 |
|
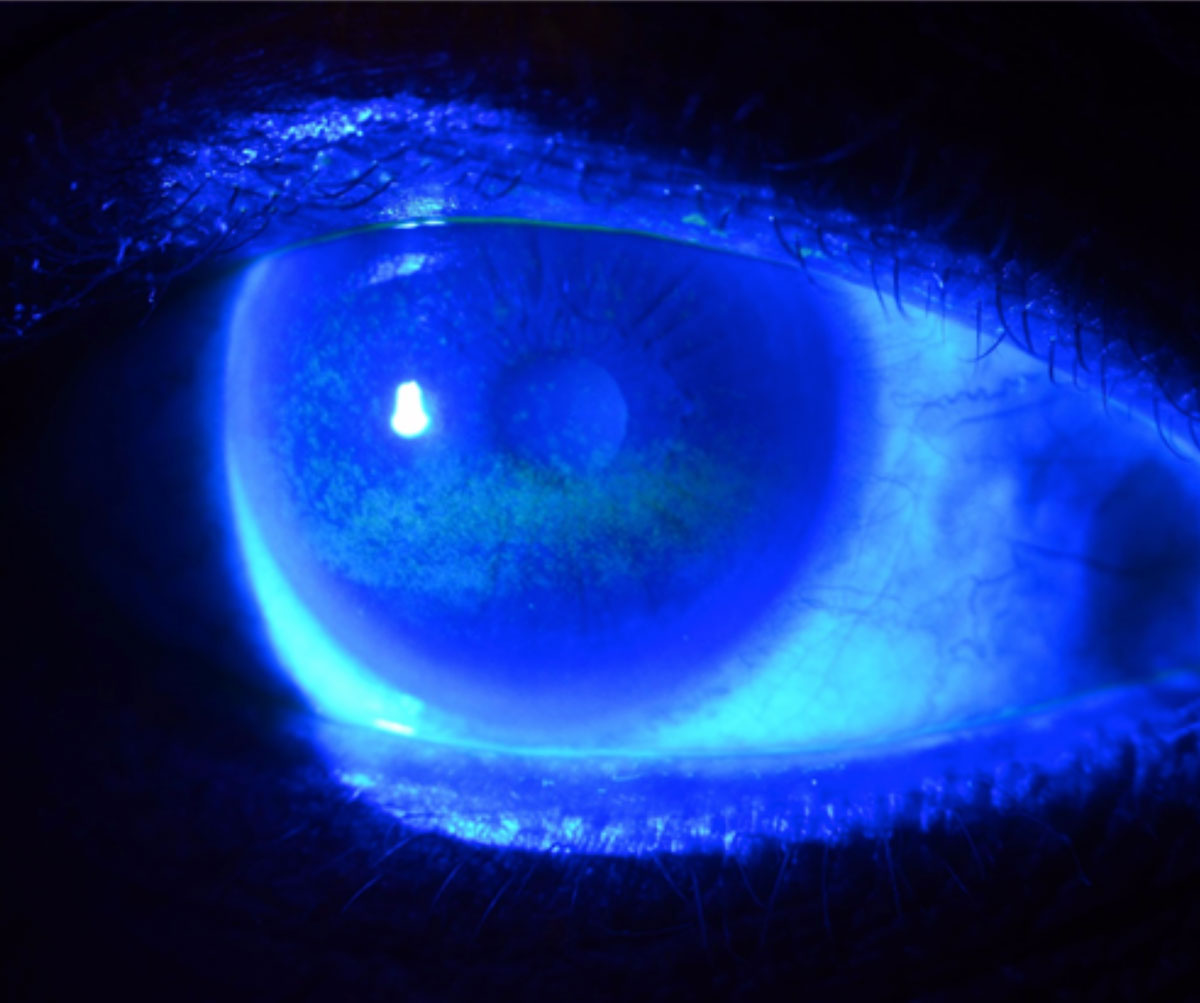
This study revealed that the co-occurrence of DED and exposure to anticholinergic drugs is not uncommon among adults. Photo: W.R. Buie, OD. Click image to enlarge. |
If you have patients who routinely use any medication classified as anticholinergic—including some popular antidepressants and antihistamines—bear in mind that they are a key culprit in medication-induced dry eye. In a recent study, researchers examined the relationship between anticholinergic burden and dry eye disease (DED), and found that taking at least one such drug was associated with an approximately threefold increase in the risk of DED in adults.
A total of 120 participants (more than half women) who underwent ophthalmological examination between February 2021 and February 2022 were evaluated, and drugs used by the patients in the last two months were recorded. Anticholinergic burden was assessed using a scale called the Anticholinergic Cognitive Burden (ACB).
Patients with DED had significantly higher Charlson comorbidity index (CCI) scores—a measure of the relative one-year risk of mortality based on 17 possible comorbid conditions—lower Schirmer test values, higher Ocular Surface Disease Index scores and higher anticholinergic burden, even after adjustments were made for possible confounding factors such as age, gender and comorbidity.
“As is known, there are many confounding factors in cases involving elderly patients, such as cognitive status, multiple drug use and comorbidities in particular, and this can be a problem, especially in studies conducted with this population,” the authors wrote. In one study, for example, “the peripheral side effects of anticholinergic burden were evaluated in a younger population (mean age of 56 years) using the ACB scale, and it was ascertained that an excess of anticholinergic load had a statistically significant effect on peripheral side effects such as fractures and falls. In light of the findings described here, we can say that our study is one of the rare studies evaluating anticholinergic burden, and especially in a younger population, while taking into account all comorbidities.”
Anticholinergic burden was associated with an approximately threefold increase in the risk of DED in adults (11.9%). All of these findings were consistent with previous study results.
“We showed for the first time that every one-unit increase in CCI score more than doubled the risk of DED,” the authors noted. “Therefore, systemic comorbidities such as drug use in people diagnosed with DED should not be ignored. These results also shed light on the importance of embracing a multidisciplinary approach toward affected patients.”
Greater caution in prescribing anticholinergic drugs for adult patients is important in reducing the rates of adverse outcomes, the authors suggested.
“In individuals at risk of DED, increased awareness of anticholinergic burden may allow for earlier targeted health interventions,” they concluded. “There is a need for future longitudinal studies to recommend strategies such as treatment changes or drug reduction for preventing the risk of dry eye in adults with high anticholinergic burden.”
Katipoglu Z, Abay RN. The relationship between dry eye disease and anticholinergic burden. Eye. February 9, 2023. [Epub ahead of print]. |


