 |
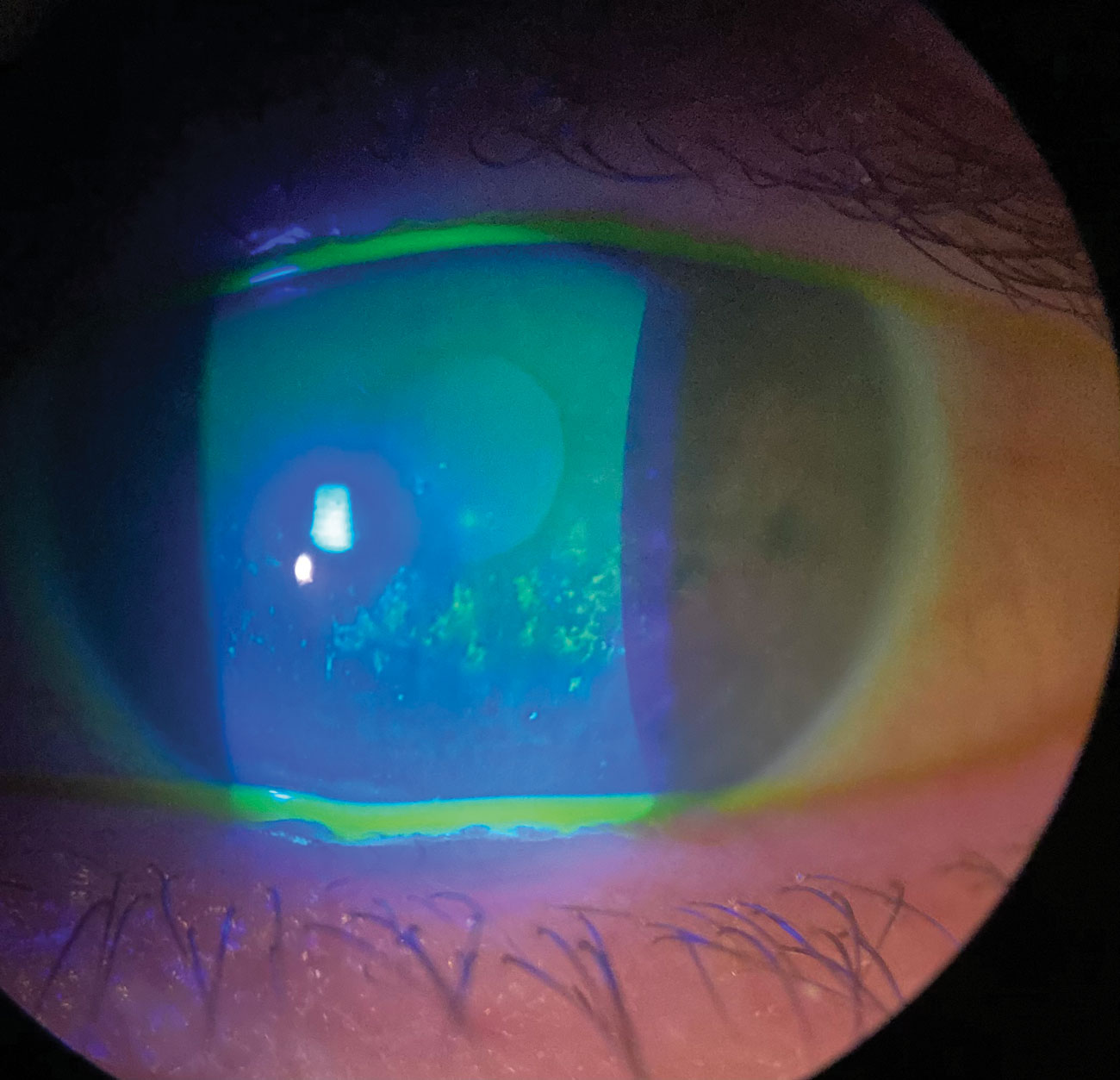
In patients with rheumatoid arthritis who experience ocular surface disease, clinicians should avoid tear osmolarity testing in the absence of independent studies confirming a diagnostic role, researchers argue. Photo: Pam Theriot, OD. Click image to enlarge. |
Dry eye disease (DED) is one of the ocular manifestations that can occur in rheumatoid arthritis (RA) patients, and clinicians generally value any diagnostic aids they can implement, but the role of measuring tear film osmolarity to determine if DED is present remains unclear. In a new study, researchers evaluated the diagnostic capacity of tear meniscus osmolarity measurement for DED in patients with RA using a portable osmometer (TearLab). They found the test showed low sensitivity, low specificity and limited agreement with the TFOS DEWS II composite reference standard for DED diagnosis.
A total of 101 RA patients were included—81 with dry eye and 20 without (controls). Researchers measured tear osmolarity and assessed other clinical diagnostic tests as suggested by DEWS II standard diagnostic criteria for DED. They analyzed the strength of agreement between osmolarity and the TFOS DEWS II composite reference standard for DED diagnosis.
The researchers found that tear meniscus osmolarity had a low diagnostic capacity for DED (area under the curve=0.57). Osmolarity measurement had a sensitivity of 35% and a specificity of 80% with a kappa level of agreement of 0.08 compared to the TFOS DEWS II composite reference standard. The low diagnostic capacity of osmolarity testing was similar for aqueous-deficient DED and for evaporative DED, being only fair for severe DED with a 57% sensitivity and 80% specificity and a kappa level of agreement of 0.36.
“The TearLab osmolarity test showed a high variability within patients, regardless of their clinical condition, either non-DED, DED or severe DED, which has also been reported by others, with different explanations,” the authors noted in their paper for the journal Diagnostics. They explained that the device only determines osmolarity of the tear meniscus, not the osmolarity of the precorneal tear film itself, “which can increase variability since tear meniscus osmolarity changes are more challenging to measure, and also due to stimulation of reflex tear secretion.”
They measured the osmolarity in the right eye first followed by the left eye, which allowed them to estimate differences attributable to the measurement order and found that, on average, the right eye had higher osmolarity values than the left eye (301.2 vs. 296.8 mOsm/L) with an average difference of 4.42 mOsm/L.
“This suggests that the TearLab osmolarity test might induce reflex tear secretion that reduces the osmolarity of the tear meniscus being more evident when measuring the second eye,” they wrote. An absolute inter-eye difference of 8 mOsm/L or higher has been proposed as diagnostic for DED. “However, the median absolute inter-eye difference was higher in patients without DED than with DED; and we found a similar proportion of patients with >8 mOsm/L of inter-eye difference across groups without DED, with DED, and with severe DED. Our findings suggest that the inter-eye osmolarity difference may not be informative to diagnose DED.”
In conclusion, this study suggests that tear meniscus osmolarity measured by the TearLab osmometer is non-informative to differentiate DED from non-DED in RA patients.
“TearLab diagnostic capacity should be analyzed by other research groups with no conflicts of interest to either corroborate or refute our findings,” the authors suggested. “The diagnostic advantage of TearLab needs to be clearly justified as the relative high cost of this platform for clinicians or health institutions, particularly in middle and low-income countries, and implies a significant investment.”
De La Parra-Colin P, Palacios-Aguirre KP, Perez-Pria-Kasusky A, et al. Diagnostic performance of the tear meniscus osmolarity measurement for dry eye disease in rheumatoid arthritis patients. Diagnostics. September 19, 2023. [Epub ahead of print.] |


