 |
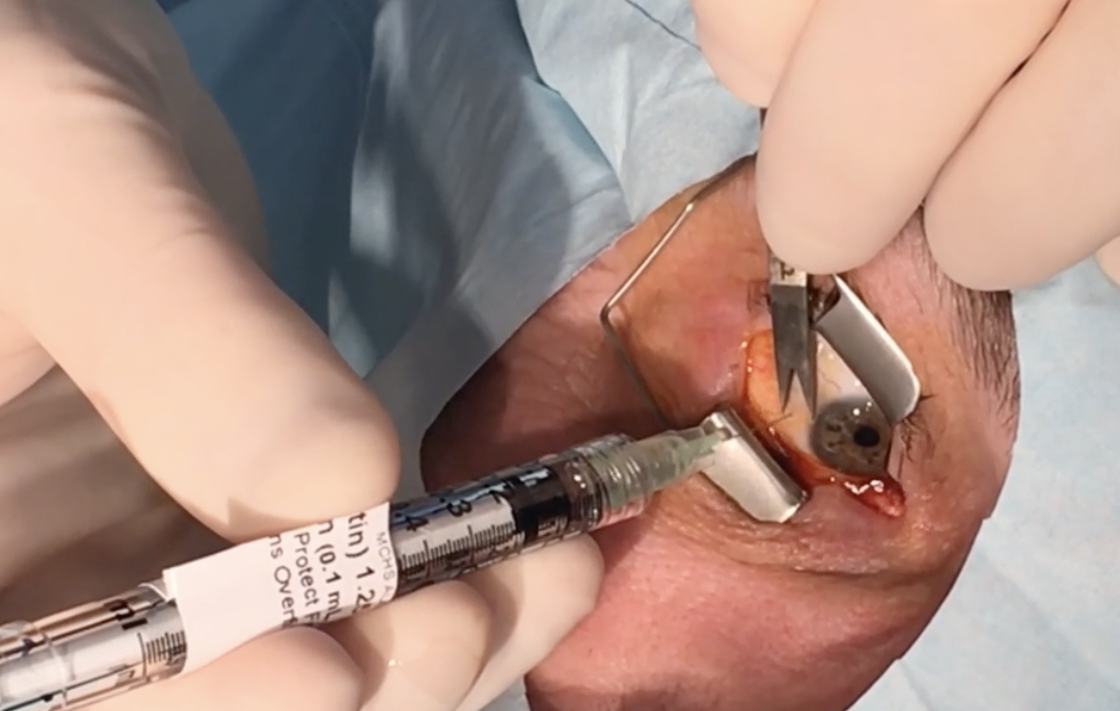
Anti-VEGF step therapy showed no difference in clinical outcomes when compared with Eylea monotherapy. Photo: Leonid Skorin Jr., DO, OD, MS. Click image to enlarge. |
Today, intravitreal anti-VEGF therapy can be used to treat a wide range of eye conditions, including diabetic macular edema (DME). But questions remain regarding which anti-VEGF agents and treatment techniques produce optimal outcomes when managing patients with this vision-threatening disease. Other important considerations when choosing the ideal treatment course for a patient are cost and insurance coverage.
It’s been known all throughout the anti-VEGF era that off-label use of compounded bevacizumab (Avastin) works just as well as several prominent—and pricy—branded therapies. A recent study published in The New England Journal of Medicine confirmed this in DME patients; those who received aflibercept monotherapy (Eylea; $1,941 per dose) had similar outcomes as patients treated initially with Avastin ($50 per dose) who then switched to aflibercept if their condition didn’t show sufficient improvement, a treatment approach known as step therapy.1
“Step therapy is a treatment approach often required by health insurers to control costs,” wrote the authors of a critical editorial on the study, also recently published in the NEJM.2 “It involves treating first with a lower-cost medication and, only if that proves ineffective, switching to another, more costly medication.”
The multicenter study gathered data from 54 clinical sites including a total of 270 patients (312 eyes) with DME involving the macular center and a visual acuity letter score of 24 to 69 (Snellen equivalent: 20/320 to 20/50). Eyes were randomly assigned to receive either 2mg of aflibercept or 1.25mg of bevacizumab. After 12 weeks, eyes in the bevacizumab-first group began switching to aflibercept therapy if criteria were met for insignificant clinical improvement. At two years, the mean change in visual acuity was recorded as the primary outcome measure. Safety and retinal central subfield thickness were also assessed at the end of the trial period.
During the two-year period, 70% of eyes in the bevacizumab-first group were switched over to aflibercept, with 54% transitioning within the first 24 weeks. The mean number of injections was 16.1 for the aflibercept-monotherapy group and 14.6 for the bevacizumab-first group. The mean improvement in visual acuity was comparable in both groups: 15 letters in the aflibercept-monotherapy group and 14 in the bevacizumab-first group. Retinal central subfield thickness was also similar between the two groups.
More patients in the aflibercept-monotherapy group experienced serious adverse events than the bevacizumab-first group (52% vs. 36%). Hospitalizations for adverse events were also more common in the aflibercept-monotherapy group (48% vs. 32%).
There is a lack of evidence on the efficacy of step therapy for various conditions, the authors of the editorial suggested. They went on to describe the design, methods and conduct of the study as “beyond reproach” but outlined several reasons why its findings need to be confirmed through further research.
“Perhaps the most important concern with the use of the bevacizumab-first strategy is the fact that the frequent follow-up of the participants in the first year of this trial exceeds what usually takes place in clinical practice,” the authors pointed out. They added that because patients with diabetes often see multiple providers, they may have increased difficulty adhering to frequent follow-up visits. “Missed or delayed follow-up visits in clinical practice could result in failure to identify vision loss at or near its onset and to implement a prompt switch from bevacizumab to aflibercept therapy,” they wrote.
Another aspect of the study design to take into consideration is the number of monthly injections patients received initially—six—before an automated algorithm was used to determine the need for additional injections. “This approach differs somewhat from the administration schedule of aflibercept recommended by its manufacturer, which includes injections every four weeks for the first five injections, followed by injections every eight weeks,” the editorial authors noted.
Jessica Haynes, OD, of the Charles Retina Institute in Tennessee, offered her take on the findings of the study. “A big thing to note is that this trial is not a direct comparison of the use of Eylea monotherapy vs. Avastin monotherapy in DME,” she said. “It does not show that Eylea and Avastin are equally effective in the treatment of DME. The previously reported protocol T study showed that those with moderate vision loss (worse than 20/50) had better visual acuity and retinal thickness outcomes with Eylea monotherapy than with Avastin monotherapy. What this trial is comparing is the initiation of treatment with Avastin, followed by switching to Eylea if there is inadequate treatment response.”
The important question that this study helped to answer, Dr. Haynes continued, was whether a delay in initiation of these more efficacious yet much more expensive drugs would make a difference for patients with DME. “Fortunately, the results of this study suggest that statistically, it does not,” she noted.
Will this research have an impact on protocols? “Most likely not, as step therapy is already required by most insurers,” Dr. Haynes answered. Lastly, she pointed out that the treatment approach may also have its downsides.
“I can attest from personal experience that it’s not fun trying to encourage patients month after month to come in and get injections when they don’t perceive a difference and the retinal thickness isn’t changing as you wait it out for approval to switch medications,” she said. “As doctors, our patients become like family. We want them to have the best treatments and the best outcomes. It can be taxing to go through the sequence of step therapy, as I know it is from their side too. However, it is reassuring that long-term outcomes may remain the same with either treatment strategy.”
1. Jhaveri D, Glassman AR, Ferris FL, et al. Aflibercept monotherapy or bevacizumab first for diabetic macular edema. N Engl J Med. July 14, 2022. [Epub ahead of print]. 2. Musch DC, Chew EY. Evidence for step therapy in diabetic macular edema. N Engl J Med. July 14, 2022. [Epub ahead of print]. |


