 |
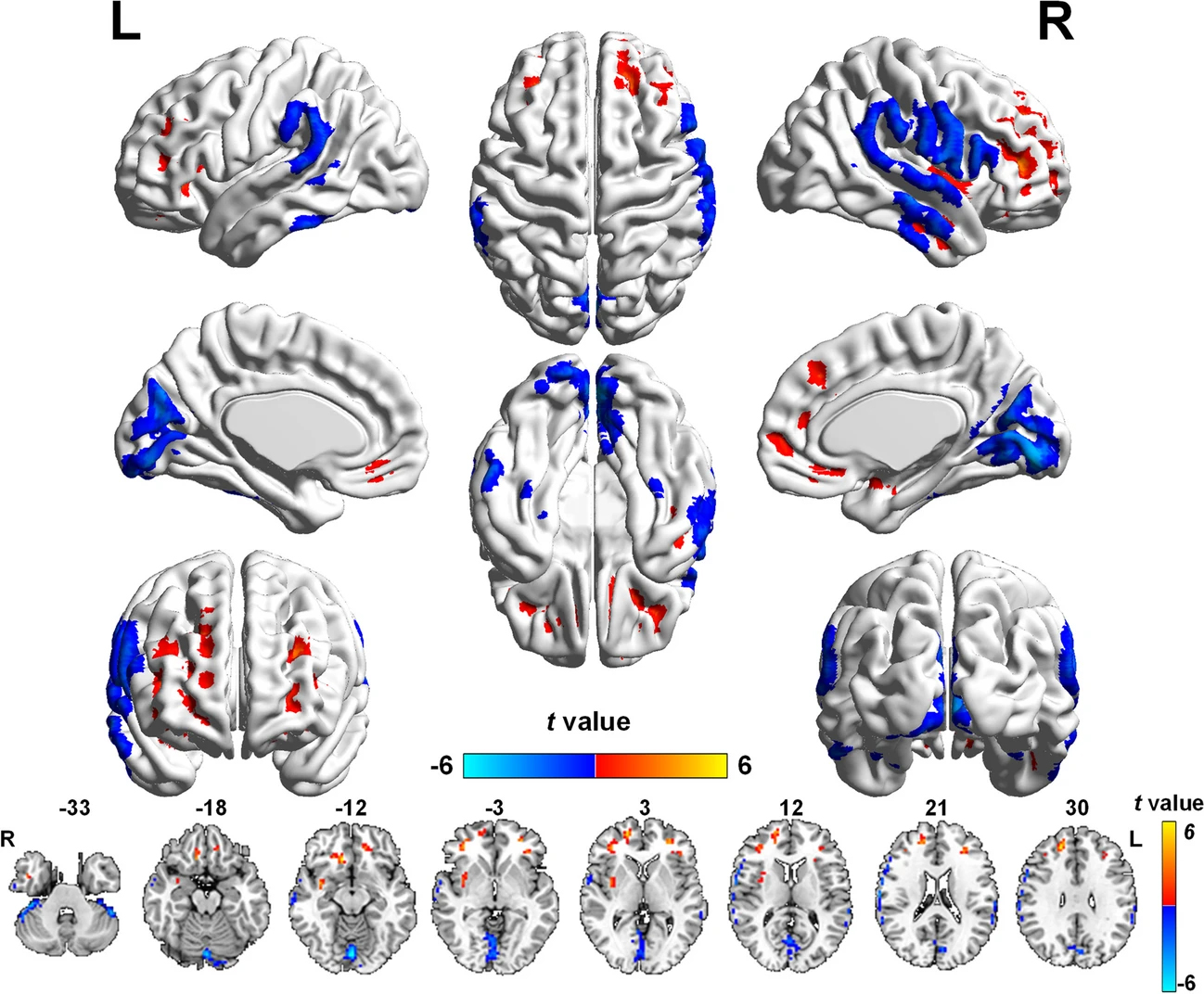
| Glaucoma can cause psychological disturbances in patients, including depression and anxiety, even at early stages. These MRIs from the study show brain regions with altered blood flow values in POAG patients. Blue = decreased flow, red = increased flow). Certain regions are also responsible for mood regulation and cognitive ability. Photo: Wang Q, Qu X, Wang H, et al. Brain Imaging Behav. Nov. 25, 2023./Creative Common 4.0. Click image to enlarge. |
Increasingly sophisticated imaging technology continues to reveal ways in which ocular neuroanatomy is an extension of the central nervous system, specifically the brain, in pathophysiology and clinical presentation. Primary open-angle glaucoma (POAG) is a neurodegenerative condition affecting not only the visual processing region of the brain, but somatosensory processing, motor control, emotional regulation and cognitive function as well.
Because cerebral hemodynamic function contributes to the pathogenesis of glaucomatous neurodegeneration, researchers in Beijing and Milwaukee wanted to investigate cerebral blood flow (CBF) redistributed patterns in visual and higher-order cognitive cortices. These regions were also studied in relation with clinical parameters in POAG.
Included in their study, recently published in Brain Imaging and Behavior, were 45 POAG patients and 23 controls who underwent an MRI technique called three-dimensional pseudocontinuous arterial spin labeling that measures resting state CBF. The researchers observed decreased blood flow in the visual cortices, postcentral gyrus, inferior parietal lobule and cerebellum of POAG patients and simultaneous increase CBF in the medial, middle and superior frontal gyri and the insula. Reduced cerebral blood flow in the visual cortices of glaucoma patients positively correlated with visual field defects; increased CBF in the right medial frontal gyrus was negatively associated with visual field defect and positively associated with cup-to-disc ratio. Negative connections weakening or converting to mild positive connections were observed in POAG patients as well as positive connections changing to negative connections.
More simply put, redistributed cerebral blood was not confined to the visual system. The structures that displayed decreased blood flow are areas with high neuronal activity, thus greater energy demands, and as a result may be more susceptible to conditions that endanger their needed energy supply, becoming prime neurodegenerative disease targets.
Moreover, correlation was observed between CBF changes and glaucomatous visual functional and structural damage. Relating to other cognitive functions, abnormal CBF in the visual cortices and left medial frontal gyrus correlated with anxiety and depression scores.
While altered blood flow is expected in the visual cortices of POAG patients, more interestingly noted in this article are the higher cognitive structures being affected, too. Mainly, the postcentral gyrus and inferior parietal lobule are key components of the primary and secondary somatosensory cortices, respectively. Both are involved in each stage of emotional processing and play central roles in emotional regulation. Increased CBF of the right insula was found, which also tends to emotional regulation and can be activated by negative emotional stimuli.
The increased CBF of the medial frontal gyrus means increased excitability, with higher perfusion as severity of glaucoma increases. The balance of the structure was impaired, and this is considered a pathogenic mechanism of anxiety disorders. Also relating to mental disorders was the finding of increased CBF on the left middle frontal gyrus; this structure is implicated in attentional reorientation, which the authors speculate enhances attentional bias toward negative stimuli, consistent with behavior of patients with depression and anxiety.
Glaucoma has previously been linked with mood and personality changes, and this study reinforces this relationship. For clinicians, it is important to remember that glaucoma may present with cognitive and/or personality changes. The authors echo this sentiment, reminding us that glaucoma is not just an ocular manifestation: “Regional and interregional CBF properties confirmed that the aberrant brain regions extend beyond the visual pathway,” they wrote, “including the somatosensory, emotional and cognitive networks, which highlights the importance of cerebral hemodynamic dysfunction in the pathophysiology of spreading neurodegeneration in POAG.”
Wang Q, Qu X, Wang H, et al. Arterial spin labeling reveals disordered cerebral perfusion and cerebral blood flow-based functional connectivity in primary open-angle glaucoma. Brain Imaging Behav. November 25, 2023. [Epub ahead of print]. |


