 |
|
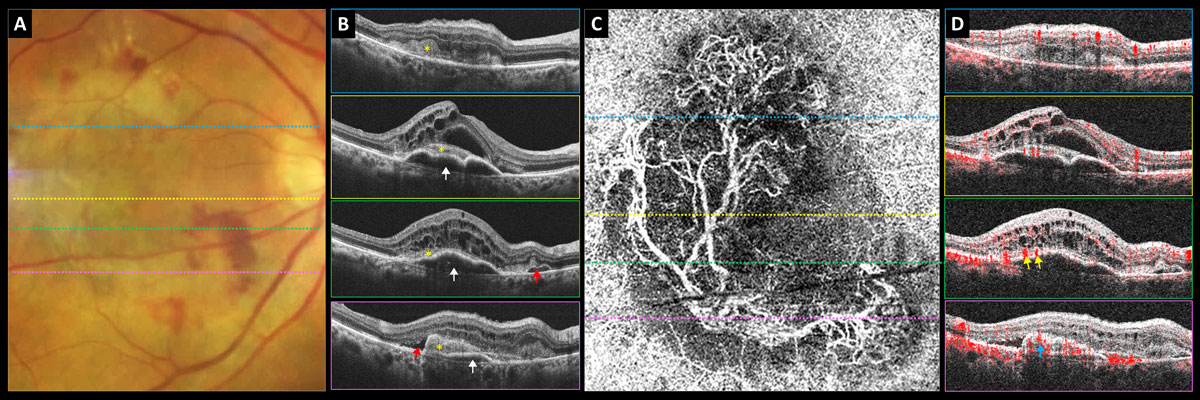
Nearly one out of every nine nAMD patients who discontinued treatment was lost to follow-up, while one out of every seven patients was nonpersistent with anti-VEGF therapy. Photo: Carolyn Majcher, OD. Click image to enlarge. |
Anti-VEGF has been proven to be a breakthrough treatment for neovascular age-related macular degeneration (nAMD), but it can’t help patients who don’t show up. A high rate of loss to follow-up was recently revealed among nAMD patients receiving anti-VEGF therapy.
In this study, researchers determined the incidence of loss to follow-up and nonpersistence in patients with nAMD treated with anti-VEGF injections in the United States and found that nearly one out of every nine patients discontinuing treatment were lost to follow-up, while one out of every seven patients was nonpersistent with anti-VEGF therapy.
A total of 185,138 eyes from 156,327 patients who were documented with treatment-naïve nAMD and subsequently treated with anti-VEGF therapy from 2013 to 2015 and followed through 2019 were included. The study disclosed a loss to follow-up rate of 11.6%. Loss to follow-up was defined as no follow-up within 12 months of the last intravitreal injection. Nonpersistence was defined as no follow-up within six months of the last intravitreal injection, and the rate was 14.3%.
Risk factors for loss to follow-up or nonpersistence included increasing age, male sex, Black or African American race/ethnicity, diabetes, unilateral involvement and Medicaid.
“Older patients likely have a greater number of comorbidities, mobility issues and transportation limitations that could impact adherence,” the authors wrote, noting that this finding is consistent with a previous study on loss to follow-up in patients with nAMD.
Patients with diabetes are associated with loss to follow-up and nonpersistence compared with those without diabetes and often have multiple comorbidities which could affect adherence.
“Patients with bilateral nAMD and better vision were less likely to be lost to follow-up and nonpersistent, suggesting that patients who see better or whose vision is threatened in both eyes may be more compliant,” the authors noted. “Women are less likely to be lost to follow-up and nonpersistent than men.”
When it comes to race and ethnicity, Hispanic/Latinos and Black or African Americans have recently been shown to have higher rates of visual impairment and blindness compared with white patients, previous studies reported. “These differences are likely due to inequalities in the distributions of social, economic and environmental resources associated with adequate healthcare access and favorable health outcomes,” the authors explained. “Compliance may be playing a role, and it further emphasizes the importance to further educate and empower these communities to stay on therapy to preserve their vision.”
For instance, in a survey of over 61 million US adults, participants reported poorer access to care, higher costs of care and less satisfaction with private insurance in comparison to public health insurance (Medicare, Medicaid and Veterans Health Administration or military coverage). “This is consistent with our results showing that patients with Medicare had better follow-up than private insurance but also inconsistent as patients with Medicaid did worse in comparison to private insurance,” the authors noted.
They concluded that improving treatment adherence and follow-up is critical to improve visual outcomes for patients with nAMD.
Khurana RN, Li C, Lum F. Loss to follow-up in patients with neovascular age-related macular degeneration treated with anti-VEGF therapy in the United States in the IRIS Registry. Ophthalmology. February 17, 2023. [Epub ahead of print]. |


