Editor’s Note: As part of our “Year in Review” retrospective, we’ve selected the top 30 news stories of the year and are re-sharing them as we close out 2022. Follow along as we count down to number 1!
This story was originally published on October 7, 2022.
 |
|
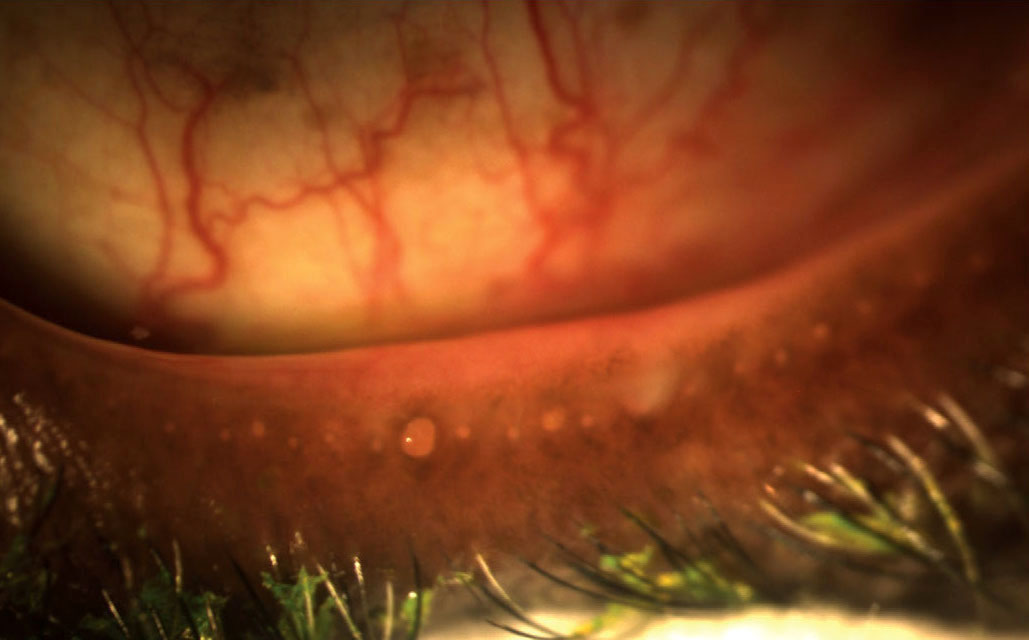
MGD patients older than 40 had a higher incidence of Demodex than their younger counterparts in this study, as well as more severe disease. Photo: Doan Huynh Kwak, OD. Click image to enlarge. |
Most ocular studies documenting the effects of Demodex infestations are conducted on the elderly due to higher incidence rates in this age group. However, one new study looked to investigate the potential differing influences that Demodex may have in younger vs. older patients. The study centered around ocular surface characteristics of those with meibomian gland dysfunction (MGD).
A group of 202 MGD patients (ages 18 to 70) were divided into two groups: young (18 to 40) and elderly (41 to 70). Observations were made about the different relationship between Demodex infestation and ocular surface and meibomian gland (MG) classifications for both groups. Additional observations compared both the relationship of the classifications between the groups.
Of the many parameters studied within the two classifications, it was broadly found that the incidence of Demodex was higher for elderly patients (60.2%) than the younger group (44%). The mean age of the Demodex-positive group was also older than both suspicious-positive and negative groups, potentially because of a weaker immune system and a decline in healthy hygiene habits sometimes seen in elderly patients. Similarly, the mean count of Demodex was greater in elderly patients compared to the younger group.
Researchers also found that MG expression, meibum quality, MG dropout, plugging of MG orifices and lid margin abnormality were all more severe in elderly Demodex-positive patients. The latter three listed were also more severe in the young Demodex-positive group. These three effects may be due to Demodex mechanically blocking MG orifices and hair follicles or transmitting bacteria that could induce an immune response.
Even further, the results indicate that a correlation between Demodex and lower tear film stability as well as corneal epithelial injury in the elderly. Results also showed that dry eye symptoms held a relationship with Demodex in the elderly group but not the younger subjects, as indicated by OSDI scores, which were higher in the elderly. Dry eye symptoms were worse in this group.
One effect Demodex did have on the younger group was its deleterious effect on meibum quality. Meibum quality was worse in the positive rather than suspicious-positive or negative cases. This is further accounted for by the increased meibum secretion found in the same group.
With many different parts of the ocular surface being affected, the authors present multiple considerations for practitioners, firstly bringing attention to the need “for early diagnosis and treatment of MGD patients with Demodex infestation,” they wrote. For all patients, they conclude, “Demodex eradication could alleviate dry eye symptoms in elderly patients but not in young patients. However, Demodex eradication may alleviate other ocular symptoms such as itching in young patients. MG physical therapy is also necessary in young Demodex infestation patients.”
Sun X, Liu Z, Sun S, Zhao S, Zhang X, Huang Y. The correlation between Demodex infestation and meibomian gland dysfunction at different ages. BMC Ophthalmol. October 1, 2022. [Epub ahead of print]. |


