 |
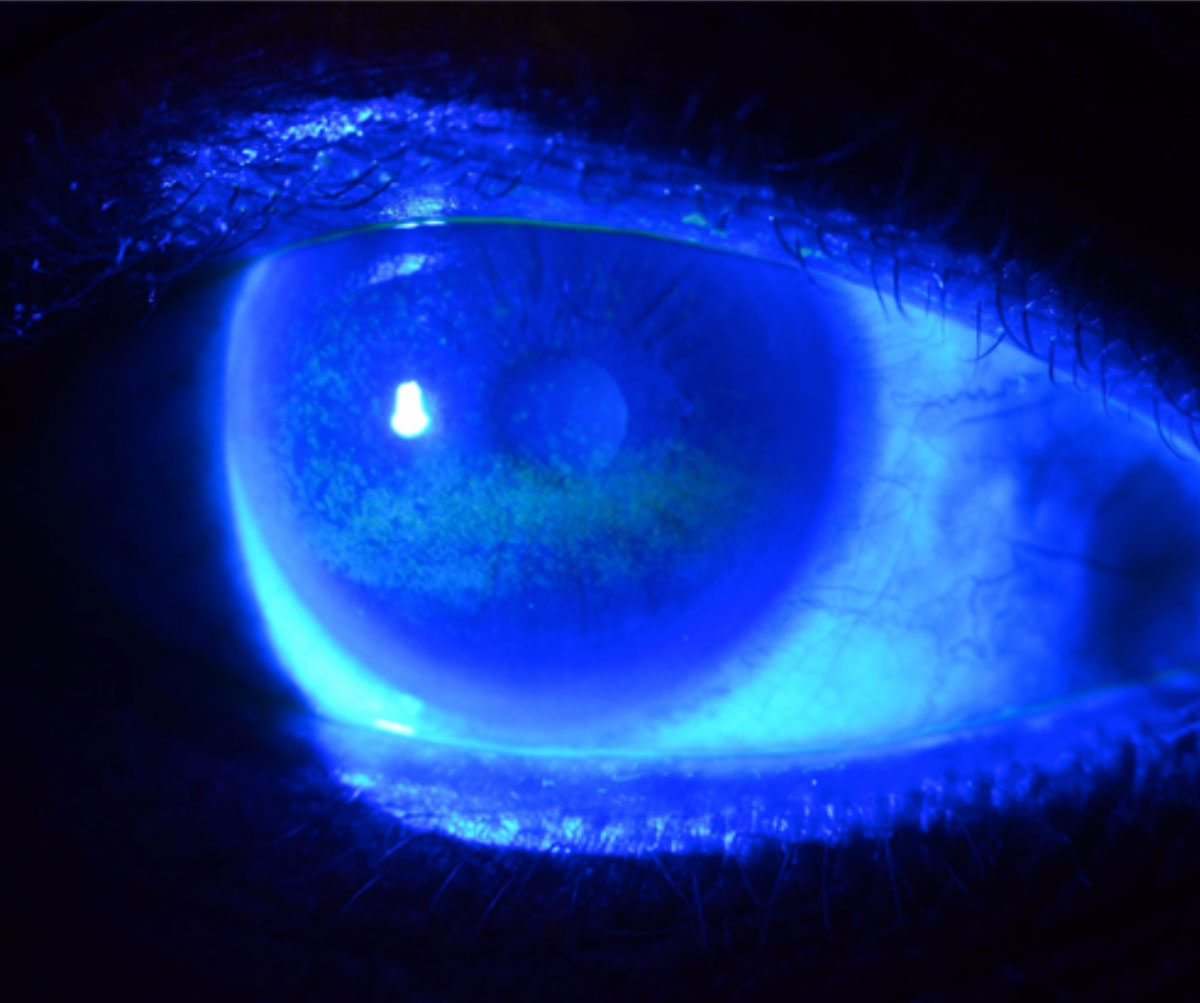
| Actual disease burden of dry eye may be underestimated due to discrepancy between clinical signs and symptoms, but SDOH indicators can help bridge this gap, researchers argue. Photo: W.R. Buie, OD. Click image to enlarge. |
It’s no surprise to optometrists that dry eye is widespread among the population, as any day in clinic will attest. Though extensively studied as a physical phenomenon arising from defects in tear film production, little evidence currently exists to describe dry eye’s connection to social determinants of health (SDOH). Defined as “the conditions in the environments in which people live, learn, work, play, worship and age,” SDOH span five domains: neighborhood and built environment; economic stability; social and community context; education access and quality; and healthcare access and quality.
A new literature review published in American Journal of Ophthalmology summarized what current evidence exists of associations between SDOH indicators and aspects of dry eye within the US, including diagnosis, care, symptoms, clinical signs and test results. Impact of SDOH indicators on dry eye were categorized as worsening, beneficial or null.
Of the 18 studies included in the analysis and spanning 51 SDOH indicators, most mapped onto the neighborhood and built environment domain. Increase in dry eye diagnosis or delayed specialty care to alleviate it was noted in 79% of SDOH associations, and 61% unveiled exacerbated dry eye symptoms. Influence of SDOH on corneal fluorescein staining was mixed, with 45% of factors increased tear break-up time and another 45% showed null associations. With these indications, the study authors convey that most of the SDOH indicators were associated with unfavorable dry eye measures, including higher disease burden, worse symptoms and delayed referral. Upon further analysis, the authors reveal that a substantial portion of the 51 potential SDOH indicators focused on climate or air quality’s effects on dry eye.
What was evident was that the “review findings revealed the scarcity of evidence on healthcare access, educational access and economic stability in relation to dry eye, highlighting the need for further research in these three SDOH domains as well as other aspects of obtaining quality eye care beyond accessibility.” Only one of the 18 included studies looked at the connection between education level and dry eye diagnosis, while only two examined aspects of eye care accessibility and affordability with quantifications like ‘self-reported visits to ophthalmologists or optometrists in the past month’ and ‘current health insurance type’ in relation to dry eye diagnosis or symptoms.
The authors suggest that “future work should focus on expanding and standardizing instruments for quantifying SDOH indicators across domains, reducing bias, increasing the sociodemographic diversity of the study population and disentangling how interaction among multiple social determinants affect patients with dry eye.”
Liu SH, Shaughnessy D, Leslie L, et al. Social determinants of dry eye in the United States: a systematic review. Am J Ophthalmol. January 17, 2024. [Epub ahead of print]. |


