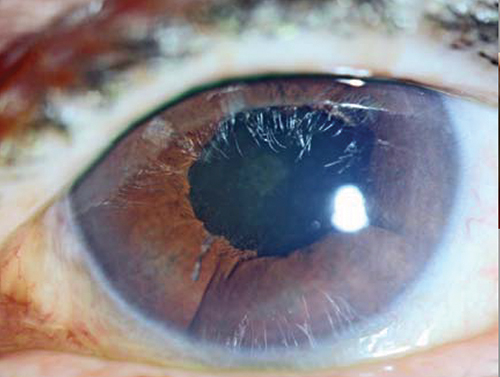
HLA-B27-associated uveitis can sometimes present with a secluded pupil, which has to be treated with a peripheral iridotomy (PI). “While the PI will most likely exacerbate the uveitis, you have to lower that pressure,” said Dr. Bronner. |
|
All You Need to Know About Uveitis
Attendees left this course with a comprehensive understanding of the many
etiologies of the condition—and how to handle them.
Aaron Bronner, OD, began yesterday morning’s session, “Managing Uveitis with Flair,” with a goal of providing “not just facts, but clinically useful information on uveitis you can use today.” He spent the first few minutes dispelling the common mindset that the condition “is no big deal,” with some sobering numbers.
Uveitis is causative in 10% to 15% of total blindness cases in the developed world, he said, and although many gradually regain vision, up to 20% are left legally blind.
Don’t Disrespect the Disease
So how do clinicians give uveitis the respect it deserves? By better understanding its sight-threatening implications, differentials and treatment options. Dr. Bronner dove into these topics with a brief primer on how cell and flare cause vision loss, and the long-term implications of ocular inflammation, including cataracts, glaucoma, cystoid macular edema and, less often, retinal detachment, epiretinal membrane and band keratopathy.
After discussing the many associated conditions, Dr. Bronner provided a few clinical pearls on managing uveitis patients. “If you aren’t comfortable with gonio, you shouldn’t manage uveitis patients,” Dr. Bronner said. “If you aren’t willing to dilate these patients, don’t manage uveitis.”
Therapy Rundown
Dr. Bronner then moved on to treatment protocols. The ultimate goal—eliminate inflammation—is simple, and he walked attendees through the common therapy escalation of a strong steroid, periocular injection, vitreal steroid implants and, for severe cases, immune modulators. “When Humira was first approved for uvieitis, everyone was excited and wondering if they should add it to their common therapy,” he said. “But we shouldn’t. It’s a very powerful drug, and should only be for severe cases. It comes with a lot of side effects.”
Clinicians can also consider nonsteroidal anti-inflammatory drugs (NSAIDs), which research now shows may be useful for some recurrent acute anterior uveitis cases, he said.
Dr. Bronner concluded the treatment portion of the lecture noting three common treatment errors to avoid: “not using cycloplegics in anterior disease, not fully controlling inflammation and being impatient with steroid taper,” he said. “These will get you into trouble.”
Diagnostic Trouble
While treatment is straightforward, Dr. Bronner said, diagnosing is not. “Really, you need to rely on the intersection between the clinical picture and patient setting,” he said. “Labs just aren’t sensitive enough.” On the other hand, the patient’s age, sex, race and other medical diagnoses are crucial to understanding their uveitis presentation and can go a long way to whittling down the differential list to make testing more useful.
“Uveitis can present with a laundry list of clinical findings,” Dr. Bronner added. “Not all findings present with each etiology. Knowing what is common for each etiology is the key to honing the differential.”
Differentials Galore
Dr. Bronner then spent the second half of the lecture running through those many etiologies, careful to include the usual clinical findings.
Everything from juvenile idiopathic arthritis, Behcet’s disease, herpetic disease and postoperative retained lens fragments to sarcoidosis tattoos and tuberculosis are all on the uveitis differential list. Dr. Bronner helped attendees get through the material by providing clinical pearls after each etiology. He concluded the lecture with an etiology “that’s mostly discussed as a curiosity, but it’s not all that uncommon,” he said. He sees as many as one patient a year with Fuchs’ heterochromic iridocyclitis—and he can’t treat them with steroids as you would a usual uveitis patient. “You have to treat the hypertension here, and then the cataract as soon as it forms.”
Dr. Bronner provided a final reminder before dismissing the lecture: “Don’t rely on labs—the clinical picture and patient setting are more helpful every time.”
NSAIDs in Uveitis Treatment
For clinicians looking for a therapy that bridges the gap between periocular agents and long-term immune modulators, research suggests oral nonsteroidal anti-inflammatory drugs (NSAIDs) may be surprisingly useful. Although NSAIDs have never been a part of the uveitis treatment protocol, Dr. Bronner discussed a small study from Massachusetts Eye and Ear that showed a reduction in uveitis episode recurrences by more than 63% in 44 patients with recurrent acute anterior uveitis.
The patients were on the maximum dose for each specific NSAID trialed for a at least six to 12 months prior to showing any reduction, and periocular steroid was used to control acute flare-ups. The researchers preferred COX selective celecoxib, unless cost was an issue for the patient.
While this is an off-label use, it may actually be very useful in optometric practice, Dr. Bronner said. “Of course, as with all long-term medications, controversy still exists, given the risk and reward balance of long-term NSAIDs in these eyes.”