 |
|
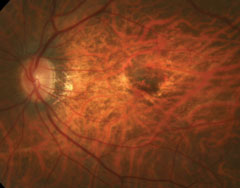
Among the risk factors for myopic macular neovascularization development are prior neovascularization, patchy atrophy and foveal RD. Photo: Mark Dunbar, OD. Click image to enlarge. |
It has been reported that myopic macular neovascularization impairs central vision at the onset and progresses to macular atrophy in the long term, both in non-treated eyes and those successfully treated with anti-VEGF agents. Therefore, it is important to determine the risk factors for the development of myopic macular neovascularization and treat the eye as early as possible. Researchers recently determined that severe grades of myopic maculopathy, prior myopic macular neovascularization in the fellow eye, presence of patchy atrophy and prior foveal retinal detachment (RD) are key risk factors.
The study reviewed 17,198 follow-up records from 5,409 eyes of 2,784 highly myopic patients during a nine-year period. All registered patients had at least one eye with an axial length longer than 26.5mm and/or a refractive error (spherical equivalent) of <-6.00D.
The results indicated that female sex, poorer best-corrected visual acuity, shorter axial length, prior myopic macular neovascularization in the fellow eye, severe grades of myopic maculopathy, presence of patchy atrophy close to the macula, foveal RD and macular hole were factors that were associated with a shorter time for the development of myopic macular neovascularization. Prior macular retinoschisis and prior macular edema were also significantly correlated with the development of myopic macular neovascularization.
Among these, myopic macular neovascularization in the fellow eye and the appearance of patchy atrophy were the main predictive indicators for the timing of myopic macular neovascularization development. The researchers noted that eyes with myopic macular neovascularization and patchy atrophy require intensive follow-up examination for myopic patients as the fellow eye has a risk of >70% for the development of myopic macular neovascularization in three years and nearly 80% in five years.
The researchers found it interesting that the eyes without patchy atrophy had almost the same risk of developing myopic macular neovascularization as eyes with patchy atrophy in the macular area. Compared with the eyes without patchy atrophy, patchy atrophy elsewhere than the macular area lowered the risk.
“Patients with these risk features should be managed with intensive follow-up examinations to monitor the development of myopic macular neovascularization in healthy eyes and intervene with prompt treatment once myopic macular neovascularization is detected,” the researchers concluded in their paper.
Du R, Xie S, Lu H, et al. Hospital-based study of risk factors associated with development of myopic macular neovascularization in highly myopic eyes. Ophthalmic Res. October 19, 2022. [Epub ahead of print]. |


