 |
|
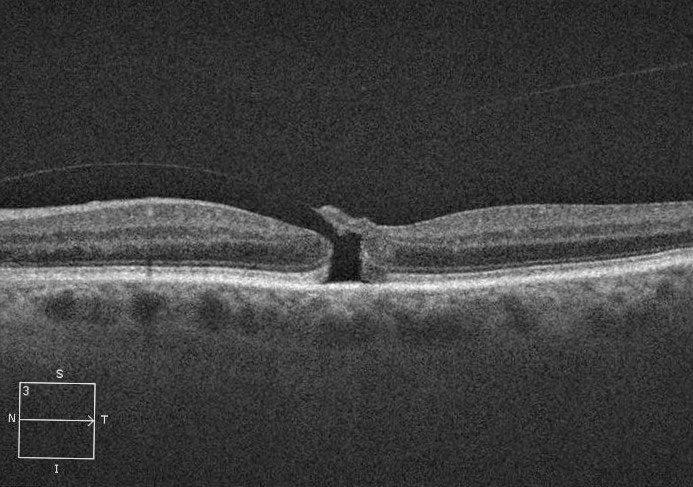
Assessing macular holes using various OCT parameters can help stratify timing of surgery. Photo: Diana Shechtman, OD. Click image to enlarge. |
Evaluating OCT scans can help inform clinicians about macular hole size and progression. A new study in the Retina journal revealed a few specific findings on the initial scan that may differentiate patients who are at greater risk for more rapid progression, which can have implications for determining surgery timing and urgency.
Using spectral-domain OCT, the following parameters were measured in patients with idiopathic macular holes on the nasal and temporal sides of the hole: minimal linear diameter (MLD), basal diameter and hole height. Scans and measurements were completed upon initial presentation and just prior to surgery. The researchers then calculated the rate of MLD change per day for each patient and completed a multivariable linear regression analysis to identify risk factors for MLD progression.
A total of 161 eyes (157 patients) were included in the study. In their paper published in Retina, the study authors identified four parameters significantly associated with MLD/day:
- MLD/basal diameter (wide basal diameter relative to MLD led to faster MLD progression),
- hole height asymmetry (larger absolute difference between nasal and temporal hole height led to faster MLD progression),
- days between scans (longer duration between scans led to a lower MLD/day rate, indicating a more rapid increase initially followed by a plateau) and
- relative to MLD quintile one, MLD quintiles three, four and five all led to a reduced MLD/day rate on multivariable regression.
Two of these findings weren’t reported in previous studies to have an association with increased MLD progression, including hole height asymmetry and a low MLD/basal diameter ratio. The study authors wrote, “Aside from comparing the largest idiopathic macular hole to the smallest (quintiles one and five), hole height asymmetry was the most significant factor in predicting the rate of MLD increase/day.”
In summary, the researchers noted in their paper, “Smaller mean hole height, higher hole height asymmetry, smaller MLD size (lower quintiles), lower MLD/basal diameter ratio (wide base relative to MLD) and shorter time between first and second OCT scan lead to significantly increased MLD increase per day.” They suggest that these parameters could help identify patients with faster-progressing macular holes that require more urgent surgical intervention.
Moussa G, Jalil A, Patton N, et al. Prediction of macula hole size progression based on baseline optical coherence tomography findings. Retina. November 17, 2022. [Epub ahead of print]. |


