 |
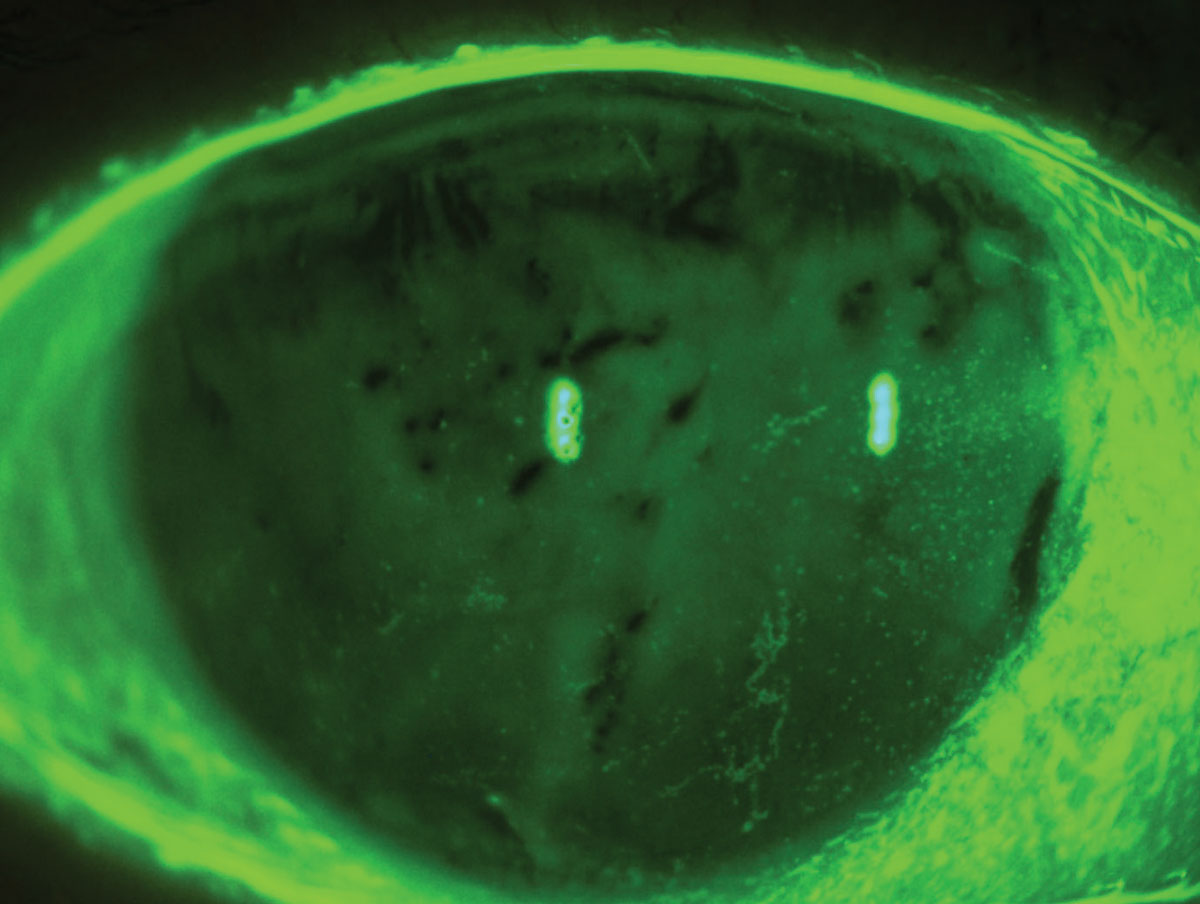
After analyzing 18 observational studies, researchers uncovered a potential link between dry eye disease, dyslipidemia and lipid-lowering drug use, though more research is warranted. Photo: Luis Rojas, OD. Click image to enlarge. |
Characterized by an imbalance in blood lipid levels, dyslipidemia is a common condition and heart disease factor affecting more than one in 10 people, with higher rates in men than women. Recent evidence has proposed a link between dyslipidemia and various ophthalmic disorders, including dry eye disease (DED) and meibomian gland dysfunction. To investigate the potential connection, researchers in China performed a systematic review and meta-analysis, which found that dyslipidemia and the use of lipid-lowering drugs could be associated with an increased risk of DED.
The team searched numerous online databases for observational studies published between 2000 and 2021. Eighteen studies, including a total of 2,663,126 patients, were ultimately selected for the review and analysis. The results demonstrated an association between DED risk and dyslipidemia (odds ratio [OR]=1.53), “especially elevated total cholesterol levels (OR=1.57), elevated low-density lipoprotein cholesterol levels (OR=1.13) and high-density lipoprotein cholesterol levels (OR=1.06), but not with serum triglyceride levels,” the researchers clarified in their paper. Additionally, they found that history of lipid-lowering drug use was positively associated with DED risk (OR=1.41).
While the current literature suggests there is likely an association between dry eye and dyslipidemia, the mechanisms behind this relationship remain elusive, the study authors explained. One possible explanation, they proposed in their paper, is that “serum lipid abnormalities potentially induce pathological changes in the ocular surface, including the corneal and conjunctival epithelia, lacrimal gland and meibomian gland.” Hence, “Ocular inflammatory changes could contribute to the pathogenesis of patients with DED,” they wrote.
Several studies have suggested that reducing dietary fat intake may help reduce serum lipid abnormalities. The researchers point to one that was conducted on mice and concluded, “A continuous high-fat diet for three months was found to be conducive to decrease tear secretion and reduce lipid accumulation via the activation of inflammation and oxidative stress of the ocular surface.” They continued, “By further knocking out cholesterol acyltransferase, an important enzyme catalyzing the esterification of cholesterol, the mice eventually developed dry eye-related ocular surface changes due to atrophy of the meibomian glands.” Compared to wild mice, both of these groups of mice had elevated serum lipid levels, especially total cholesterol levels, which the researchers point out “which might explain why high total cholesterol levels were closely associated with an increased risk of DED.”
One limitation of this review and meta-analysis is that varying strategies were used across studies to adjust for confounding variables. The researchers point out that five studies even failed to adjust for two of the most fundamental factors, age and sex. Other factors that varied between studies and may reduce the quality of evidence include diagnostic methods of DED, race and geography.
“Given the accumulating burden of patients with DED and the fact that dyslipidemia is an important risk factor for coronary heart disease, ophthalmologists and general practitioners could enhance their role in education and dietary guidelines for the management of patients with DED,” the study authors concluded.
Li Y, Xie L, Song W, et al. Association between dyslipidaemia and dry eye disease: a systematic review and meta analysis. BMJ Open. 2023;13:e069283. |


