 |
|
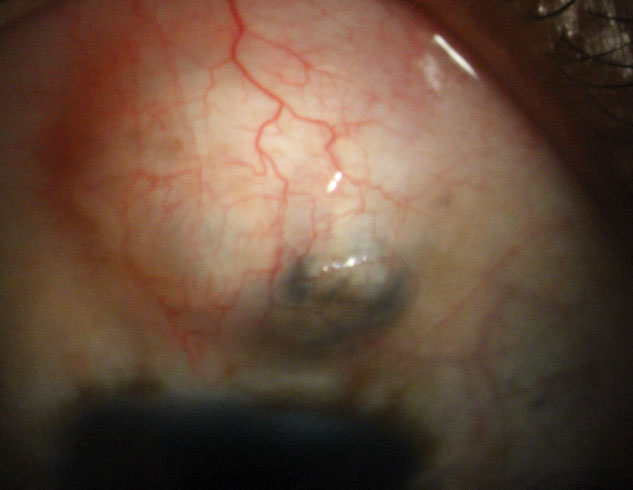
While trabeculectomy provided greater effect in OAG patients, eye drops were considered more cost-effective within a two-year period. Photo: Justin Schweitzer, OD. Click image to enlarge. |
Editor’s Note: As part of our “Year in Review” retrospective, we’ve selected the top 30 news stories of the year and are re-sharing them as we close out 2022. Follow along as we count down to number 1!
This story was originally published on August 9, 2022.
No. 13 biggest news story of 2022:
Approximately 25% of newly diagnosed patients with open-angle glaucoma (OAG) present with advanced disease in at least one eye. The vision loss associated with OAG can lead to significant impacts on vision, quality of life and healthcare resources. It is essential to understand management strategies that are both effective and provide the best use of these resources. Researchers in the United Kingdom have carried out a cost-utility analysis over 24 months and determined that, although trabeculectomy had slightly greater quality of life outcomes, eye drops were more likely to be considered cost-effective at this time horizon.
The Treatment of Advanced Glaucoma Study was conducted in 27 National Health Service secondary care glaucoma departments. Participant resource use, in terms of the type and frequency of resources used, was measured using bespoke case report forms that captured the use of resources such as intervention costs, surgery procedures, medications, post-surgery interventions and management of any resulting complications. The forms were completed at baseline, four months, 12 months and 24 months. Patient health-related quality of life was measured by the EQ-5D-5L, Health Utilities Index 3 and Glaucoma Utility Index. Results were expressed as incremental cost per quality-adjusted life year (QALY) gained.
Interestingly, the EQ-5D-5L proved to be the most likely to detect a difference in health-related quality of life in glaucoma patients. Using the larger multiple imputed data set, the incremental cost per QALY of trabeculectomy at two years is £45,456 (about $55,000). The probability of surgery being cost-effective at a £20, 000, £30,000 and £50,000 QALY threshold was 0%, 12% and 56%, respectively. “At two-years follow-up, surgery was unlikely to be considered cost-effective over the range of values that society might be willing to pay for a QALY,” the researchers noted in their paper.
“As OAG is a chronic, lifelong condition the full benefit (and costs) of each randomized intervention is unlikely to be captured within this time frame,” they wrote. “Further research will follow the longitudinal benefits of surgical and medical intervention beyond the two-year time horizon, as there is evidence from previous economic modeling studies that surgery could be considered cost-effective over a longer time horizon.”
Kernohan A, Homer T, Shabaninejad H, et al. Cost-effectiveness of primary surgical versus primary medical management in the treatment of patients presenting with advanced glaucoma. Br J Ophthalmol. July 26, 2022. [Epub ahead of print]. |


