 |
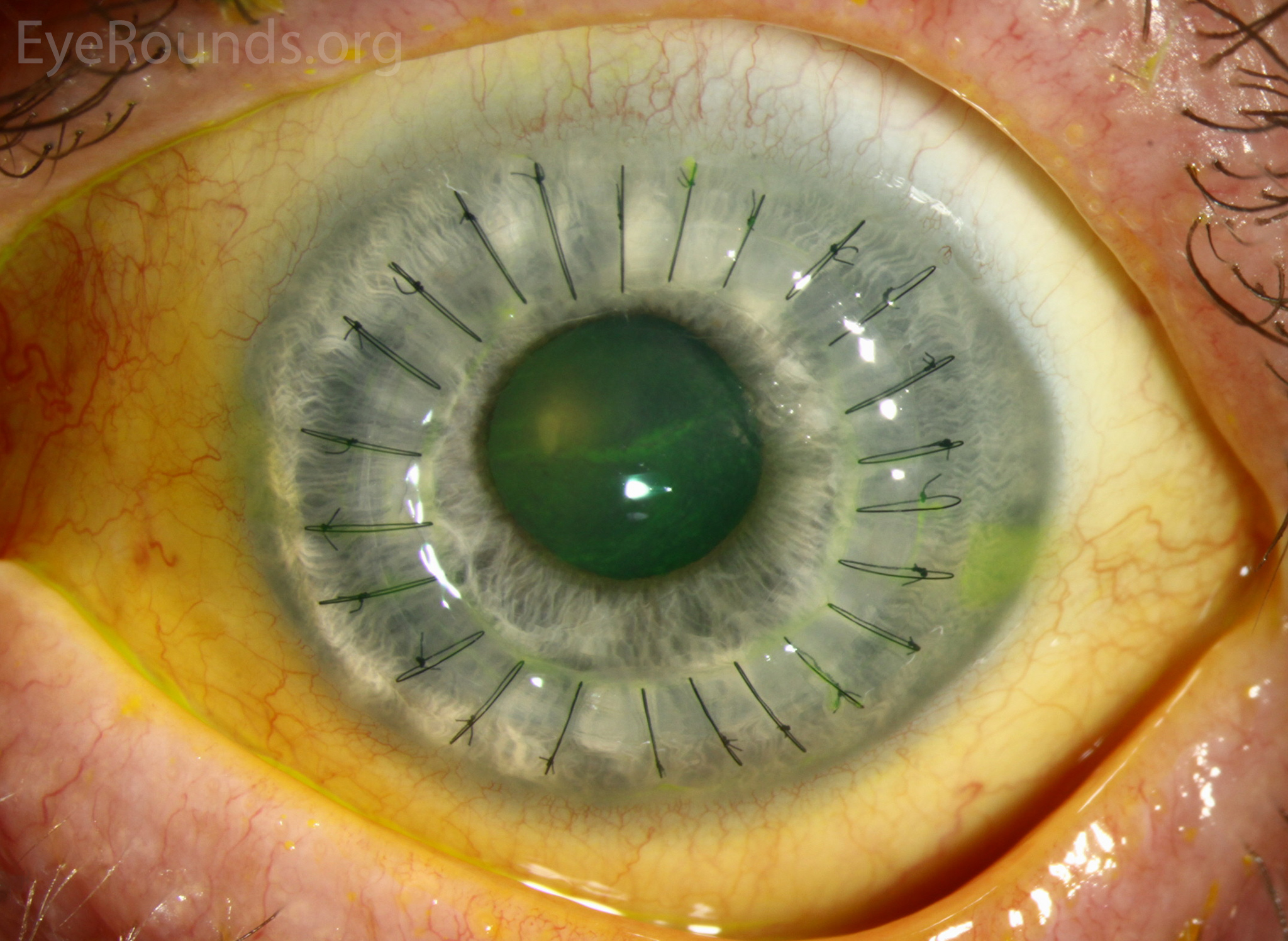
| Compared with PK, DALK provides higher survival of the corneal endothelium and a lower risk of postoperative elevated IOP in keratoconus eyes, study finds. Photo: Univ. of Iowa/eyerounds.org. Click image to enlarge. |
Deep anterior lamellar keratoplasty (DALK) and penetrating keratoplasty (PK) have both been shown to be successful in treating keratoconus, though differences in long-term outcomes and graft survival between the two methods are not well studied. To fill this gap in research, a recent study looked at 20-year data of patients who received DALK and PK and found that the former procedure offers a higher endothelial survival and lower risk of postoperative ocular hypertension than the latter.
The retrospective comparative case series included 228 patients who had received DALK (103 months of follow-up, on average) and 274 who received PK (106 months of follow-up) for keratoconus between 1993 and 2021 by a single surgeon. Among the 502 total eyes, graft survival was 96.7% at 10 years and 95.6% at 20 years. Visual acuity improved from 20/378 preoperatively to 20/32 at 30 months post-op, and corneal epithelial cell density decreased from 2,494 cells/mm2 to 1,521 cells/mm2 at 10 years. The mean simulated keratometry increased from 44.88D at one year to 46.60D at three years, then remained stable.
When comparing the graft survival rates of DALK and PK, the researchers noted rates at 10/20 years of 96.4%/94.9% in the PK group and 97.0/97.0% in the DALK group. They then totaled the reported cases of post-op ocular hypertension requiring treatment and found a cumulative incidence that was 50% higher in PKs than in DALKs. This is despite the fact that significantly more DALKs had a preoperative intraocular pressure above 20mm Hg and/or a history of glaucoma.
Additionally, the team found that early- and late-phase rates of epithelial cell density loss were 50% lower in DALKs than in PKs. Simulated mean keratometry was also significantly higher in DALKs than in PKs at 10 years, but not at 20 years. Visual acuity outcomes at both time points were comparable between the two procedures.
The researchers identified one potential downside of manual dissection-DALK compared with big bubble-DALK and PK: longer recovery time during the first five years. Beyond this, no significant differences in outcomes were noted in manual dissection-DALK vs. big bubble-DALK.
While both DALK and PK appear to provide high 20-year graft survival and good visual recovery, “DALKs featured a lower risk of adverse events than PKs in our study,” the team summarized in their paper, published recently in British Journal of Ophthalmology. “Higher postoperative epithelial cell density and lower risk of postoperative ocular hypertension requiring treatment were the main advantages of DALK over PK. For those reasons, DALK should be preferred to PK for treating keratoconus,” they concluded.
Borderie VM, Georgeon C, Sandali O, Bouheraoua N. Long-term outcomes of deep anterior lamellar versus penetrating keratoplasty for keratoconus. Br J Ophthalmol. October 27, 2023. [Epub ahead of print]. |


