 |
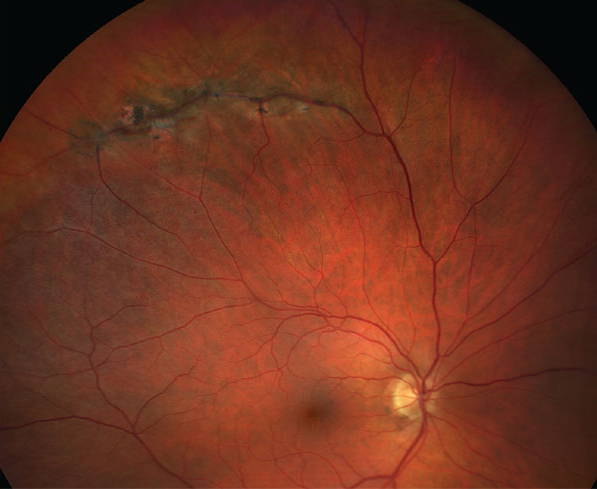
| Eyes with peripheral vitreoretinal abnormality and strong vitreoretinal adhesion at the time of full-PVD development will progress into RRD. In contrast, the eyes with peripheral vitreoretinal abnormality of which significant vitreoretinal adhesion had been released would stay attached even after full-PVD development. Photo: Jay M. Haynie, OD. Click image to enlarge. |
The extent of swept-source OCT coverage has widened to include the far retinal periphery, allowing more precise observation and better understanding of the peripheral retina. Despite the significant clinical burden of rhegmatogenous retinal detachment (RRD) and well-known associations with high myopia, standard guidelines for the preventive treatment of peripheral vitreoretinal abnormality—a catch-all term for things like vitreoretinal traction, lattice degeneration, retinal breaks and other atypical findings—have not yet been established.
A recent study in Ophthalmology evaluated the retinal peripheries of myopic eyes from young and asymptomatic participants using guided SS-OCT to assess the prevalence of peripheral vitreoretinal abnormality and retinal breaks and detachment and their risk factors. The research team found that none of the retinal detachment cases showed purely RRD features. Also, among the eyes with peripheral vitreoretinal abnormality, the risk of retinal breaks or detachment increased with age and when the eye showed multiple peripheral vitreoretinal abnormalities, especially linear lesions.
The researchers retrospectively reviewed the records of 1,966 eyes of 983 consecutive patients between 18 and 42 with refractive error in the spherical equivalent lower than zero diopters. Among these, 16.1% had peripheral vitreoretinal abnormality, and then 57.4% and 42.6% of eyes had focal and linear lesions, respectively. They noted that 4.7 % had full-thickness retinal breaks or detachment among participants with a mean age of 26.3 years.
The risk of peripheral vitreoretinal abnormality was increased with axial length of the eyes (odds ratio; OR=1.24), corneal astigmatism (OR=1.32), presence of discrete margins of different retinal reflectivity that indicate outer retinal disruption from abnormal vitreoretinal traction (OR=1.75) and posterior vitreous detachment (PVD) at posterior pole of the retina (OR=1.83).
Among eyes with peripheral vitreoretinal abnormality, patient age (OR=1.06), linear (OR=15.23) and multiple lesions (OR=3.432) were independently associated with the presence of retinal breaks or detachment.
“Considering that these eyes did not develop complete PVD nor vitreous liquefaction, the tractional force would be the main reason for retinal detachment in these young myopic eyes, in contrast to the RRD seen in elderly patients with vitreous liquefaction,” the researchers wrote in their paper. “The vitreoretinal interface status at the time of abrupt PVD would be the determinant factor for the development of sight-threatening RRD.”
The team pointed out that the first peak of RRD in the third decade of life in the East Asian population, where high myopia is prevalent, suggests that myopic progression is an independent risk factor for RRD apart from senile PVD. Therefore, they proposed that the prophylactic laser photocoagulation of retina recommendation should be differentiated for young myopes based on their ocular characteristics, encompassing asymmetric ocular expansion (AL and corneal astigmatism) and vitreoretinal interface (discrete margins of different retinal reflectivity and PVD).
“The treatment plan for peripheral vitreoretinal abnormality eyes should emphasize the greater risk of retinal breaks and detachment with increasing age and the presence of linear and multiple lesions,” they concluded in their paper.
Koh K, Tuuminen R, Jeon S. Ultra-widefield-guided swept-source optical coherence tomography findings of peripheral vitreoretinal abnormality in young myopes. Ophthalmology. November 14, 2023. [Epub ahead of print]. |


