 |
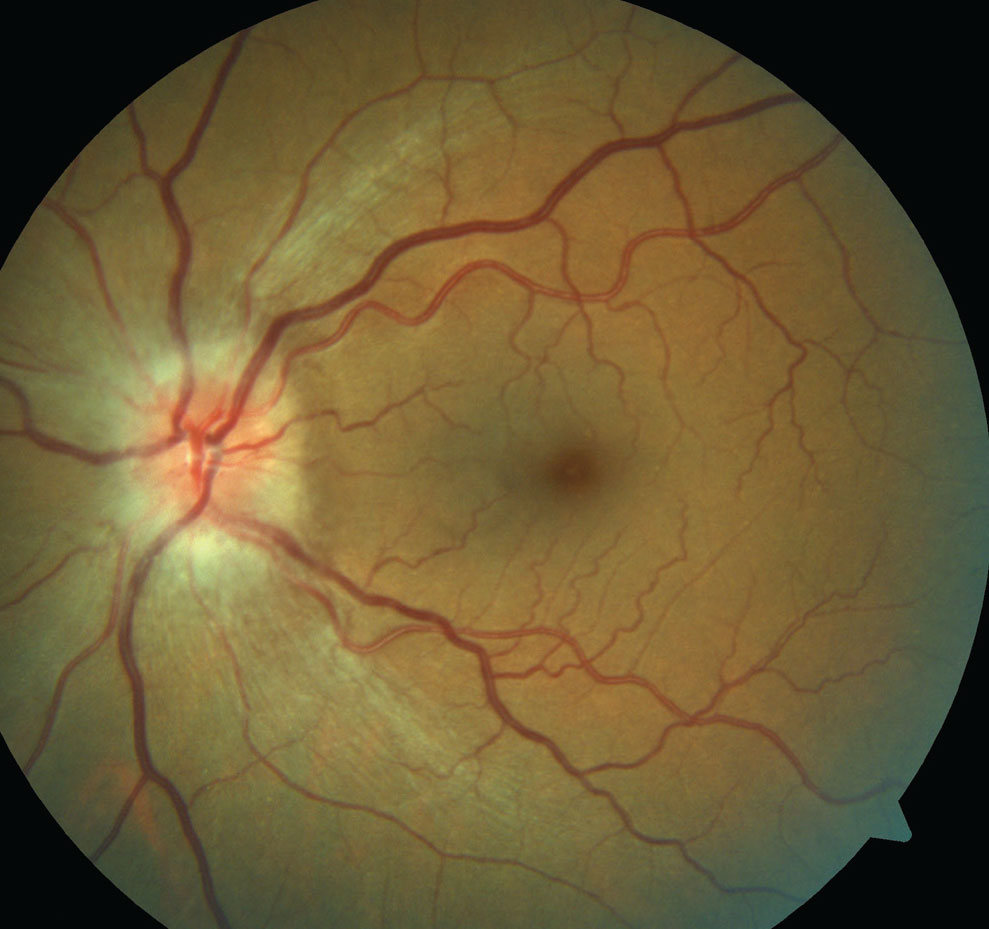
| Nasal- and temporal-quadrants were best-suited to predict favorable VF and VA outcomes, respectively. Photo: Michael Trottini, OD, and Candice Tolud, OD. Click image to enlarge. |
New research conducted in Thailand examined results of patients experiencing acute nonarteritic anterior ischemic optic neuropathy (NAION) to evaluate the utility of peripapillary retinal nerve fiber layer thickness (pRNFLT) in anticpating visual acuity (VA) and visual field (VF) outcomes.
Included in the retrospective analysis were 60 eyes of 60 individuals with acute NAION. Reliable VF values were able to be obtained in 30 eyes at the initial and six-month follow-ups; these were included in the VF analysis. pRNFLT was measured both globally and separately in all four quadrants using OCT at initial visit. Using pRNFLT as a prediction of visual outcomes, favorable VA was defined as better or equal to 20/25 and favorable VF was defined as a visual field index (VFI) of ≥90% at six-month follow-up.
At initial visit, median VA was 0.4 and median VFI was 73.1%±6.7%. At six-month follow-up, median VA was 0.3 while median VFI was 69.3%±28.9%. the tinner temporal-quadrant pRNFLT was associated with favorable VA, with a cut-off value of 128µm. Favorable VF was mapped onto thinner nasal-quadrant pRNFLT, with a cut-off of 105µm.
From these results, the authors were able to determine that pRNFLT is indeed a clinically useful way to predict visual outcomes of acute NAION patients. They further elucidate why this might have been the case: “We speculate that this finding can be explained by the temporal-quadrant pRNFLT being representative of the papillomacular bundle (PMB), and this visual outcome (VA) deficit may depend on the severity of the damage sustained by the PMB. For example, the less severe is the damage to the PMB, and therefore the thinner is the temporal-quadrant pRNFLT, the less severe is the visual outcome (VA) deficit.”
One retrospective study showed chronic NAION eyes’ VA displayed a strong negative correlation with the temporal-quadrant pRNFLT, while no correlations between global and other quadrants of pRNFLT and VA were seen.
The authors add an interesting finding that absence of diabetes was associated with favorable VA, which reflects results similarly seen in one previous study. This previous investigation only included acute NAION eyes in Thailand and displayed that diabetes presence was a predictor of poor VA improvement.
Clinically, the authors of this study establish that “we have established cut-off values of pRNFLT for the prediction of favorable VA and VF in the Thai population. These cut-off values could be used by ophthalmologists and neurologists to provide better information regarding the visual prognosis of patients, which is an important part of the therapeutic approaches of acute NAION, owing to the lack of proven effective treatments for acute NAION.”
Sriwannavit S, Padungkiatsagul T, Jindahra P, Vanikieti K. Peripapillary retinal nerve fiber layer thickness as a predictor of visual outcomes in patients with acute nonarteritic anterior ischemic optic neuropathy. Clin Ophthalmol. 2024;18:1133-42. |


