 |
|
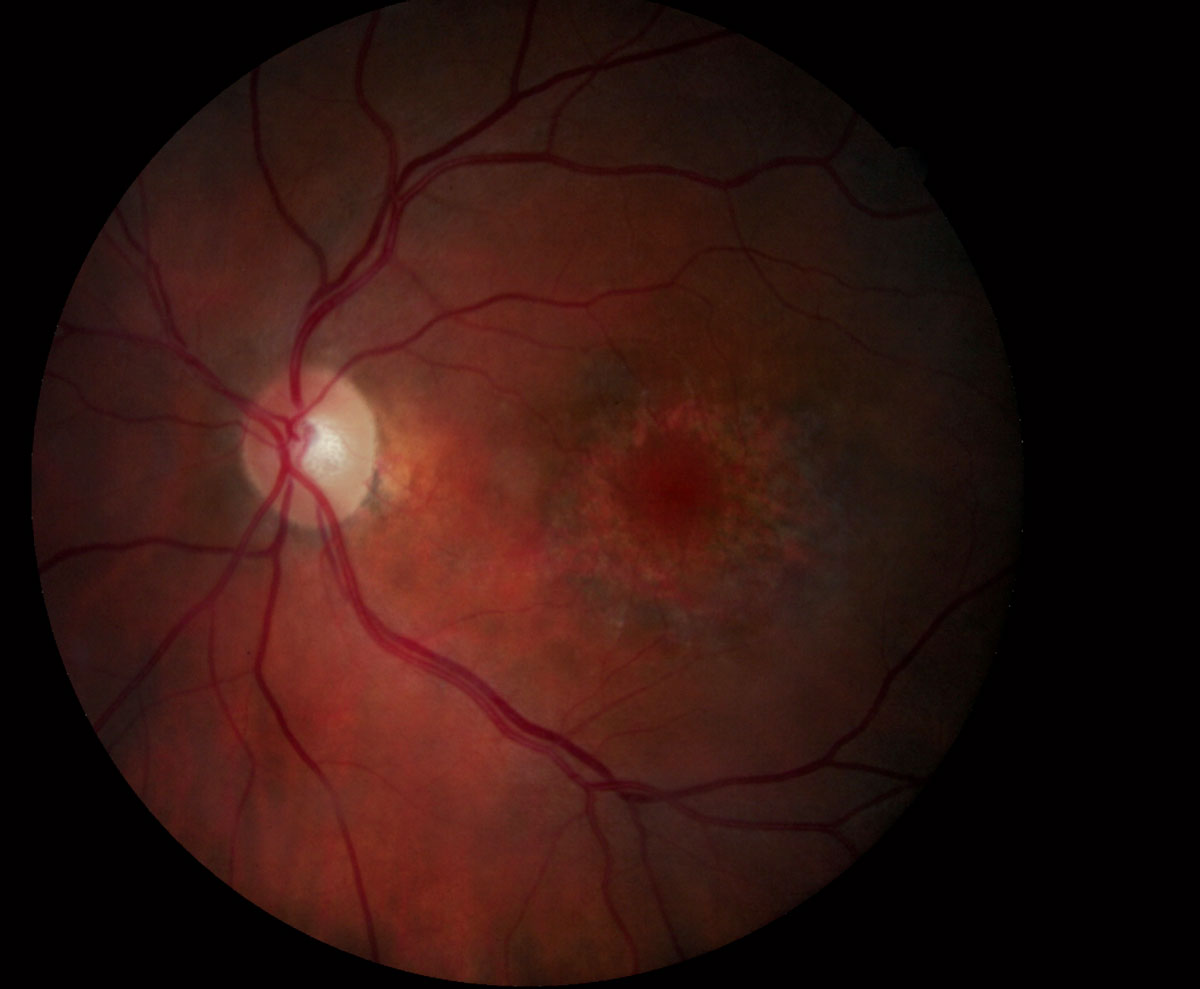
Conventional fundus examination may not always reveal Plaquenil toxicity, seen here. Earlier identification is possible with advance OCT devices. Image courtesy of Marlon Demeritt, OD. Click image to enlarge. |
Researchers recently evaluated the efficacy of swept-source OCT angiography (SS-OCT-A) in patients who underwent hydroxychloroquine (HCQ) treatment for more than five years, a drug that can cause retinopathy and threaten vision. Using a small sample size, they compared patient results from SS-OCT-A with that of other tests currently recommended for HCQ retinopathy screening and found that the imaging modality may be particularly effective in observing a patient’s condition.
Study participants included 10 patients undergoing HCQ treatment and 18 healthy controls, both groups with a mean age of 39. The HCQ group had treatment durations ranging from five to 15 years.
Results from SS-OCT-A showed that the HCQ group showed vessel density reduction in the 1mm central field, in the nasal and temporal subfields of the deep capillary plexus and in the 1mm central subfield of the choriocapillaris. Further observation of the HCQ group included an increased foveal avascular zone in the three capillary plexuses, a greater frequency of choriocapillaris flow voids and foveal choroidal thinning.
The following tests produced normal results in 100% of 20/20 eyes: best-corrected visual acuity, multifocal electroretinogram, SS-OCT B-scan and C-scan, automated visual field and fundus autofluorescence testing. SS-OCT-A allowed the researchers to observe choroidal thinning and flow abnormalities in the retinal capillary plexuses and choriocapillaris that may have otherwise been overlooked.
SS-OCT-A could reveal information about the status of a patient’s condition otherwise undetectable through traditional tests and imaging modalities, they concluded.
Forte R, Haulani H, Dyrda A, et al. Swept source optical coherence tomography angiography in patients treated with hydroxychloroquine: correlation with morphological and functional tests. Br J Ophthalmol. 2021;105:1297-1301. |


