| |
|
| Vol. 1, #12 • Thursday, December 3, 2020 |
|
|
|
|
| |
|
Review's Chief Clinical Editor
Paul M. Karpecki, OD, FAAO
Provides you with cutting-edge clinical strategies for optimal management of ocular surface disease and beyond.
|
|
|
|
|
|
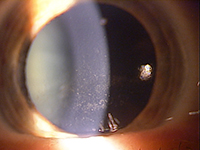 |
| A patient presenting for cataract evaluation with significant dry eye. |
|
The FDA approval of EYSUVIS™ (loteprednol etabonate 0.25% ophthalmic suspension) from Kala Pharmaceuticals for the short-term treatment of signs and symptoms of dry eye disease plays an important role in the management of DED patients. In this pearl, we’ll look at potential applications relevant to this labeling.
The recent approval of a new therapy for dry eye disease management begs the question of what the key applications for EYSUVIS™ will be. As a reminder, EYSUVIS™ is formulated with mucus-penetrating particle (MPP) Drug Delivery Technology to enhance penetration of loteprednol etabonate (LE) into target tissue on the ocular surface.
In order to identify the ideal applications for such a therapy, it’s important to have some understanding of dry eye “flares.” Most patients with chronic DED have episodic flares, usually four to six per year, triggered by a number of environmental stressors or activities.1 Contributing factors may include allergy season, air flow from continuous positive airway pressure (CPAP) machines or masks, arid environments, hormonal changes, digital device use, or anything that can increase tear osmolarity. These flares are typically associated with a rapid increase in symptoms, followed by prolonged levels of inflammation.
With that in mind, the following approaches may be good opportunities to prescribe EYSUVIS™ QID for up to two weeks.
1. In chronic dry eye patients. These patients on long-term medications such as cyclosporine or lifitegrast often experience flares. Treating them with EYSUVIS™ may serve to calm the flares so ongoing therapies can restore homeostasis.
2. DED patients who don’t want to remain on long-term therapy. One alternative to avoiding chronic therapy is to consider treating patients who present with more of a “flare and subside” dry eye expression with a two-week course of EYSUVIS™. The hope is this approach controls the condition for longer periods of time after patients discontinue the medication.
3. Patients with milder forms of episodic dry eye who need rapid resolution of signs and symptoms. I fall into this category. When traveling long distances on planes, where I often work for extended periods of time on my computer, my eyes get red and feel extremely dry with a foreign body sensation, a few hours into the flight. I currently dose myself with topical corticosteroids to remain asymptomatic for the duration of the flight and the remainder of my travels.
4. As induction therapy. Many patients don’t want to wait one to three months for improvement in signs and/or symptoms; yet, their clinical findings suggest the need for chronic dry eye therapy. To help these patients get faster relief from signs and symptoms, a two-week short course of corticosteroids prior to long-term therapy with lifitegrast or cyclosporine would be ideal.
5. Dry eye patients scheduled for cataract or refractive surgery. A two-week course of therapy may alleviate signs (and any symptoms if present) for these patients, as well as better prepare the ocular surface for surgery, and ideally help with surgical outcomes.
This new therapy, indicated for short-term treatment of DED signs and symptoms, has a meaningful place in a number of presentations. Next week, we’ll look at when topical corticosteroids are potentially contraindicated.
|
|
|
|
KEY TAKEAWAY: A new FDA-approved therapy serves an important role in dry eye management by offering short-term treatment of the signs and symtoms of dry eye disease.
1. Perez VL, Stern ME, Pflugfelder SC. Inflammatory basis for dry eye disease flares. Exp Eye Res. 2020; Oct 8. [Epub ahead of print].
|
|
|
|
| Supported by an independent medical grant from Kala Pharmaceuticals |
|
| |
| |
Review of Optometry® is published by the Review Group, a Division of Jobson Medical Information LLC (JMI), 19 Campus Boulevard, Newtown Square, PA 19073.
To subscribe to other JMI newsletters or to manage your subscription, click here.
To change your email address, reply to this email. Write "change of address" in the subject line. Make sure to provide us with your old and new address.
To ensure delivery, please be sure to add revoptom@lists.jobsonmail.com to your address book or safe senders list.
Click here if you do not want to receive future emails from Review of Optometry. |
|
|
|
|
|
|
|
|