year following the abovementioned corneal transplants were analyzed. Subgroup analyses included patients who carried preexisting glaucoma diagnoses prior to corneal transplant surgery. There were 3,098 patients who underwent corneal transplants during the study period, including 1,919 EK, 1,012 PK, 46 ALK, 32 KPro, and 89 PK and EK. Rates of glaucoma surgery ranged from 6.1% to 9.4% in the corneal transplant groups, without statistically significant differences among groups. However, 10% of patients with preexisting glaucoma required glaucoma surgery following any transplant surgery, compared with 5.3% of patients without preexisting glaucoma. This included 12.4% of PK patients with preexisting glaucoma compared with 2.8% of PK patients without preexisting glaucoma (p<0.01). Despite the literature suggesting that more angle-altering cornea surgeries conferred higher risk, the authors found no statistically significant differences among various transplant groups. Patients with preexisting glaucoma, however, had a higher risk of glaucoma surgery within the same year following corneal transplant surgery, which was especially pronounced in the PK group. Consequently, the authors wrote, these patients require special care when considering long-term effects of corneal transplants. |
||||
SOURCE: Zheng C, Yu F, Tseng VL, et al. Risk of glaucoma surgery after corneal transplant surgery in medicare patients. Am J Ophthalmol. 2018; May 12. [Epub ahead of print]. |
||||
 |
||
| News & Notes | |
| American Academy of Optometry Launches Online CE Platform The American Academy of Optometry introduced Academy Online—an online CE and resource platform. There, users can find a collection of session recordings from past annual meetings as well as distance learning credits. Content can be viewed at any time using any device with online access. Content highlights include video footage of the 2016 Plenary Session featuring world-renowned author and speaker Malcolm Gladwell and other popular sessions from Academy 2017 Chicago. Users can also browse posters from the 2016 Scientific Program and interact with presenters via discussion threads. Academy members have complimentary access to Academy Online, and non-members can access the content for a fee. Learn more. |
|
| Study Compares Accuracy of Subjective Refraction Using Vmax Vision's VASR vs. Traditional Refraction In a comparison study, reported at ARVO 2018 and conducted by researchers at the Southern College of Optometry, 50 healthy subjects were examined by a masked investigator using a standard autorefractor (Nidek TonoRef II) followed by subjective refinement using a standard phoropter (monocular subjective refraction with binocular balance). Subjective measurements were also conducted in the corresponding subjects using a Voice Activ Subjective Refractor (VASR) by Vmax Vision. For spherocylindrical refractive error, the results obtained with the Vmax VASR by a second-year optometry student with two hours of training were not statistically different from those achieved by an SCO optometrist and faculty member using traditional phoropter methods. The researchers determined that training requirements to refract with the VASR were substantially easier than those to use a phoropter. |
|
|
|
|
Optometric Physician™ (OP) newsletter is owned and published by Dr. Arthur Epstein. It is distributed by the Review Group, a Division of Jobson Medical Information LLC (JMI), 11 Campus Boulevard, Newtown Square, PA 19073. HOW TO ADVERTISE |


