 |
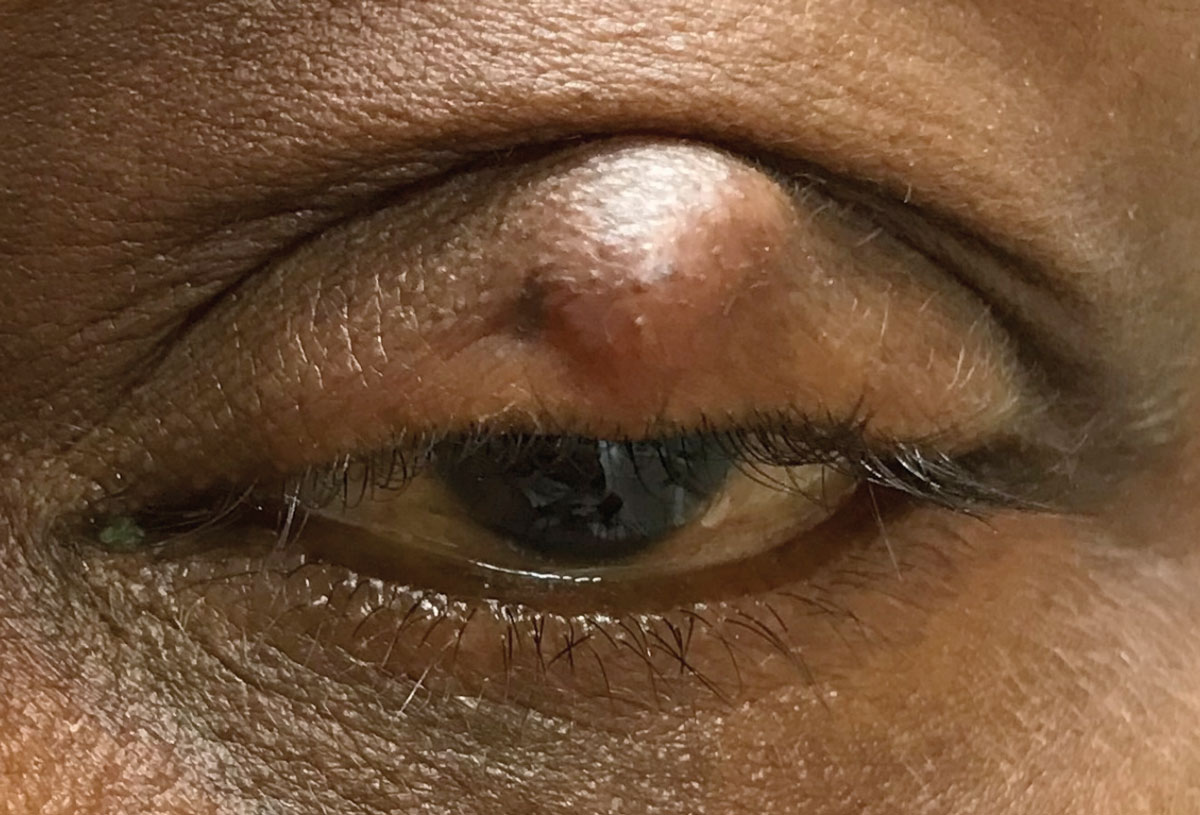
Antibiotics were not shown to improve chalazion in this study. Photo: Joseph W. Sowka, OD. Click image to enlarge. |
To treat a chalazion or hordeolum, antibiotics are often prescribed, but little evidence exists suggesting they should be the treatment of choice for both. In this study, researchers identified factors associated with antibiotics and the treatment success of various interventions.
A total of 2,712 patients were included, nearly 37% of which were put on antibiotics. In addition, antibiotic use differed among clinical sites, with patients seen in emergency and acute care settings significantly more likely to be prescribed an antibiotic for a chalazion.
Older age was associated with a higher risk of receiving an antibiotic for a hordeolum. Adding an antibiotic to conservative measures for a chalazion or hordeolum was not associated with an increased likelihood of treatment success. For hordeolums, neither antibiotics alone nor antibiotics in combination with conservative measures were associated with improved treatment success relative to conservative measures alone.
“Overall, success with medical management was highly favorable, and an antibiotic did not statistically improve the rate of resolution for either a chalazion or hordeolum, regardless of whether prescribed as a topical and/or oral formulation,” the authors concluded. “When medical management failed, a procedural intervention yielded excellent outcomes.”
A previous study showed that despite an association of blepharitis with chalazions, antibiotics were not found to improve their resolution regardless of type of formulation.
“Furthermore, when examining the tetracycline and macrolide classes, specifically endorsed for their anti-inflammatory and lipid regulating properties in blepharitis, a difference in treatment success for chalazions was not detected compared with other oral agents,” the authors explained. “However, when evaluating antibiotic regimens used for their proposed anti-inflammatory properties (long duration and/or low dose) as opposed to antimicrobial, a reduced risk of recurrent chalazions was observed. Interestingly, a higher risk of a recurrent hordeolum was noted for these regimens.
“The difference in effect is supported by the pathogenesis of these two entities and the proposed mechanism of anti-inflammatory antibiotic dosing,” the authors continued. “Improvement in chronic eyelid inflammation would be expected to reduce the risk of a recurrent chalazion, whereas under treatment (from a low antibiotic dose) or over-treatment (from a long duration) of eyelid bacteria could have deleterious effects for infectious hordeolums, such as the development of antibiotic resistance or eradication/disruption of commensal bacteria.”
The authors suggest further research is warranted to evaluate the potential role of anti-inflammatory antibiotic dosing regimens in preventing recurrent chalazia.
Alsoudi AF, Ton L, Ashraf DC, et al. Efficacy of care and antibiotic use for chalazia and hordeola. Eye Contact Lens. November 8, 2021. [Epub ahead of print]. |


