| |
Volume 14, Number 1 |
April
2018 |
|
|
Inside
This Issue |
|
|
|
|
|
This e-newsletter is provided free to doctors through industry support from |
 |
| |
FROM
THE DESK OF THE EDITOR
Last week, I had a 56-year-old patient who had earlier presented with acute non-arteritic ischemic optic neuropathy (NAION). He came in a week prior immediately at the onset of his symptoms, but returned because his vision and visual field had further deteriorated. The kicker was that this wasn’t the first time. He had developed NAION three years prior in his other eye. So now, all of a sudden, this poor gentleman went from functional vision to non-functional vision literally overnight as his blood pressure got too low to adequately perfuse the optic nerve. He was now missing 50% of his visual field in each eye and his binocular acuity went from 20/20 to 20/70. This is the clinical scenario that I dread most. We talked about the chance that his vision could improve, but it could also stay the same or even worsen. The worst part was that I had no treatment options to give him. We were already in the process of arranging a sleep study to rule out undiagnosed sleep apnea. We talked about trying high-dose oral steroids, and the fact that this is extremely controversial. Ultimately, I had to put myself in his shoes. Knowing what I know, would I give this a try? After a long discussion about unproven therapy and the side effects that accompany high doses of oral steroid, we decided to go that route. Would I rather give him zero treatment choices or the small hope of an unproven option?
The clinical scenario that I would much rather be in is to tell a patient that has already suffered from longstanding vision loss that there is new hope for improvement. Please take a look at the article in the journal abstract section by Dr. Brad Sutton about a recently FDA-approved gene therapy for individuals with a very specific type of Leber’s congenital amaurosis or retinitis pigmentosa. This marks the first FDA approval for gene therapy for a genetic disease. It is a promising development that renews my sense of optimism. We’re all going to be in a position sometimes to give bad news to patients. So the opportunity to give hope to patients who previously did not have any is exciting.
Anna Bedwell, OD, FAAO
Editor-in-Chief
PRESIDENT'S MESSAGE
A recent study (JAMA Ophthlamol 2017:135(6):57-575) revealed that 25% of eyes deemed normal on a dilated eye examination by primary care physicians (either optometrist or ophthalmologist) were found to have AMD on fundus photos reviewed by trained raters. Further, of these with undiagnosed AMD, 30% had large drusen that probably should be on nutritional supplementation. To me, that means that we are really not doing as good of a job recognizing and diagnosing AMD as we should be. As optometrists, we are deathly afraid of missing a single glaucoma patient, putting even the most unlikely suspect through an extensive battery of tests, yet we dismiss AMD so quickly with only a glance at the posterior pole. I would argue that before we had treatments, such as nutritional supplements to slow the progression in patients with intermediate or worse dry AMD, or anti-VEGF injection in our wet AMD patients, it probably was irrelevant if we missed the diagnosis. But now, it is even more imperative, and we must do better. We now have new tools in our toolbox, such as OCT, OCTA, dark adaptation, macular pigment optical density, better and wider fundus cameras and genetic testing (and so on) to aid us in our diagnosis and management of patients with AMD. There is really no reason that we should be doing such a poor job. So, like the quote from one of my favorite comic book books and later Marvel movie states, “With great power comes great responsibility” (Spider-Man, Amazing Fantasy, Aug. 1962). We have the power to help patients with AMD get appropriate treatment and help maintain their vision, and it is our responsibility to do so. Diagnosing AMD is the first step!
Sincerely,
Steven Ferrucci, OD, FAAO
ORS President

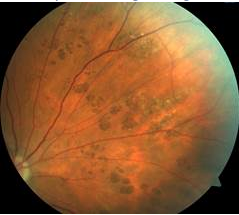
Do you think bear tracks (like in the image shown below) have an association with colon polyps and/or colon cancer?
|
IN MEMORY
It is with a heavy heart that I share the awful news that Gay K. Tokumaru, OD, FAAO, ORS Fellow, passed away after a battle with cancer. Gay was Chief of Optometry at the Hampton VA Hospital in Virginia for many years. She contributed to the profession in multiple ways, such as through the Education Committee of the American Academy of Optometry as well as the Advanced Competency in Medical Optometry Committee, where I has the pleasure of serving with her. Beyond her dedication to the profession, she was also a caring individual, trusted colleague, and friend to many of us. She will be missed not only by us that knew her as a friend and colleague, but certainly by her family, friends and many patients.
https://www.dignitymemorial.com/obituaries/williamsburg-va/gay-bessen-7786660
Steven Ferrucci, OD, FAAO
ORS President
YOU
MAKE THE DIAGNOSIS
Answer appears later in newsletter.
Figure 1.
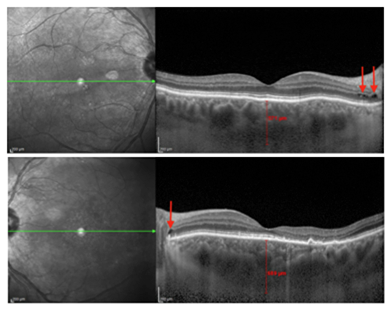
Figure 2.
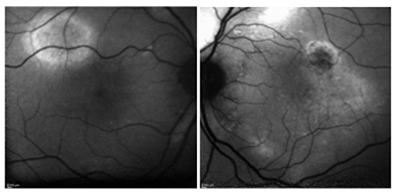
Figure 3.
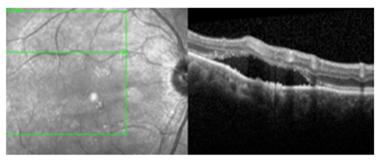
Figure 4.

Figure 5.
|
Answer appears later in newsletter.

Image Gallery
Which of the following images represents a traumatic choroidal rupture?
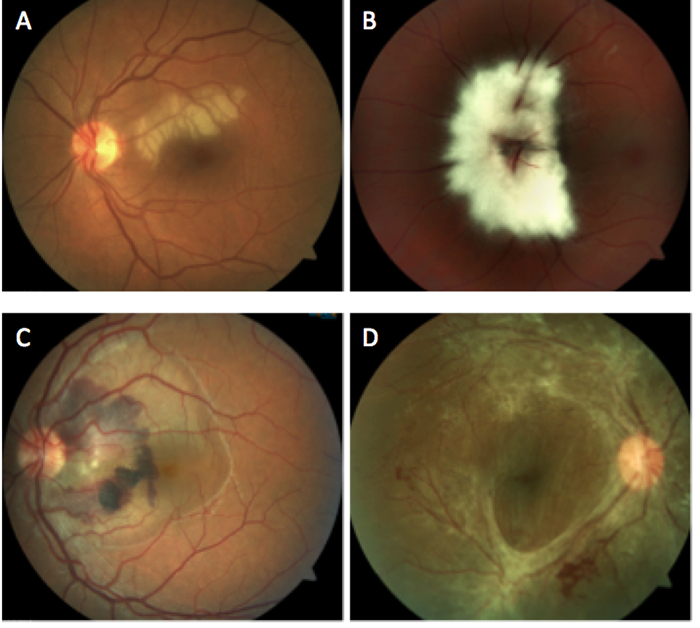
Answer appears later in the newsletter.
|

JOURNAL
ABSTRACTS
Central Macular Thickness in 6.5-year-old Children Born Extremely Preterm is Strongly Associated with Gestational Age Even When Adjusted for Risk Factors
Preterm birth is an already known risk factor for abnormal macular development. Extremely preterm (EPT) births are on the rise due to better medical advancement. This study compared the macular thickness of 6.5-year-old children born EPT with children born at term.
The study group was made up of 6.5-year-old children born before 27 weeks gestational age-matched to normal children born at term of gestational age ≥37 weeks. The children were born in counties in Sweden between 2004 and 2007. The EPT group was screened for retinopathy of prematurity (ROP) and staged according to guidelines set by the International Committee for the Classification of Retinopathy of Prematurity. The children all had comprehensive examinations including VA with LogMAR Lea symbols, cycloplegic autorefraction and Cirrus OCT macular cube (512 x 128). To be deemed acceptable, the OCTs had to have the fovea centered, correct segmentation, signal strength ≥, no detectable blink or eye movement artifact.
A total of 134 of the children born EPT and 145 of the controls had acceptable OCT images (one or both eyes) to be included in analysis. As expected, there was a significant difference in visual acuity between the EPT group and the controls. In comparison with the ETDRS areas of the OCT macular cube, the EPT group had a significantly thicker central macula with an average difference of 34.4 μm (p<0.001). There were no significant differences between the groups in the inner and outer ETDRS circles. Potential risk factors were calculated using a simple linear mixed model in the EPT group. The associations found statistically significant included gestational age (p=0.009), body weight (p=0.037), ROP (p=0.002) and male gender (p=0.008) compared with central macular thickness.
This study found that EPT birth, as well as low GA and ROP (regardless of stage or treatment), are important risk factors for a thick central macula. Other studies have demonstrated that a thicker central macula in prematurity is caused by incomplete migration of the inner retinal layers, thus, resulting in a thicker central macula. This study provides additional insight in understanding the macular development in this particular pediatric population.
Molnar AEC, Rosén RM, Nilsson M et al. Central macular thickness in 6.5-year-old children born extremely preterm is strongly associated with gestational age even when adjusted for risk factors.
Retina. 2017;37(12):2281-8.
Cuticular Drusen: Clinical Phenotypes and Natural History Defined Using Multimodal Imaging
Cuticular drusen are classified as small, round drusen located sub-RPE that develop in early adulthood. There is less understanding of cuticular drusen in comparison with hard and soft drusen. This retrospective study monitored the life cycle, variation and complications of cuticular drusen phenotypes via multimodal imaging.
A total of 266 eyes with cuticular drusen were examined from four different locations across the world. To be included, eyes had to display characteristics of cuticular drusen in three of four imaging modalities: multiple yellow, uniform, round sub-RPE accumulations in photos, sub-RPE location on OCT, starry-sky appearance on FA and drusen with central hypofluorescence with a hyperfluorescent edge on FAF. Of 266 eyes, 240 met the criteria for cuticular drusen. The observers looked at the location of the drusen, natural course over >5 year follow up (disappearance, coalescence, new pigmentary abnormalities) and complications (neovascularization, GA, AVL–acquired vitelliform lesion).
The natural course (over >5 year follow up) showed that cuticular drusen disappeared in 58.3% of eyes, coalesced in 70.8% and developed new pigmentary abnormalities in 56.2%. Complications occurred more often in patients older than 60. Across all eyes, RPE abnormalities occurred most often (47.5%), followed by GA (25%), AVL (24.2%) and neovascularization (12.5%).
The authors suggested that the structural findings in cuticular drusen seemed akin to hard drusen, while the natural course and risk of complication was more similar to soft drusen. This stressed the importance of multimodal imaging to classify drusen phenotype. Ultimately, further investigation is warranted to understand how cuticular drusen phenotypes differ from classic AMD.
Balaratnasingam C, Cherepanoff S, Dolz-Marco R, et al. Cuticular Drusen: Clinical phenotypes and natural history defined using multimodal imaging. Ophthalmology. 2018 Jan;125(1):100-18.
Subfoveal Choroidal Thickness Predicts Macular Atrophy in Age-Related Macular Degeneration: Results from the TREX-AMD Trial
The TREX-AMD trial, an ongoing, multicenter, randomized, controlled clinical trial, has the primary objective of comparing monthly dosing vs. treat-and-extend (TREX) dosing of intravitreal ranibizumab in treatment-naïve neovascular AMD (nAMD). In this particular report, the development of macular atrophy (MA) was studied.
This study included 60 patients with treatment-naïve nAMD in at least one eye. Eyes were not included if they did not reach 18 months follow-up, had poor-quality OCT images, or MA beyond the scanning fields of the FAF picture or SDOCT. Eighty-eight eyes of 52 patients fit this criteria; of those eyes, 33 had dry AMD and 55 had nAMD. To be defined as MA, there had to be 125 microns of thinning to the RPE band, with loss of the ellipsoid zone and external limiting membrane, and increased signal transmission into the choroid. At the foveal center, subfoveal center thickness (SCT) was measured from Bruch’s membrane to the inner surface of the sclera.
In the dry AMD group (early or intermediate), 15 eyes had MA while 18 eyes had dry AMD without MA. There was a statistically significant (p=0.04) difference in mean SCT between the groups (group without MA 169.8 ±65.1 μm and group with MA 129.3 ±40.8 μm). In the nAMD group, 23 eyes had CNV and MA, and 32 had only CNV. Again, the eyes with MA and CNV had a much thinner average SCT (p=0.01). The eyes with only CNV had a SCT of 174.2 ±57.0 μm and those with both CNV and MA had an SCT of 133.2 ± 57.9 μm. Comparing the MA vs. non-MA groups, there were no significant differences in age or sex. Interestingly, there was no significant difference between the dry AMD group and nAMD group in terms of baseline SCT.
Six additional eyes in the nAMD group developed MA during the 18-month follow-up. The difference in SCT between those that developed MA (125.7 μm) and those that did not (185.4 μm) was statistically significant (p=0.03). Their analysis found a 4.3x higher risk for development of MA with a SCT of ≤124 μm.
In summary, the authors found AMD eyes with MA were more likely to have a thinner SCT. The relationship between the choroid and development of MA certainly necessitates further investigation. Although anti-VEGF is highly effective for nAMD, there is no treatment or prevention for atrophy in AMD.
Fan W, Abdelfattah NS, Uji A, et al. Subfoveal choroidal thickness predicts macular atrophy in age-related macular degeneration: results from the TREX-AMD trial. Graefes Arch Clin Exp Ophthalmol. 2018; Jan 27. doi: 10.1007/s00417-017-3888-2. [Epub ahead of print]
Changes in Plasma Vascular Endothelial Growth Factor Level after Intravitreal Injection of Bevacizumab, Aflibercept, or Ranibizumab for Diabetic Macular Edema
Vascular endothelial growth factor (VEGF) is associated with diabetic macular edema (DME) and the progression of non-proliferative diabetic retinopathy (NPDR) to proliferative diabetic retinopathy (PDR). VEGF may reach retinal vasculature through intraocular fluid or systemic circulation as plasma VEGF. Prior research has shown that intraocular VEGF correlates with DME and diabetic retinopathy (DR) severity, whereas the correlation between plasma VEGF and DME status has not been investigated.
This prospective study investigated the role of plasma VEGF with DME and DR progression. Plasma VEGF levels were evaluated in 72 patients with DME receiving intravitreal injections of bevacizumab, aflibercept, or ranibizumab. The control group consisted of 17 patients without DR or DME who underwent cataract surgery. At baseline, there was no significant difference in plasma VEGF levels in patients with DME vs. age-matched controls. After a single anti-VEGF injection, bevacizumab and aflibercept showed significant suppression of plasma VEGF levels at 1 week and 4 weeks after the injection. Plasma VEGF levels after injection of ranibizumab remained unchanged at one and four weeks. This is likely due to the short two-hour systemic half-life of ranibizumab, whereas aflibercept has a half-life of five days and bevacizumab’s half-life is 20 days. Central subfield macular thickness was significantly reduced from baseline in all three test groups. Best-corrected visual acuity improved in all three groups at week one, but only aflibercept achieved significant vision improvement at week four. There was no significant relationship found between plasma VEGF levels and DR or DME severity.
The results of this study showed that plasma VEGF suppression was not necessary in the treatment of DR or DME with intravitreal anti-VEGF injections, as plasma VEGF levels were unrelated to DR and DME severity. Because of the limited sample size and single-center setting, researchers suggested that further studies are warranted.
Hirano T, Toriyama Y, Iesato Y, et al. Changes in plasma vascular endothelial growth factor level after intravitreal injection of bevacizumab, aflibercept, or ranibizumab for diabetic macular edema. Retina. 2017; Dec 21. doi: 10.1097/IAE.0000000000002004. [Epub ahead of print].
The Real-World Effect of Intravitreous Anti-Vascular Endothelial Growth Factor Drugs on Intraocular Pressure
Anti-vascular endothelial growth factor (anti-VEGF) prevents VEGF from binding to VEGF receptors, thus preventing neovascularization and limiting vascular permeability. Anti-VEGF injections have proven to be effective in treating several conditions such as neovascular age-related macular degeneration (AMD), diabetic macular edema (DME) and macular edema after retinal vein occlusions. A sharp increase with a relatively quick decrease in IOP is known to occur directly after an intravitreal injection; however, the long-term effect on IOP is in question. The goal of this study was to examine sustained effects of anti-VEGF agents on IOP.
This database study looked at 23,776 patients in the American Academy of Ophthalmology Intelligent Research in Sight (IRIS) Registry who received a single type of anti-VEGF injection (bevacizumab, aflibercept, or ranibizumab) into the right eye with a diagnosis of AMD or macular edema due to diabetes or retinal vein occlusion between January 1, 2013, and December 31, 2015. Exclusion criteria included eyes that received more than one type of anti-VEGF agent, an injection in the fellow eye and/or an intravitreal corticosteroid injection. All patients receiving anti-VEGF injections for more than one year showed a statistically significant but small decrease in IOP from baseline with a mean of 0.9 mmHg in treated eyes vs. 0.2 mmHg in fellow untreated eyes. Bevacizumab was associated with a smaller decrease in IOP than aflibercept and ranibizumab when accounting for confounders in a generalized linear model. Those with an IOP increase of 6 mmHg or more resulting in an absolute IOP of more than 21 mmHg (termed clinically significant IOP rise) were 2.6% overall vs. 1.5% of fellow untreated eyes. Of the three anti-VEGF agents, aflibercept was less likely to increase IOP when compared with bevacizumab and ranibizumab. Three times more patients who experienced a clinically significant IOP rise had a pre-existing diagnosis of glaucoma. Further studies are needed to determine glaucoma risk or progression in patients receiving anti-VEGF injections. Overall, the results from real-world data showed that anti-VEGF injections were associated with a small decrease in IOP over time.
Atchison EA, Wood KM, Mattox CG, et al. The real-world effect of intravitreous anti-vascular endothelial growth factor drugs on intraocular pressure. Ophthalmology. 2018; Jan 11. pii: S0161-6420(17)31512-9. doi: 10.1016/j.ophtha.2017.11.027. [Epub ahead of print].
Follow-Up to Gene Therapy in Retinal Disease
In the last issue of the ORS Newsletter, we discussed a novel gene therapy for a very specific form of inherited retinal disease. As a reminder, this gene therapy (Luxturna) from Spark Therapeutics is designed to treat individuals with a faulty RPE 65 gene. Approximately 8.5 % of patients with Leber’s Congenital Amaurosis (LCA) and up to 2% of patients with retinitis pigmentosa (RP) carry this particular mutated gene. There are believed to be around 2,000 individuals in the United States with this mutation. At the time the prior article was written, Luxturna had not yet received full FDA approval. Recently, it received that clearance, so we now have the first gene therapy available to treat an ocular condition. Via intraocular injection, a viral vector is utilized to carry a healthy copy of the RPE 65 gene to the target tissue. It was widely expected that the therapy would be very expensive, and that has certainly proven to be the case. It is initially being priced at $850,000.00, $425,000.00 per eye, which is actually less than the $1,000,000.00 that many analysts had predicted. The combination of extensive research and development costs, the one-time nature of the treatment and the very small number of potential recipients necessitates this hefty price tag. Spark understands the barriers that this creates, and is working with insurers to develop effective mitigation strategies. These include offering the option to pay for the therapy via installment payments made over time, and offering a partial refund if the therapy proves not to be effective for a given individual. The idea of paying via installments is an intriguing one, but it is likely to be complicated by the fact that patients often switch insurance carriers rather frequently over time. Originally, Spark was offering free genetic testing through Prevention Genetics that was capable of identifying a sizeable number of rod-mediated inherited retinal disorders. That program has been discontinued, but the free testing is still available to check only for the presence of a faulty RPE 65 gene. In patients with LCA or RP, performing this test will allow an individual to know if they are a candidate for Luxturna treatment or if they are not. Any eye care practitioner interested in more information regarding obtaining the in-office test kits can call 855-772-7589. We live in an era of astounding technological advancements in health care. While Luxturna is the first true gene therapy approved for an ocular condition, it won’t be the last.
Brad Sutton, OD, FAAO
Immediate Past President, Optometric Retina Society

|
ANSWER
TO "YOU MAKE THE DIAGNOSIS"
Introduction:
Uveal effusion (UE) refers to the abnormal accumulation of fluid into the suprachoroidal space. Literature sources also refer to it as choroidal effusion, ciliochoroidal effusion, ciliochoroidal detachment and choroidal detachment.1 Causes of UE include inflammation (i.e., trauma, scleritis, photocoagulation, uveitis); and hydrostatic conditions (i.e., hypotony, primary-angle closure glaucoma; drug-induced, arterio-venous fistula).1
In 1963 Schepens and Brockhurst acknowledged a specific UE type of unknown cause which formed a definite clinical entity, occurring almost exclusively in males.2 Without signs of inflammation or hydrostatic changes, they used the term uveal effusion syndrome (UES) and considered it a diagnosis of exclusion.1–3
Case Report:
A 59 year-old Caucasian male presented with complaints of a blurred spot in the right eye for two weeks, and in the left eye since cataract surgery in 2012. The blurred spots, which became increasingly noticeable when going from a light to a dark room, were constant and did not change with eye movement. He also reported a generalized decrease in visual acuity OS>OD, and described his vision as if he was looking through water.
BCVA measured 20/20 OD with +1.50 DS, and 20/30+2 OS with +0.75-0.75x090. Chairs skills were unremarkable. Ocular history included pterygium removal OS in 1980. Medical history was positive for hypertension and gout. No medication use was reported. Anterior segment examination revealed nasal corneal scarring consistent with the previous pterygium surgery OS, and PCIOL OU with mild posterior capsular opacification OU. Prior to cataract development, the patient maintained 20/20 vision OD and OS with a refractive error of +3.00 OD and +3.75 OS. Intraocular pressures obtained with Goldmann tonometry were 13 mmHg OD and OS.
Dilated fundus exam results included flat, pink optic nerves with a cup-to-disk ratio of 0.25 round OU. Scattered areas of retinal pigment epithelial (RPE) disruption were noted within the posterior pole OU. Optical coherence tomography B-scans (OCT-B) with enhanced depth imaging (EDI) were obtained along with fundus autofluorescence (FAF) pictures and ultrasound B-scans. Previous ophthalmic visits did not include OCT-B or other imaging and therefore comparable scans were not available for review. Results from earlier dilated fundus examinations ranged from “normal” OU in 2006 to trace macular mottling without edema OU prior to surgery in 2012.
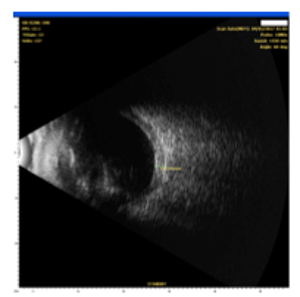
OCT-B EDI scans (Figure 1) demonstrated marked pachychoroid of nearly 600 um OD and 700 um OS. FAF (Figure 2) OD highlighted an area of autofluroescence approximately the size of the macula inside the superior temporal arcade. OCT-B scans of this area confirmed a serous retinal detachment (Figure 3). The more diffuse autofluorescence in the FAF OS included two areas of increased intensity superior and superior-temporal to the optic nerve (exaggerated due to instrument gain amplification). A retinal thickness map of the segmented outer nuclear layer (ONL) OS (Figure 4) illustrated the extensive areas of ONL atrophy. The “hot spot” correlated to a focal retinoschisis. The FAF OS also showed an area absent of autofluorescence about 1 DD superior temporal to the macula. An OCT-B scan through this area revealed outer retina and RPE atrophy. The ultrasound B-scan (Figure 5) exhibited a thickened retina-choroid-sclera complex, but no peripheral choroidal detachments, which correlated to clinical findings. An ultrasound biomicroscopy (UBM) scan was not obtained due to the lack of peripheral choroidal involvement.
Dicussion:
UES is closely related to nanophthalmos or hyperopia and a thick sclera, and is rarely accompanied by significant inflammation.1,6 It results from abnormal trans-scleral diffusion of choroidal extravascular proteins from the suprachoroidal space.3,7 This leads to vortex vein compression and subsequent congestion of choroidal veins.3 Pachychoroid ensues from fluid accumulation, thus setting the stage for ciliochoroidal and non-rhegmatogenous retinal detachments.
In this case, the preoperative refractive error measured +3.00 OD, and +3.75 OS. B-scan ultrasound approximated the retina-choroid-sclera complex thickness to be 2.65 mm. Studies involving scleritis consider a “posterior coating” (i.e., retina-choroid-sclera) value of 2 mm or greater to be thick.8,9 Estimating this patient’s retina and choroid thickness from OCT-B results and removing them from the equation leaves a rough posterior scleral estimate of 2 mm. Normal posterior scleral thickness hovers around 1 mm with a standard deviation of about 0.2 mm.10,11
When UES is confined to the posterior pole, as shown here, the alternative diagnosis PUES applies. Speculation exists as to the mechanism of fluid transfer into the posterior pole. In this patient, the posterior subretinal fluid may have extended from the cystic spaces noted at the optic disk margin (Arrows, Figure 1). This has been reported elsewhere in patients with PUES.4,5 Liu et al postulated that a combination of RPE and photoreceptor loss in the presence of a temporal disk crescent could facilitate the movement of choroidal fluid to the neurosensory retina. This anatomical appearance of a thick peripapillary choroid and disk crescent may present a weak link in the blood-retinal barrier.4 A fluorescein angiogram could pinpoint these areas of peripapillary leakage (this patient declined consent for the procedure).
UES is thought to be extremely rare1,3, and few reports of PUES exist in the literature.4,5 This may be due to a lack of diagnostic acumen. Middle-aged to older patients presenting with pigmentary changes and subretinal fluid may erroneously be diagnosed with exudative macular degeneration. In these cases, the clinician should note the refractive error, image the choroid with OCT-B EDI to evaluate for pachychoroid and perform a B-scan to assess for posterior thickness and nanophthalmos.
The disease may also be confused with central serous chorioretinopathy (CSR) as similar clinical findings, multimodal imaging results and demographics (male predilection) exist. As with this patient, comparable data made CSR a strong diagnostic contender. The lean toward an ultimate PUES diagnosis hinged on several factors.
First, a meta-analysis by Chen et al. found the mean subfoveal choroidal thickness in patients affected by CSR to be 413.1 ± 93.0 μm.12 Using this data, the OD choroidal thickness in this patient would be almost two standard deviations above the mean, while the OS choroidal thickness would be three times above it.
Second, the patient did not exhibit CSR risk factors such as corticosteroid use, Type A personality or other medications associated with the disease. Gender does match for CSR, but his age is above the reported peak years of onset (40 to 45 years for men), though studies vary on this matter.13
Third, the lack of autofluorescence superior temporal to the macula OS may lead one to hypothesize that this area housed the most activity and therefore suffered more damage. Compare this to the OD FAF and the area of interest nearly mirrors the OS FAF location, superior temporal to the macula. Over the course of the disease, bilateral CSR occurs in 20% to 40% of patients.12 However, the non-foveal, nearly symmetrical involvement certainly warrants thought when differentiating PUES from CSR.
Fourth, cataract surgery may exacerbate existing UES.1,4 Pautler and Browning noted this in their publication, and the patient in this case self-reported a blurred spot post-cataract extraction, which would appear to support this correlation. Conversely, the visual change could merely have been the result of greater overall contrast sensitivity, or simply an increase in acuity which allowed for better visual discern.
Finally, the peripapillary cystic spaces OU discovered on OCT were consistent with the fluid leakage theory in PUES proposed by others. All the above combined with the hyperopic status and thickened sclera edged PUES to the more likely diagnosis.
Both UES and PUES are difficult to manage and often follow a relapsing course.6 Full-thickness sclerectomy is the surgical treatment of choice by many for UES, but outcomes are variable.1 In their case of PUES, Pautler and Browning reported effective treatment with oral acetazolamide for the acute stage, with a switch to the topical form for maintenance. They cited a 2009 literature review by Siesky et al., which showed posterior pole effects from topical carbonic anhydrase inhibitor therapy and theorized that since PUES is isolated to the posterior pole, this treatment may increase fluid transport from the subretinal space to the choroid.4 In this case report, the patient declined any treatment and elected to observe the condition. At eight months, some areas of serous retinal detachment improved while others remained relatively stable. The fovea remained flat and intact OU.
Conclusion
UES is rare where uveal effusion and serous retinal detachment are the most characteristic clinical findings.1 It has a middle aged-male predilection, and 65% of cases occur bilaterally.1,3 Uyama et al. categorized UES into three groups initially, but kept only two after the results of their study (Table 1).14 Few cases of PUES have been reported.
Diagnosing UES or PUES necessitates the use of multimodal imaging and expanded critical thinking. Along with the ancillary tests listed above, UBM imaging should also be considered when peripheral choroidal detachment and/or increased intraocular pressure occur. UBM allows the examiner to more clearly depict the anterior ciliary body for thickness changes and rotation. These changes are more common in UE where the anterior choroid has a thickened, spongy or cystic appearance.15 Due to the lack of peripheral involvement, a UBM was not obtained in this case.
Jim Williamson
ORS Fellow
| |
Eyeball |
Axial Length |
Refractive Error |
Sclera (MRI) |
Scleral Status |
Histology |
Surgery |
| Type 1 |
|
Small (<19mm) |
High hyperopia (>12D) |
Thickened |
Thick and Rigid |
Abnormal |
Effective |
| Type 2 |
|
WNL or slightly small (21 mm) |
Small error |
Thickened |
Thick and Rigid |
Abnormal |
Effective |
Table 1. Note that scleral thickness was documented with MRI findings (vs. ultrasound), and scleral status was determined during surgery. Sixteen out of 17 eyes were successfully treated with subscleral sclerectomy. |
Bibliography
1. Elagouz M, Stanescu-Segall D, Jackson TL. Uveal Effusion Syndrome. Surv Ophthalmol. 2010;55(2):134-145. doi:10.1016/j.survophthal.2009.05.003.
2.Schepens C, Brockhurst R. Uveal Effusion: 1. Clinical picture. Arch Ophthalmol. 1963;70:189-201.
3.Abell RG, Kerr NM, Vote BJ. Bilateral nanophthalmic uveal effusion syndrome: Clinical presentation and surgical management. Retin Cases Br Reports. 2013;7(4):386-390. doi:10.1097/ICB.0b013e318297f6c1.
4.Pautler SE, Browning DJ. Isolated posterior uveal effusion: Expanding the spectrum of the uveal effusion syndrome. Clin Ophthalmol. 2014;9:43-49. doi:10.2147/OPTH.S75448.
5.Liu Q, Hemarat K, Kayser DL, Stewart JM. A case of posterior uveal effusion syndrome masquerading as uveitis. Retin Cases Br Reports. 2017;11(1):S124-S127. doi:10.1097/ICB.0000000000000463.
6.Kong M, Kim JH, Kim SJ, Kang SW. Full-thickness sclerotomy for uveal effusion syndrome. Korean J Ophthalmol. 2013;27(4):294-298. doi:10.3341/kjo.2013.27.4.294.
7.Harada T, Machida S, Fujiwara T, Nishida Y, Kurosaka D. Choroidal findings in idiopathic uveal effusion syndrome. Clin Ophthalmol. 2011;5(1):1599-1601. doi:10.2147/OPTH.S26324.
8.Okhravi N, Odufuwa B, McCluskey P, Lightman S. Scleritis. Surv Ophthalmol. 2005;50(4):351-363. doi:10.1016/j.survophthal.2005.04.001.
9.McCluskey PJ, Watson PG, Lightman S, Haybittle J, Restori M, Branley M. Posterior scleritis: clinical features, systemic associations, and outcome in a large series of patients. Ophthalmology. 1999;106(12):2380-2386. doi:10.1016/s0161-6420(99)90543-2.
10.Norman RE, Flanagan JG, Rausch SMK, et al. Dimensions of the human sclera: Thickness measurement and regional changes with axial length. Exp Eye Res. 2010;90(2):277-284. doi:https://doi.org/10.1016/j.exer.2009.11.001.
11.Vurgese S, Panda-Jonas S, Jonas JB. Scleral Thickness in Human Eyes. Vavvas D, ed. PLoS One. 2012;7(1):e29692. doi:10.1371/journal.pone.0029692.
12. Chen G, Tzekov R, Li W, Jiang F, Mao S, Tong Y. Subfoveal choroidal thickness in central serous chorioretinopathy: A meta-Analysis. PLoS One. 2017;12(1):1-13. doi:10.1371/journal.pone.0169152.
13. Liegl R, Ulbig MW. Central serous chorioretinopathy. Ophthalmologica. 2014;232(2):65-76. doi:10.1159/000360014.
14.Uyama M, Takahashi K, Kozaki J, et al. Uveal effusion syndrome: Clinical features, surgical treatment, histologic examination of the sclera, and pathophysiology. Ophthalmology. 2000;107(3):441-449. doi:10.1016/S0161-6420(99)00141-4.
15.Shah PR, Yohendran J, Hunyor AP, Grigg JR, McCluskey PJ. Uveal Effusion. J Glaucoma. 2016;25(4):e329-e335. doi:10.1097/IJG.0000000000000329.
|

IN THE
NEWS
 |
Topcon's DRI OCT Triton Series Receives 510(k) Clearance
In January 2018 Topcon Medical Systems announced that its Deep Retinal Imaging (DRI) OCT Triton Series has obtained 510(k) clearance from the FDA. The DRI OCT Triton is a multimodal instrument with capabilities of color, red-free, FA and FAF imaging with Swept Source OCT/OCTA. The instrument has a 1 micron, 1,050 nm light source and scanning speed of 100,000 A-scans/sec. Topcon notes that the DRI OCT Triton is not hindered by media opacities or hemorrhage and is able to visual deeper pathology in the choroid and sclera. Fundus images and OCT can be acquired in a single capture. Then Pin-Point™ Registration maps the position of the B-scan on the fundus image. The Triton series marks the first commercially available multi-modal swept source OCT in the US.
|
 |
SciFluor Reports Positive Results of Phase 1/2 Study in Topical Treatment of Exudative AMD
Results of Phase I/II trial have come back supportive for SF0166, SciFluor Life Sciences’s topical treatment for exudative macular degeneration. The Phase 1/2 study included 42 wet AMD patients taking either 2.5% or 5% SF0166 eye drops twice a day over 28 days. The study analyzed the safety, tolerability and initial efficacy of SF0166. No serious adverse events were noted. The drug also exhibited clinically significant biological activity with an average increase in visual acuity of five letters across the treatment group. SF0166 is a selective small-molecule inhibitor of integrin αvβ3. It has physiochemical properties that allows diffusion of high amounts to the retina.
|
 |
Ohr Pharmaceutical Announces Squalamine Fails Phase III Trial
In January, Ohr Pharmaceutical reported topline data from the MAKO study, which assessed the efficacy and safety of topical squalamine in addition to Lucentis injections to treat exudative AMD. The MAKO study was a multi-center, double-masked, placebo-controlled clinical trial. Participants were randomized to either topical squalamine 0.2% BID and monthly Lucentis injections or Lucentis monotherapy (topical placebo BID and monthly Lucentis injections). At the nine-month endpoint, the efficacy was assessed by visual acuity gain. Participants receiving Lucentis monotherapy fared slightly better with a mean gain of 10.58 letters vs. the combination therapy with a mean gain of 8.33 letters.
|
 |
FDA Approves Clinical Study of PRIMA Miniaturized Retinal Implant
Pixium Vision, based in Paris, France, announced that the US FDA has approved start of a clinical feasibility trial for PRIMA in patients with atrophic dry AMD. The University of Pittsburgh Medical Center will recruit up to five patients with vision loss attributable to advanced dry AMD. The study, expected to start in early 2018, will assess safety and the reestablishment of visual perception. A similar clinical trial has already initiated in France.
PRIMA utilizes 378 electrodes in a micro photovoltaic implant of just 2x2 millimeters in size and only 30 microns thick. The PRIMA implant is surgically placed in a subretinal position. Patients wear spectacles furnished with a camera. The camera converts images to near-infrared light and wirelessly transmits to the implant. The implant coverts this into electrical current to stimulate bipolar cells so that communication can be made to the optic nerve and brain.
|
 |
Genentech Announces Positive Results From Phase II BOULEVARD Study
Genentech’s RG7716 is the first intravitreal therapeutic with a mechanism to inactivate vascular endothelial growth factor A (VEGF-A) and Angiopoietin-2 (Ang-2). The Phase II BOULEVARD study compared two doses of RG7716 (1.5 mg and 6 mg) to ranibizumab in the treatment of diabetic macular edema At 24 weeks, patients (treatment-naïve to anti-VEGF) given 6 mg RG7716 had a mean 13.9 letter improvement, 1.5 mg RG7716 had a 11.7 letter improvement and those on 0.3 mg ranibizumab had a 10.3 letter gain. Genentech reported 6 mg RG7716 showed statistically significant visual acuity gains in comparison to 0.3 mg ranibizumab. Both strengths of RG7716 had a better decrease in central retina thickness, a greater improvement of diabetic retinopathy severity and were well-tolerated. RG7716 is also being studied to treat neovascular AMD within the Phase II AVENUE and STAIRWAY studies.
|
 |
pSivida Announces Second Phase III Study Profile at 12 Months for Durasert
pSivida, a developer of sustained release drug products, confirmed positive results 12 months in to a 36 month Phase III study of Durasert. The study is evaluating the recurrence of posterior uveitis in patients with Durasert vs. sham. The company reports a 36.6% decrease in recurrence of posterior segment uveitis in patients treated with Durasert compared to 71.2% of patients on sham treatment (p<0.001) over 12 months follow up. The average increase in intraocular pressure has been minimal at 2.0 mmHg in Durasert-treated eyes vs. 0.0 mmHg in sham-treated eyes. During the first 12 months, 50.5% on Duraset and 51.9% on sham needed IOP-lowering treatment.
Durasert, a miniaturized insert that allows for sustained-release of low-dose corticosteroid, is indicated for the treatment of posterior uveitis to reduce flareups for up to three years with a single injection. The company submitted a New Drug Application to the FDA in January 2018 and is awaiting a decision.
|

|
IMAGE QUIZ ANSWER
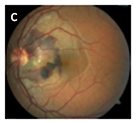
Image C in the gallery represents a traumatic choroidal rupture with subretinal hemorrhage and neurosensory serous detachment. This particular picture belongs to a 32 year old male that reported a high speed concrete projectile to the left eye about two weeks prior.
Choroidal ruptures are most often (80%) indirect, occurring remotely from the area of impact (countercoup). This most often occurs from non-penetrating, blunt trauma to the globe. The globe is mechanically compacted in the anteroposterior plane resulting in stretching in the horizontal plane. Bruch’s membrane is most susceptible to traumatic rupture as it is weaker than the sclera and less flexible than the retina. Initial visual acuity after the trauma is generally poor. The length of the choroidal rupture, proximity to the fovea and CNVM development are important features in predicting final visual outcome.
A: Medullated nerve fiber layer (Berg’s Syndrome) B: Cilioretinal artery occlusion
C: Proliferative diabetic retinopathy
|
WHY BECOME AN ORS FELLOW?
By Bill Denton, O.D., F.A.A.O.
Chair, Membership Committee
At some point in your career, you realize you just may be coasting. Your knowledge has been limited to the journals you receive and attempt to read, and the conferences that may not be as fulfilling as they once were. You simply need a challenge that will add an extra dimension to your professional learning.
Fellowship in the Optometric Retina Society (ORS) can provide several benefits in addition to the initial challenge of qualifying for this honor. Plenty of perks accompany your induction, but the coolest part is being associated with a body of knowledge and resources which can help you in many other ways. It is not uncommon to receive weekly thought-provoking emails about challenging cases and treatment dilemmas. Some fellows like to share their awesome cases they have diagnosed, while others post their cases with hopes that other Fellows will suggest an alternative differential diagnosis. At times it is like a round-table of brainstorming, but through the use of modern technology. Fellowship has little obligation with a huge opportunity for professional growth.
If you are up to the challenge of becoming a Fellow of the ORS, feel free to peruse the details and application at www.optometricretinasociety.org. Advice can be given to assist you in your quest. Feel free to contact us.
|
SPONSOR NEWS

Editor
in Chief
Anna K. Bedwell, OD, FAAO
Co-Editor
Brad Sutton, OD, FAAO |
Journal
Reviewers
Katelyn Lucas, OD
Senior Graphic Designer
Matt Egger
|
Review of Optometry® is published by the Review Group, a Division of Jobson Medical Information LLC (JMI), 11 Campus Boulevard, Newtown Square, PA 19073.
To subscribe to other JMI newsletters or to manage your subscription, click here.
To change your email address, reply to this email. Write "change of address" in the subject line. Make sure to provide us with your old and new address.
To ensure delivery, please be sure to add revoptom@lists.jobsonmail.com to your address book or safe senders list.
Click here if you do not want to receive future emails from Review of Optometry. |
|