 |
|
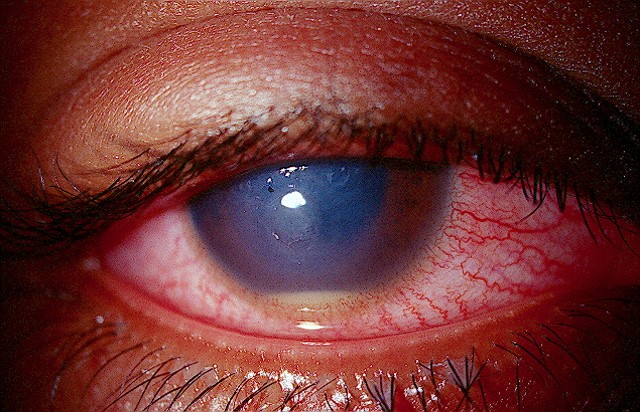
Prolonged use of a face mask during intravitreal injections did not lead to an increased rate of post-injection endophthalmitis. Click image to enlarge. |
Although it’s advisable in most high-risk settings to wear a face mask to reduce chances of airborne pathogen transmission, eye care specialists learned during the pandemic that it can also have deleterious effects on the ocular surface due to the redirecting of oral bacteria toward the eye. Still, the jury is out in some settings, including during intravitreal injection. Previous studies have not demonstrated an increased rate of endophthalmitis. The hypothesis was that contaminated masks could affect the flora in the periocular region, and/or the altered airflow could be associated with increased bacterial exposure in the sterile field.
Researchers at a university near Stuttgart, Germany recently investigated whether the introduction of universal compulsory face masking in public life leads to increased rates of post-injection endophthalmitis, finding no clear increased risk in their patient population. Six months after the mandate was enforced, no difference in visual acuity was detectable.
All injections of bevacizumab, ranibizumab, aflibercept, dexamethasone or triamcinolone between Jan. 2015 and Dec. 2021 were included in the retrospective analysis. The two study periods were defined by the introduction of the compulsory face masking rule in public life during the COVID-19 pandemic (Jan. 1, 2015 until April 27, 2020 vs. April 28, 2020 until Dec. 31, 2021). The injection procedure included the use of a sterile drape covering the head up to the shoulders which prevents air flow toward the eye.
A total of 83,543 injections were performed in a tertiary eye clinic, associated with a total of 20 post-injection endophthalmitis episodes (0.024%, one in 4,177 injections). Of these, thirteen were documented during the pre-pandemic period (0.021%, one in 4,773 injections) and seven during the pandemic period (0.033%, one in 3,071 injections). The researchers observed no significant difference in post-injection endophthalmitis risk, and there was no case of oral flora-associated post-injection endophthalmitis.
The median age of patients with endophthalmitis was 76. In the pre-pandemic group, the median age was 76 and 80 in the pandemic group. On median, patients had previously received 29 injections in the first group and 20 injections in the second. In the pre-pandemic group, endophthalmitis was associated with neovascular AMD in six patients, veno-occlusive disease in another six and diabetic macular edema in one. In contrast, in the pandemic group, endophthalmitis occurred in six patients with neovascular AMD and one with diabetic macular edema.
“Nevertheless, patients should continue to be educated about the importance of hygiene after intravitreal injections to minimize risk,” the researchers concluded in their paper. “In addition, consistent use of artificial tears should be advised during prolonged face mask wear to counteract the development of dry eye disease.”
Neubauer J, Gklavas K, Kortüm F, et al. Legal obligation in the general population: face mask influence on endophthalmitis after intravitreal injection. Graefes Arch Clin Exp Ophthalmol. 2023;261(1):97-102. |


