 |
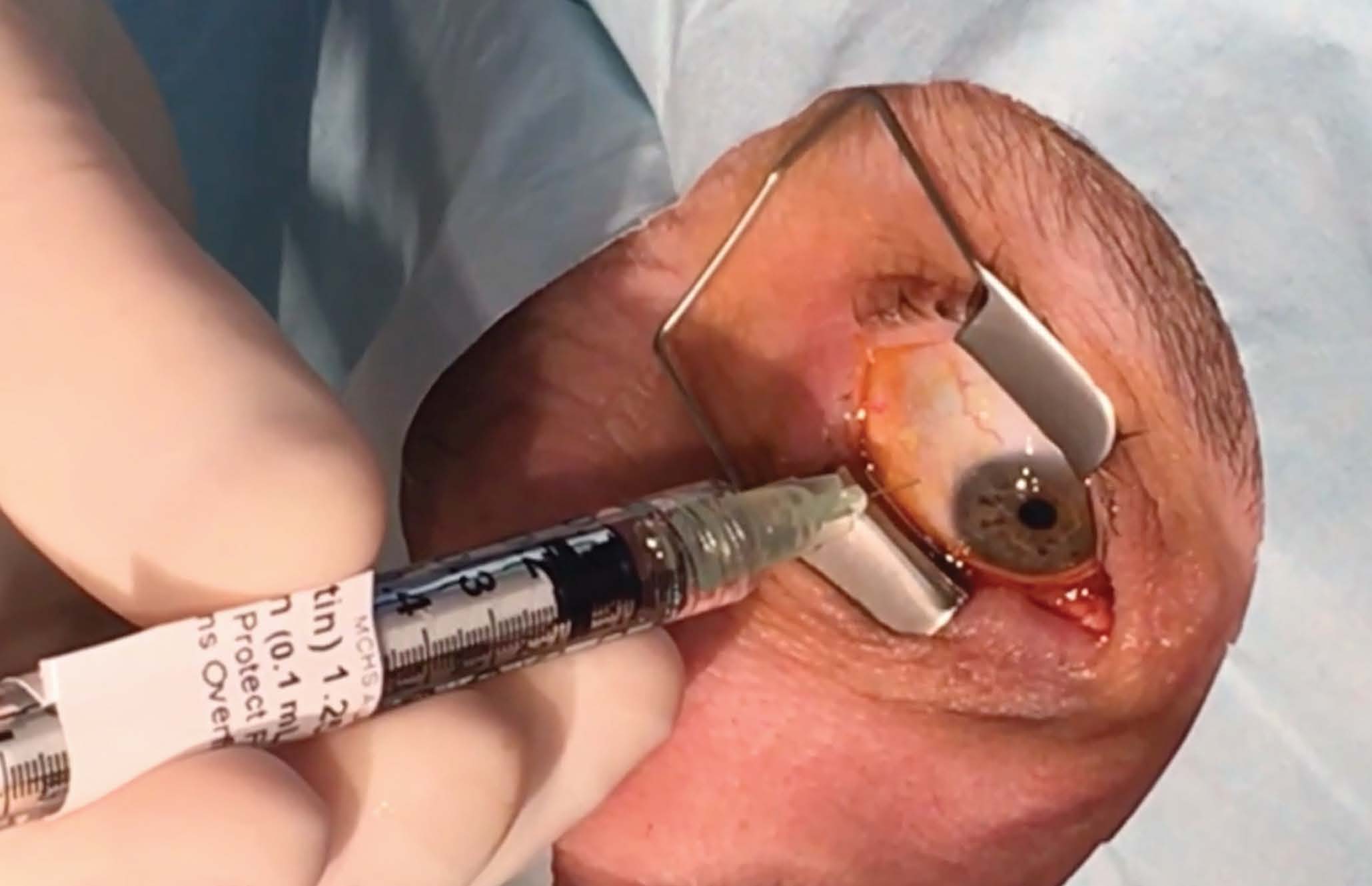
The IRIS Registry collects information from almost 70% of ophthalmology practices in the United States, across all payers and all populations, including those without insurance. This vast reach provides a powerful, representative sample of the US population. Photo: Leo Skorin, OD. Click image to enlarge. |
Real-world scenarios usually don’t align perfectly with carefully monitored clinical settings, so the true impact of many treatments often varies. Fortunately, large databases such as the IRIS Registry enable powerful real-world analyses of ocular outcomes. Using this resource, researchers looked into anti-VEGF treatment patterns and the influence of patient demographics on neovascular age-related macular degeneration (nAMD) outcomes. Their findings confirmed that the burdens patients face make it challenging to adhere to treatment.
The retrospective, noninterventional, real-world study included a cohort of 226,767 patients (254,655 eyes; 160,423 with visual acuity data) with a first anti-VEGF and at least two years of follow-up.
The researchers found that patients experienced a mean visual acuity increase of three ETDRS letters at year one, but this was followed by annual decreases, leading to a net loss from baseline of 4.6 letters after six years. They noted that patients with longer follow-up had better baseline and follow-up visual acuity.
The mean number of injections was 7.2 in year one and 5.6 in year two. Injections plateaued in years three to six between 4.2 and 4.6 injections. A total of 38.8% of eyes discontinued treatment and 32.3% switched treatment. Adjusted data showed that each additional injection led to a 0.68-letter improvement from baseline to year one, leading the researchers to conclude that multiple injections in a year could be clinically meaningful.
The following risk factors were associated with increased risk of vision loss at year one: older age, male sex, Medicaid insurance and not being treated by a retina specialist. During follow up, 58.5% of patients lost 10 or more letters of vision at least once, and 14.5% had sustained poor vision after a median of 3.4 years.
“Overall, these findings suggest that most patients with nAMD may find it difficult to adhere to the requirement for frequent intravitreal anti-VEGF injections and could therefore be at risk of experiencing poor vision outcomes,” the researchers concluded. “New therapies, including those with different modes of action and/or new routes of administration, which safely reduce treatment burden by extending the duration between re-treatments while maintaining optimal efficacy outcomes could result in improved visual outcomes for patients in routine clinical practice.”
Wykoff CC, Garmo V, Tabano D, et al. Impact of anti-VEGF treatment and patient characteristics on vision outcomes in nAMD: up to 6-year analysis of the AAO IRIS Registry. Ophthalmology Science 2023. [Epub ahead of print]. |


