 |
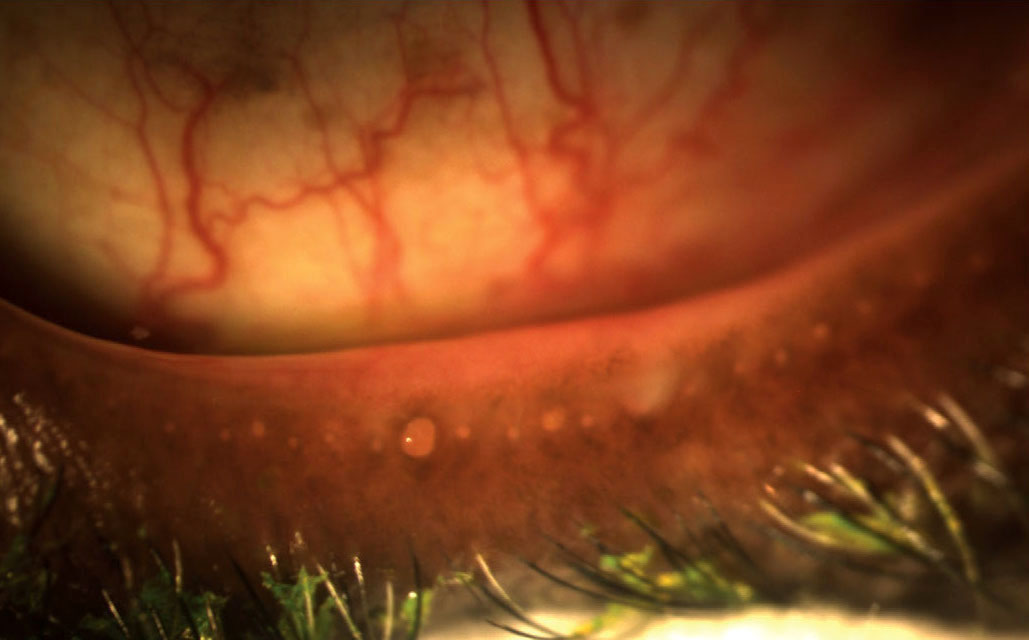
Lid margin score is among the most valuable parameters to evaluate MGD. Photo: Doan Huynh Kwak, OD. Click image to enlarge. |
Diagnosing meibomian gland dysfunction (MGD) is often a challenge, and while meibography can provide evidence of gland dropout, this approach is not always an option for many clinics. Therefore, researchers sought to determine which clinical ocular marker is most associated with meibomian area loss. Their secondary objective was to identify correlations with confocal microscopy imaging of the lid margin.
This observational, cross-sectional clinical study included 100 participants between the ages of 18 to 65. The researchers conducted a number of measurements of the right eye and its upper eyelid, including noninvasive tear breakup time, bulbar and limbal redness scores, blepharitis score, lipid layer thickness and number of parallel conjunctival folds, as well as tear osmolarity, corneal fluorescein staining, phenol red thread test, lid margin score, meibography and in vivo confocal microscopy. Participants also completed the Ocular Surface Disease Index questionnaire.
The study authors observed significant correlations between meibomian area and lid margin score as well as between meibomian tortuosity and lid signs of blepharitis. They reported that a lid margin score of 1.70 or greater detected meibomian area loss with a sensitivity of 0.58 and a specificity of 0.86. Additionally, they found that there were significant associations between meibomian area and orifice area at a 30mm depth.
Summarizing their findings, the study authors noted, “The lid margin score was most related to early meibomian area loss, and its assessment could assist in the early detection of undiagnosed MGD. A lid margin score of 1.70 [or greater] was considered abnormal. There is only a weak association between low-magnification meibography and high-magnification confocal microscopy imaging of the gland orifice area.”
Zhou N, Edwards K, Colorado LH, et al. Lid margin score is the strongest predictor of meibomian area loss. Cornea. March 5, 2022. [Epub ahead of print]. |


