 |
|
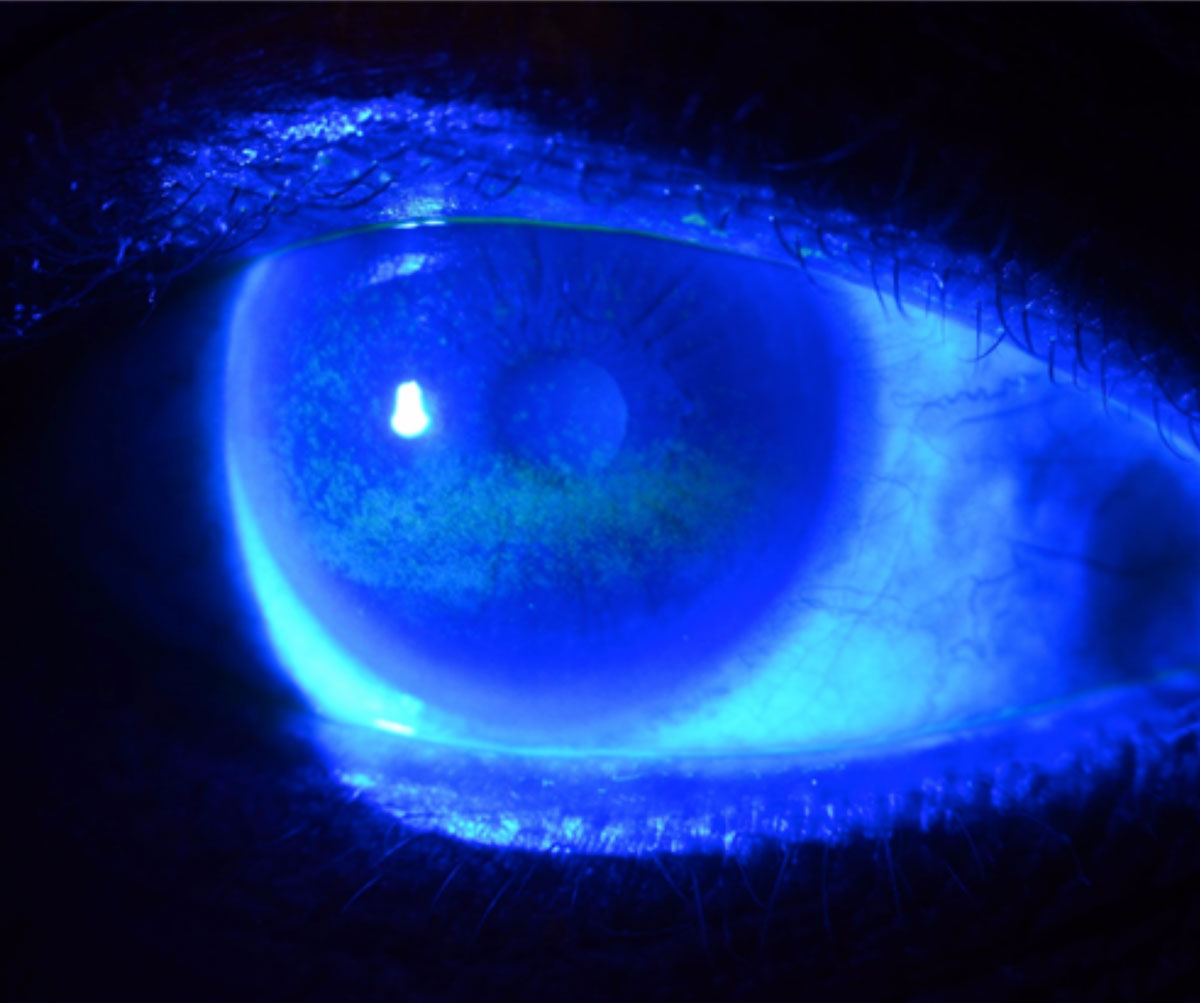
Despite the objective nature of diagnostic signs of dry eye such as corneal staining (above), researchers argue that clinicians should more strongly heed symptomatic reports when assessing their patients. Photo: W.R. Buie, OD. Click image to enlarge. |
Despite the widespread prevalence of dry eye, mismatch of the disease’s presenting factors is a common phenomenon that can complicate diagnostic workups. Recent research conducted in Taiwan examined initial presenting symptoms in relation to the sex of the patient. The retrospective design aimed to identify predictors of discordance between signs and symptoms in the Taiwanese population of dry eye patients.
Over seven years, 1,229 patients diagnosed with dry eye disease (DED) were included in the study. A composite score was derived using their initial presenting symptoms, which indicated discordance between symptoms and signs, using DED symptom severity sign severity scores.
A majority of patients (79.3%) were female, with a mean age of 57. Sex differences were not significant with initial presenting symptoms, but predictors of higher symptom severity score than sign severity scores did exist. These factors included being female and past surgical history of cataract, pterygium or conjunctivochalasis. However, lower symptom severity score than sign severity score was linked with older age and artificial tear use.
In their discussion, the study authors expand on their findings. Of symptoms reported at initial visit, the most common was sensation of dryness, which agrees with previous studies. Also consistent with prior studies was the finding of older age linked to lower symptom than sign scores. They did additionally find evidence of corneal sensitivity decreasing with age.
Although severity levels of signs and symptoms were often similar for men and women, women were more likely to report symptoms, which could be influenced through many factors. One possibility is that sex differences may exist in terms of ocular surface sensitivity and pain perception; this is evidenced through women’s generally lower pain threshold than men, the authors noted. Another reason may be ocular surface changes taking place due to hormonal states and variations; androgens can enhance ocular adnexal tissue function while estrogens may antagonize this and simultaneously activate inflammatory responses. Lastly, DED-related comorbidities are also more common in women, including allergies, depression and autoimmune diseases like Sjögren’s.
Although advanced age was associated with lower symptom severity score than sign severity score, previous cataract surgery could reverse this correlation and lead to more DED symptoms and post-op complaints. Interestingly, the researchers found those with diabetes to have lower symptom severity scores than sign severity scores, potentially masked by reductions in tear film stability, subbasal nerve density and corneal sensitivity that all can lead to corneal hypoesthesia, thus preventing symptomatology.
In regard to clinical practice, eyecare providers “should allocate greater attention to symptoms rather than relying solely on clinical signs when dealing with female patients, those with ocular allergies and individuals who have undergone surgical interventions for cataract, pterygium or conjunctivochalasis,” the researchers advocated.
As well, they caution that “it is essential not to dismiss the potential presence of DED solely based on the absence of subjective symptoms, especially among older adult patients, those with pre-existing cataracts or diabetes and those using artificial tears.” Keeping both points in mind, “early recognition and enhancement of postoperative care can improve patient satisfaction and quality of life.”
Lu PT, Lee CY, Sun CC. Sex differences and discordance between symptoms and signs of dry eye disease. Am J Ophthalmol. October 14, 2023. [Epub ahead of print]. |


